Summary: A Findlay, Ohio–based collaborative made up of local employers, physicians, and a hospital system pooled data from employee health claims to find variation in the quality and cost of treatment of their employees. To reduce the identified variation, the collaborative encouraged physicians to follow standardized treatment protocols, especially for chronic conditions such as hypertension and diabetes. The hospital system also redesigned its care practices for diabetic patients with a goal of improving outcomes and reducing lengths of stay. The collaboration has provided a venue for physicians to suggest changes to employer benefit programs that encourage patients to seek more preventive care and increase medication adherence. One employer in the collaborative went on to create a patient-centered medical home that has more than doubled cancer screenings while reducing emergency department use.
By Sarah Klein
Issue
Efforts to standardize care for specific conditions by encouraging providers to follow evidence-based guidelines are designed to reduce overuse of medical services and avoidable hospitalizations, as well as unwarranted emergency department use, which together contribute to rising health care costs and drain resources that might be better spent increasing access to care. Researchers have suggested as much as 30 percent of all health care spending is lost to overuse of medical services and other forms of waste. 1
To employers, such standardization is seen as a means of improving the value of services their employees receive and lowering costs—thus enabling employers to remain competitive with other businesses in countries with lower health care spending. While standardizing care for conditions for which evidence-based protocols exist has been shown to improve quality and lower costs, efforts to assess provider adherence to such protocols are hampered in part by the challenge of identifying variations among providers.2
Data that would provide a comprehensive view of such variation are dispersed among many sources, including large insurers, employers, disease management programs, pharmacy benefit programs, and government payers, all of which capture health claims data for discrete populations of patients. Aggregating those data is a challenge because providers and payers may use different methodologies to assess performance and disagree about the validity of the data. Collaborations among employers and providers to analyze such data and reach consensus about problems in care can expedite efforts to reduce variation by demonstrating to providers the importance of standardization and by demonstrating to employers and other payers the need for changes to benefit design. Despite these potential benefits, leaders of such collaborations say they are few and far between.
Organization and Setting
The Employer Data Project was formed in 2005 by a handful of employers operating around Findlay, Ohio, the local hospital system, and representatives of more than 300 local primary and specialty care physicians. Findlay is a largely rural community approximately 50 miles south of Toledo that has a population of 36,672, according to a 2009 estimate based on census figures.
Its providers treat patients from Findlay as well as those of neighboring counties, many of whom are employed by the participants in the collaborative, including Whirlpool Corp., Marathon Oil Corp., and Cooper Tire and Rubber Co. The majority of the employers are manufacturers with a stable base of employees, meaning they often pay employees' claims for decades rather than years and thus have an incentive to lower costs and improve care. Together the 11 employers represent approximately 23,980 employees, retirees, and their dependents, or one-third of the population of Hancock County (74,538), which includes Findlay.3
The hospital system, Blanchard Valley Health System (BVHS), consists of two hospitals with a total of 175 beds. The health system also operates a level 3 trauma center, two retirement homes, a hospice, and a durable medical equipment company. For the purposes of the Employer Data Project, which the group refers to as EDOC, the hospital system serves as both the organizing entity and a participating employer.
While the hospital system serves as the organizing body of EDOC, employers and physicians play an equal role in setting agendas for the group's thrice-annual meetings. The physicians, who are all volunteers who consider quality improvement an important goal, represent different specialties. Physician representatives say the multidisciplinary approach is essential to understanding and improving care coordination among specialists and primary care physicians.
The participating primary care and specialty care physicians tend to work in small practices of two to seven doctors, but many are represented by the Hancock Medical Group, a physician association.
Objective
EDOC creates a forum in which employers and providers can discuss the quality and cost of care in the community. In particular, local employers were concerned that the costs of care did not correspond to the value of services their employees were receiving. One local employer estimated that prior to the creation of EDOC, charges for some procedures were significantly higher than other communities in which it operated, a gap it attributed in part to the increased cost of attracting physicians to a rural community. The goal of EDOC was to explore other causes behind these costs and to reach a consensus on the most appropriate way to address them.
Process of Change
EDOC relies heavily on the analysis of health care claims supplied by the employers, which use different third-party vendors to process the claims of their employees. To aggregate the data from multiple sources and harmonize the approach to analysis, the participating employers hired The Delta Group, a South Carolina–based company that specializes in measuring the clinical and financial performance of health care organizations. To create a basis for comparison, the company uses a nationally recognized severity adjustment system and episode-of-care measures for discrete procedures and conditions, such as hypertension, diabetes, and knee replacement surgery. Such episode-of-care measures, which are severity adjusted, include total inpatient, outpatient, and pharmacy benefits and have been used by other employer groups to identify variation in the cost and quality of treating these conditions and procedures.
