Synopsis
Patients with the knowledge, skills, and confidence needed to manage their health conditions are sometimes referred to as “activated.” Health care systems can use patient activation scores to help predict use of costly services, like the emergency department (ED). Knowing who is most at risk for incurring high costs enables systems to tailor their outreach efforts and better manage overall health care costs.
The Issue
Identifying patients who have a heavy disease burden and are likely to incur sizable costs is key to successfully managing health care spending. Currently, health systems rely on past medical claims data and diagnosis information to identify high-risk patients. Commonwealth Fund–supported researchers posit that this formula is missing an important element: patient activation. For a study published in Health Affairs, they theorized that knowing a patient’s activation level can help predict whether he or she will be likely to use costly services. The research team looked at information from patients enrolled with Fairview Health Services, an accountable care organization (ACO) in Minnesota.
Key Findings
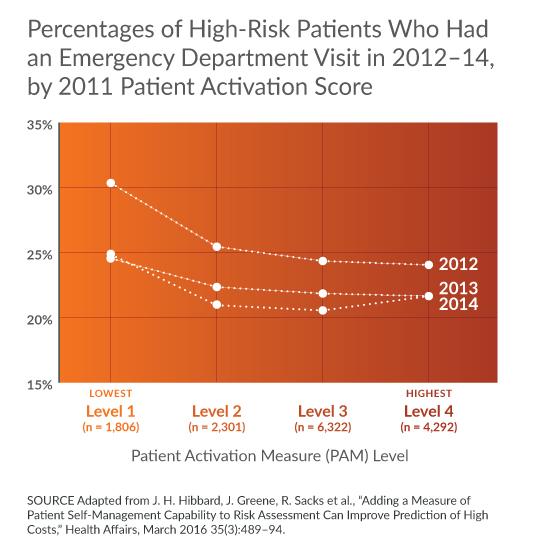
- High-risk patients were defined as those most likely to have high health care costs, based on their demographic profile, diagnosis, episodes of care, and pharmacy use. These patients were found to be twice as likely as low-risk patients to be at the lowest patient activation level. High-risk patients were three times as likely to have had an ED visit and 14 times more likely to have had a hospitalization as low-risk patients.
- Focusing on a subset of only high-risk patients, the researchers found those at the lowest activation level (1) were significantly more likely to have an ED visit and hospitalization compared with those at the highest level (4).
- Patient activation scores accurately predicted the use of costly services three years later. Patient activation scores were first measured in 2011. In 2012, hospitalization costs were 38 percent lower for people at the highest level of activation compared with those at the lowest level ($12,467 vs. $7,714). In 2014, the difference between the two groups was 29 percent.
- In 2012, ED costs were 37 percent lower for those at highest activation level versus the lowest ($1,126 vs. $711). In 2014, the difference was 28 percent.
The Big Picture
"Less-activated patients may benefit more from care coordination and care management services than patients who have equal disease burden but are more proactive about managing their health."
Being able to identify patients based on their activation level can help health systems segment their populations and use resources more effectively to support patients. For example, Fairview Health Services uses the patient activation measure to decide how intensely to follow and manage specific patients. Peace Health, a nonprofit health system in the Northwest, uses patient activation information to tailor its outreach. More-activated patients can be supported with Web-based and community resources, but less-activated patients may require support from health professionals.
About the Study
The study, conducted in collaboration with Fairview Health Services, involved 98,412 adult patients, of whom 14,721 were at the greatest risk for high health care costs. Fairview began routinely collecting patient activation measure results for its primary care patients in 2010. To measure utilization and cost of care, the study examined ED visits, hospitalizations, and total annual medical charges.
The Bottom Line
High-risk patients who are not adept at managing their health conditions are more likely to visit the emergency department or undergo a hospitalization. Health systems can use patient activation scores to more accurately assess risk, manage costs, and address patients’ needs.



