Synopsis
Minority patients in the New York City area are significantly less likely than whites to be treated at high-volume hospitals for cancer surgeries, cardiovascular procedures, and other services for which high volume and positive outcomes are related.
The Issue 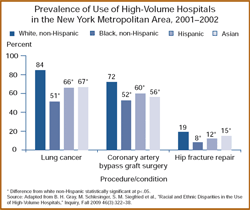
Racial and ethnic disparities in health care and treatment outcomes have been well documented in the United States, but the causes are poorly understood. Various issues may be involved, but a key question remains: are differences in the source of care a contributing factor? Hospitals that perform a large number of a given surgery or procedure can often provide better patient outcomes for that particular service. The authors of this study examined racial and ethnic differences in the patterns of use of high-volume hospitals for 17 services for which there is a relationship between high volume and positive outcomes.
Key Findings
- Black patients in the New York City area were significantly less likely than white patients to use a high-volume hospital for 16 of the 17 services examined between 2001 and 2002; Hispanics were less likely than whites to use such hospitals in 15 of the 17 services, and Asians less likely for 13 services.
- The differences were largest for cancer surgeries and cardiovascular procedures, averaging more than 20 percentage points between blacks and whites for 11 of these services.
- Blacks and Hispanics were more likely than whites to seek admission to a high-volume hospital for one of the 17 services examined: AIDS.
- Racial and ethnic differences were found not only for services for which admissions were largely unplanned (e.g., heart attack), but also for those generally planned in advance (e.g., hip-replacement surgery), challenging the idea that disparities are caused by how close patients live to hospitals.
- Disparities were exacerbated by the disproportionate numbers of minorities who were Medicaid and self-pay patients. However, within every insurance group—private insurance, Medicare, Medicaid, and self-pay—whites were more likely than minorities to use a high-volume hospital.
- Based on the research, as well as volume and outcomes, the racial and ethnic disparities found could result in 5 percent to 20 percent higher mortality rates for minority patients, as compared with whites, for common services, and 10 percent to 60 percent higher mortality rates for infrequent procedures.
Addressing the Problem
Even in a large, racially diverse metropolitan area, where high-volume hospitals are relatively accessible geographically to the entire population, researchers found evidence of racial and ethnic disparities. These findings raise important questions about the way that patients, particularly minorities, gain access to care. For example, many may prefer providers with whom they are familiar. The authors recommend policies that increase the number of high-volume hospitals among the providers of a given service. For example, New York's certificate-of-need program limited the number of institutions that perform common procedures like angioplasties, resulting in a majority of hospitals that perform a high volume of these procedures. "When the majority of patients use high-volume hospitals, there are fewer racial and ethnic disparities," the authors conclude.
About the Study
The researchers used patient discharge records from hospitals in New York City, plus adjacent counties, in the periods 1995–1996 and 2001–2002. The study focused on patients hospitalized for 17 services (five types of cancer surgery, six cardiovascular services, three orthopedic procedures, two prostate procedures, and admission for AIDS) with positive volume–outcome relationships. Demographic information indicated if patients were Hispanic, white, black, Asian or Pacific Islander, or other. The researchers controlled for socioeconomic characteristics, insurance coverage, and other factors. The Agency for Healthcare Research and Quality and The Commonwealth Fund supported the study.
The Bottom Line
Minority patients in the New York City area are significantly less likely than whites to be treated at high-volume hospitals for services for which high volume is associated with better outcomes, raising important questions about the ways in which racial and ethnic groups gain access to medical care.