For EDOC, the task of creating a reliable profile of physician performance proved to be complicated because it required properly attributing care to physicians who changed roles, depending on the venue in which they worked (for example, some switched from emergency department doctors one day to primary care physicians the next.) The data from the third-party administrator of the health claims were sometimes problematic because they included claims for the Medicare population that were based only on secondary insurance, and thus excluded claims that involved Medicare, making costs look lower than they truly were.
Another problem was that the employers and the pharmacy benefit managers with whom the employers contracted also used different approaches to processing claims, and these had to be resolved before analysis could proceed. But once complete, the aggregated and de-identified data enabled employers to benchmark their cost and quality data against the larger group as well as national figures. It also enabled the group to focus on areas where there were wide variations in care.
One of the first conditions the group tackled was hypertension. While the data suggested wide variation in fees, these results had been distorted by inappropriate coding by physicians. Some had coded complex cases with co-morbidities as cases without co-morbidities, making the cost of care appear more expensive than expected. This also made the average cost of less complex cases higher.
A similar problem occurred with knee replacement surgery. For example, one physician coded the rehabilitation of a patient who had a catastrophic motorcycle accident solely as a knee replacement, which again led to a misstatement of costs.
To address this issue, EDOC spent six months educating physicians about the importance of proper coding, beginning with hypertension and gastro-esophageal reflux disease (GERD). In addition to providing training, EDOC sent a nurse employed by the Hancock Medical Group to audit medical charts in physician offices, which heightened physicians' awareness of the need for close blood pressure control. These efforts resulted in a reclassification of hypertension cases with and without co-morbidities.
To encourage adherence to evidence-based guidelines, physicians from EDOC also provided other local physicians with information about appropriate management and therapies. Physicians received reports showing their individual results, group practice results, and EDOC-wide results after each hypertension audit. The focus on hypertension enabled the physicians to point out a secondary problem: patients were not following up with their doctors on self-measured blood pressure results, which are essential to assess the effectiveness of prescribed medications. Some of the employers responded by increasing workplace blood pressure checks and asking their occupational nurses to record the results and encourage patients to communicate them to their physicians.
The focus on hypertension led to a 25.5 percent reduction in the combined costs of physician visits and hospital care from 2004 to 2007. Pharmacy costs fell more modestly; when pharmacy costs were added to physician and hospital care, the overall reduction fell to 11 percent. EDOC estimates that the employers as a group saved $528,000 over a two-year period in 2006 and 2007, or $121 per patient. The long-term benefit may be greater as the percentage of patients whose blood pressure came under control (defined as a rate below 134/85) increased by 26.8 between 2006 and 2008 (Exhibit 1). 
The group also examined emergency department visits, which were of great concern to employers. They discovered that physicians in the emergency department were arguably practicing defensive medicine, such as ordering magnetic resonance imaging when a regular X-ray and a physical exam would have sufficed. EDOC physicians rather than an employer's third-party administrator identified the problem and communicated it to the emergency physicians by educating them about the impact of extra costs on employers.
The physicians also noted that a large number of their colleagues in private practice were referring parents to the emergency department after hours to obtain treatment for their children's ear infections, rather than using an after-hours service to triage such calls. Making matters worse, the emergency staff were referring these patients back to primary care practices the next day to assess the effectiveness of the treatment, a practice that increased costs but provided little value as antibiotics for ear infections do not take effect for days, if not weeks.
EDOC explained to the physicians the importance of not referring such parents to the emergency department. Emergency department physicians were asked to tell parents to call but not visit the doctor's office the next day. To educate parents about the changes in practice, a physician wrote an article for the local newspaper and employers included similar messages in their employee newsletters. After the program was implemented, the rate of emergency department visits per episode of middle ear infections fell from 11.8 percent in 2006 to 10.8 percent in 2007.
EDOC also looked at diabetes care after data revealed that less than 20 percent of patients were receiving microalbumin tests, about the national average, according to LeRoy Schroeder, M.D., chair of EDOC's medical management committee. Dilated eye exams were performed less than 40 percent of the time. To improve adherence to evidence-based guidelines, EDOC provided training and implemented a registry system that enabled physicians, many of whom did not have electronic health record systems, to record the tests they administered and procedures performed through a Web-based system. EDOC also provided physicians with individual, group, and EDOC-wide results on adherence to evidence-based guidelines for diabetes care.
