Synopsis
Employers are interested in features of the Small Business Health Options (SHOP) marketplaces, including the ability to compare health plans and get help administering them, but they are very sensitive to the cost of coverage. To increase the potential for success among SHOP marketplaces, it will be important to elicit buy-in from insurance brokers,who play a large role in managing benefits for small businesses, and to limit the number of small firms moving to selfinsure.
The Issue
Compared with midsize and large-group markets, the health insurance market for small groups (those with fewer than 50 members) has higher administrative costs, more volatile pricing, and lower-value products. The Affordable Care Act includes several provisions intended to strengthen this market, notably the establishment of the Small Business Health Options (SHOP) exchanges, or marketplaces. The state-based SHOP marketplaces will allow employers to compare and purchase plans and will perform administrative functions, such as billing and claims adjudication. The marketplaces opened for enrollment on October 1 for coverage beginning January 1, 2014. This Commonwealth Fund–supported study reports on the results of a survey that asked more than 600 small firms about whether they offer coverage, how they view SHOP features, and how the health reform law has affected them to date.
Key Findings
- Sixty percent of the small firms offered employee health benefits in 2012, and 41 percent of employees were enrolled in their employer’s plan.
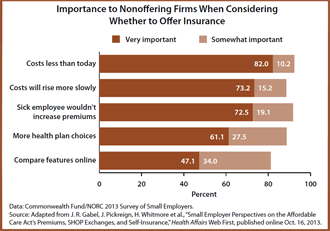
- Among firms not offering coverage, 75 percent pointed to cost as the most important reason why they do not. When asked what monthly premium for single-employee coverage they could afford, firms reported prices considerably below the current market average of $502.
- A majority (56%) of small-business owners who currently offer health benefits were interested in a key feature of the SHOP marketplaces: the ability to offer employees a choice of health plans while paying a fixed cost, with employees paying extra for choosing a more expensive plan.
- Other features of the SHOP marketplaces were also broadly appealing: 70 percent of respondents said they would be very interested in getting one bill and paying one check each month, and 68 percent would value the ability to compare plans’ costs, benefits, and physician networks.
- Eighty percent of firms offering coverage use brokers to help with tasks such as selecting health
plans and enrolling employees—functions the SHOP marketplaces can provide.
Addressing the Problem
Health insurance brokers act as de facto benefit managers for the vast majority of small firms, a business model that may be threatened by the SHOP marketplaces. The survey findings suggest marketplaces may need to elicit buy-in from brokers while demonstrating their value to employers. The survey also found that among firms using insurance brokers, one-quarter are considering self-insuring, or paying for health claims directly, and buying stop-loss coverage to protect against catastrophic costs. To avoid leaving fully insured markets (like the SHOP marketplaces) with greater risks and higher premiums, states or Congress could regulate or prohibit the sale of stop-loss coverage to small firms.
About the Study
Researchers at NORC at the University of Chicago interviewed CEOs, office managers, CFOs, and others at 604 randomly selected private firms with three to 50 employees. Among the 604 firms, 434 offered health benefits and 170 did not. For firms not offering coverage, the survey asked about their reasons, their experience in shopping for coverage, and factors that would make them likely to purchase it. Firms offering coverage were asked about their experiences in purchasing coverage, views of SHOP features, the effects of the health care law, and whether they had considered self-insurance.
The Bottom Line
Several features of the SHOP marketplaces have appeal for small businesses. Affordability will be a key consideration as small businesses decide whether to purchase coverage from the marketplaces.


