Synopsis
A study of Medicare beneficiaries admitted to U.S. hospitals with congestive heart failure or pneumonia showed no definitive connection between the cost and quality of care, or between cost and death rates.
 The Issue
The Issue
Hospitals face increasing pressure to lower the cost of health care while at the same time improving quality. Some experts are concerned about the trade-offs between the two goals, wondering whether hospitals with lower costs and lower expenditures might devote less effort to improving quality. Critics wonder if the drive to lower costs might create a "penny-wise and pound-foolish" approach, with hospitals discharging patients sooner, only to increase readmission rates and incur greater inpatient use—and costs—over time. To examine the relationships between quality and cost, researchers analyzed discharge, cost, and quality data for Medicare patients with congestive heart failure and pneumonia at more than 3,000 hospitals.
Key Findings
- There were large variations in hospitals' costs for treating congestive heart failure (CHF) and pneumonia, with care for a typical CHF patient varying from $1,522 in the lowest-cost hospital to $18,927 in the highest-cost hospital. Costs of care for a typical patient with pneumonia ranged from $1,897 to $15,829.
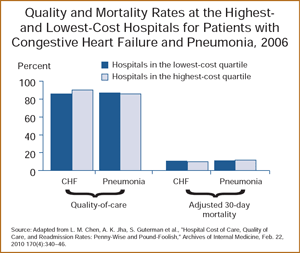
- Compared with hospitals in the lowest-cost quartile for CHF care, hospitals in the highest-cost quartile had higher quality-of-care scores (89.9% vs. 85.5%) and lower mortality (9.8% vs. 10.8%).
- For pneumonia care, the opposite was true: high-cost hospitals had lower quality-of-care scores compared with low-cost hospitals (85.7% vs. 86.6%).
- Hospital costs were stable over time: 63.6 percent of the hospitals in the highest-cost quartile for CHF in 2004 were still in the highest quartile in 2005, and 88.8 percent were in the two highest quartiles.
- The risk of readmission within 30 days for patients with CHF was greater at low-cost hospitals than at high-cost hospitals (24.7% vs. 22.0%), but readmission rates were similar among low-cost and high-cost hospitals (17.9% vs. 17.3%) for pneumonia.
- Compared with patients initially seen in hospitals with the highest costs, patients initially seen in low-cost hospitals had lower six-month inpatient costs ($12,715 vs. $18,411 for CHF; $10,143 vs. $15,138
for pneumonia).
 Addressing the Problem
Addressing the Problem
Understanding national patterns of quality and cost are a critical part of policymakers' efforts to improve the value obtained from health care dollars. In this study, researchers found limited evidence to support the "penny-wise and pound-foolish" hypothesis: that low-cost hospitals discharge patients earlier but have higher readmission rates and greater downstream inpatient costs. Compared with higher-cost hospitals, lower-cost hospitals had only slightly higher readmission rates for CHF but did not generate higher costs for either CHF or pneumonia. The authors suggest that future work might examine whether some of the variation in costs between hospitals may be related to structural differences, including type of governance, extent of health information technology adoption, and degree of vertical integration with outpatient practices.
About This Study
The authors conducted an observational cross-sectional study of more than 3,000 non-federal U.S. hospitals discharging Medicare patients for congestive heart failure or pneumonia in 2006. For each condition, the researchers examined the association between hospital cost of care and the following variables: process quality of care, 30-day mortality rate, readmission rate, and six-month inpatient cost of care.
Bottom Line
This study shows little evidence that low-cost hospitals discharge patients earlier but have higher readmission rates and incur greater inpatient costs downstream.