EDOC also worked to standardize treatment for diabetic patients who were hospitalized to ensure that the treating physicians used the most current methods for controlling blood sugar, which has an impact on patients' ability to recover from the condition or surgery for which they were hospitalized. Effecting this change required significant collaboration between hospital departments, such as nursing and dietary services, to ensure the proper timing of medication and meal services, as well as training for physicians. The program increased the percentage of diabetic patients with basal insulin orders, a proactive approach to controlling blood sugar as recommended by the American Diabetes Association, from 47 percent in January 2006 to 69 percent in April 2010 (Exhibit 2). 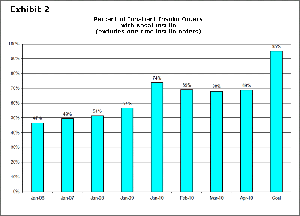
The EDOC physicians also urged employers to change their benefit plans to ensure diabetic patients received proper nutritional counseling and diabetes education and to provide incentives, such as low copayments for pharmacy benefits and physician office visits, for patients to increase medication adherence and patient engagement. Marathon Oil was an early adopter of the physicians' recommendations; it began covering nutritional counseling and providing additional coverage for physician visits, among other benefits. Other employers followed by providing full coverage for laboratory tests and office visits, as well as low copayments on diabetes medications.
As a result of its collaboration with providers and other employers, Marathon Oil also forged relationships with the local nursing and pharmacy schools to use their students at workplace clinics. They also learned of potential wellness strategies, such as the use of employer-sponsored cooking classes. "EDOC opened up a whole bunch of resources," says Larry McDaniel, Marathon's director of human resources services.
One employer, Whirlpool Corp., went beyond these efforts to create a patient-centered medical home program in 2010. To do so, it offered a modest (and undisclosed) payment to participating physicians to maintain a more comprehensive registry of care provided to patients with chronic diseases. The company also decreased copayments for patients seeking preventive care, including cancer screenings.
The hospital system quickly followed suit, creating a similar program for its employees that began in 2011. Between both employers, there is a total of 3,725 participants (including employees and their dependents) in the medical home program, the goal of which is to provide a comprehensive view of care and to use that information to help employees seek more preventive care. "The hospital system and Whirlpool are really trying to motivate the employee to take responsibility for their health," says Susan Pavlopoulus, Whirlpool's senior manager of global benefits.
Early results suggest that medical homes, coupled with value-based plan design, are an effective means of increasing delivery of preventive care. The number of physicals for adults and children who had medical homes more than doubled from 564 in 2009 to 1,200 in 2010. The number of mammograms for women age 40 or older increased by 64 percent over the same period, while the number of colonoscopies for patients age 50 and above tripled from 51 to 149. During this time period, the number of patients with one or more emergency department visits fell by 14 percent, to 210.
Whirlpool has also found that patients with a medical home are more likely to use their benefits for diabetes care than employees whose care is not provided through a medical home. Forty-seven percent of patients with a medical home make use of their medical benefits for diabetes care, compared with 35 percent of non–medical home patients, while 60 percent of medical home patients take advantage of pharmacy benefits. In contrast only 55 percent of patients in non–medical homes do the same. Whirlpool says it is too early to tell whether the medical home program has reduced costs, but it is monitoring this.
Next Steps
EDOC has also worked to standardize care for GERD in an effort to reduce GERD-related emergency department visits. That program has reduced such visits by 35 percent from 36 in 2005 to 22 in 2007, the most recent year for which results are available.
Going forward, the physicians in EDOC would like to focus on heart failure, lipid management, and chronic renal disease. They also would like to see greater use of value-based benefit design to support patient engagement.
Meanwhile, the medical home program is still evolving. Other employers may follow the lead of Whirlpool and BVHS if the results demonstrate cost savings and quality improvements.
Lessons
In offering advice to other communities, leaders of the EDOC program stress the importance of taking an open-minded, non-adversarial approach to meetings involving employers and providers, especially at the outset. The employers "have a lot of data and it is by no means all good," says the hospital system's CEO, Scott Malaney. But they did not use the data as a cudgel, he says. The employers felt it was important not to do so: "The biggest thing was for the doctors to be able to put themselves in our shoes and for us to be able to put ourselves in their shoes," says Robin Love, Marathon's benefits administration manager. McDaniel believes physicians also strengthened their arguments for value-based insurance design by stressing the financial benefit of proposed changes.
Providers that do work closely with employers can learn valuable lessons about business process improvement, Malaney says. His discussions with employers helped him recognize what manufacturers have long known: the importance of removing variation at the beginning of the process rather than the end. In health care, that means reducing variation in the primary care office.
Selecting physicians with the temperament and willingness to analyze a large amount of data was also critical, Schroeder says. Physicians participating in this program volunteered their time and did so because they had a strong commitment to quality improvement. Persuading other physicians to adopt their recommendations was made easier by pointing out that such programs will help the physicians prepare for the rewards and penalties associated with forthcoming pay-for-performance programs from government and other payers. "Boy did they recognize that word money," Schroeder says.
Implications
While the EDOC is making significant strides in reducing variation and improving quality, the program may be difficult to replicate in some large metropolitan environments, especially those with numerous hospitals in competition with one another. "We are a small enough community that we all know each other and communicate," says Stephen Orr, M.D., an ophthalmologist who serves on EDOC's medical management committee.
There are indications, however, that stakeholders with divergent interests can collaborate to achieve the goals of such programs. The Network for Regional Healthcare Improvement (www.nrhi.org) includes many multi-stakeholder organizations that bring competitors together to improve the health care and health status of patients. And in Findlay, BVHS took a leadership role in the EDOC even though EDOC programs were likely to reduce hospital revenues (by reducing MRIs in the emergency department and decreasing after-hours referrals to the emergency department by physicians in private practice.) BVHS believes its participation will pay off if the cost savings enable local businesses to expand and/or invest in the community.
Securing the participation of private insurers and government payers is also critical to creating a complete picture of provider performance and the impact of benefit design on outcomes. "We would love to have all payers," says Patricia Beham, BVHS's director of managed care. However, Malaney, the system's CEO, thinks insurers may be reluctant to share proprietary claims data.
Schroeder also expressed concern that some employers seem reluctant to change employee benefits, especially benefits that are popular with patients such as the use of chiropractic care for low back pain. Other employers have hesitated about paying for expensive hypertension drugs that may be needed or switching to over-the-counter medication for GERD. Schroeder sees this as a significant barrier: "They are going to have to go to value-based purchasing if they want to win."
The physicians and the hospital also face resistance from providers and as a result Malaney says some of the programs have hit a plateau, which EDOC members find frustrating. Reaching performance goals may require the group to take a more aggressive tack by publicly releasing provider-specific results, using more financial incentives, and/or excluding low performers who are outliers from contracts. "As you might imagine, clearly we aren't too excited about hurrying to get there," Malaney says. Using such levers may be a requirement to advance the program.
Still, many believe the early success will spur greater effort. "A project like this can demonstrate that as a group we can encourage each other to become more educated and motivated to meet these goals. We are far from hitting the goals of all those parameters, but we are a heck of a lot better off compared to the baseline data set," Orr says.
Contact: Patricia Beham, director of managed care, Blanchard Valley Health System, [email protected].
Notes
1. J. E. Wennberg. E. S. Fisher, and J. S . Skinner, "Geography and the Debate Over Medicare Reform," Health Affairs Web Exclusive (February 13, 2002) and E. Fisher, "More Care Is Not Better Care," Expert Voices, Issue 7 (National Institute for Health Care Management, January 2005). This estimate is based on a study of geographic variation in health care, which found greater spending for health care services does not yield better outcomes.
2. Institute of Medicine, The Healthcare Imperative: Lowering Costs and Improving Outcomes: Workshop Series Summary (Washington, D.C.: National Academies Press, 2010).
3. EDOC includes self-insured employers but at this stage does not include insurers.
This study was based on publicly available information and self-reported data provided by the case study institution(s). The Commonwealth Fund is not an accreditor of health care organizations or systems, and the inclusion of an institution in the Fund’s case studies series is not an endorsement by the Fund for receipt of health care from the institution.
The aim of Commonwealth Fund–sponsored case studies of this type is to identify institutions that have achieved results indicating high performance in a particular area of interest, have undertaken innovations designed to reach higher performance, or exemplify attributes that can foster high performance. The studies are intended to enable other institutions to draw lessons from the studied institutions’ experience that will be helpful in their own efforts to become high performers. It is important to note, however, that even the best-performing organizations may fall short in some areas; doing well in one dimension of quality does not necessarily mean that the same level of quality will be achieved in other dimensions. Similarly, performance may vary from one year to the next. Thus, it is critical to adopt systematic approaches for improving quality and preventing harm to patients and staff.


