By Mary Nowotny and Douglas McCarthy
Issue: Ninety million Americans "have difficulty understanding and acting upon health information," according to an Institute of Medicine report on health literacy.[1] Further, "low health literacy," according to an Agency for Healthcare Research and Quality (AHRQ) report on the subject, "is associated with several adverse health outcomes, including low health knowledge, increased incidence of chronic illness, poorer intermediate disease markers, and less than optimal use of preventive health services."[2]The Iowa Health System (IHS), recognizing that half of its patients and some employees were at risk for low health literacy, established a collaborative to improve patients' health literacy and, consequently, their health outcomes.
Objective: The aim of the IHS Health Literacy Collaborative is to "create a patient- and family-centered environment fostering effective communication that enables individuals to read, understand, and act on health care information." It seeks to create a "shame-free" environment in which patients and their families are comfortable asking for help with difficult information.
Organization and Project Leadership: The Iowa Health System (IHS) is affiliated with 10 large hospitals in seven cities—Sioux City, Fort Dodge, Waterloo, Cedar Rapids, Dubuque, Des Moines, and the Quad Cities (a metropolitan area that straddles the Mississippi River at Davenport). It also includes a network of 14 rural hospitals and 430 primary care physicians located in more than 30 Iowa communities.
Mary Ann Abrams, M.D., M.P.H., a health management consultant in the IHS Department of Clinical Performance Improvement, leads the Health Literacy Collaborative. The collaborative includes nurses, staff and patient educators, quality improvement staff, home health personnel, and members of New Readers of Iowa, a health literacy advocacy group.
Implementation Timeline: IHS initiated the Health Literacy Collaborative in 2003 with a series of hands-on workshops. In the workshops, which ran throughout 2004, participants shared information about health literacy and strategies for addressing the issue. The workshops drew on the Institute for Healthcare Improvement's Model for Improvement, the American Medical Association's train-the-trainer module, and the AMA's health literacy education toolkit. Further workshops were held in 2005 and 2006, involving more staff in the process, adding new information about health literacy, and reinforcing continuous improvement among those already trained in health literacy. The collaborative has continued to grow, with 12 rural groups joining the effort in July 2006.
Target Population: Groups participating in the collaborative chose the patient populations on which to focus their intervention, based on local needs. However, the target groups are not limited to patients with poor reading skills, as health literacy efforts are believed to be important for all patients. Says Abrams: "At some point, we're all vulnerable when it comes to understanding health-related information."
Key Measures: To assess the collaborative's impact, IHS selected five measures of patient–provider communication from patient satisfaction surveys. Baseline data were gathered using post-discharge mail surveys, from October 2003 to June 2004, and compared with data gathered after the implementation of health literacy interventions, from July 2004 to May 2006. Patients were asked:
- Did you receive an explanation about tests and treatments you received?
- Were you informed about medications you received?
- Did you receive instructions on caring for yourself at home?
- Did nurses keep you informed?
- Did physicians keep you informed?
- improving interpersonal communication between providers and patients;
- using tools to help ensure patients' comprehension of health information;
- simplifying health care situations such as check-in or health care referrals;
- developing simpler paperwork and educational materials; and
- empowering patients to ask questions.
Ask Me 3, a tool created by the Partnership for Clear Health Communication, recommends that patients ask their doctor, nurse, or pharmacist three questions: What is my main problem? What do I need to do? Why is it important for me to do this? Patients who still don't understand what they need to do are encouraged to ask their caregivers to explain the information again.
Teams within the collaborative have worked to clarify written materials, from patient admission forms to brochures on diabetes, heart disease, and pregnancy, among others. They participated in "Creating Reader-Friendly Print Materials" workshops, led by members of the Clear Language Group and involving patients, adult learners, and adult literacy program representatives. Hospital training programs were used to disseminate the modified patient materials throughout the system. Consent forms also were reviewed and revised, with input from adult learners, health literacy teams, the legal department, and clinical leadership. The new, reader-friendly forms prompt teach backs, instituting a National Quality Forum Safe Practice, developed with support from The Commonwealth Fund, to ask "each patient or legal surrogate to recount what he/she has been told during the informed consent discussion."
Early Results: Post-discharge surveys following the collaborative's health literacy interventions found an increase in the percentage of patients reporting that the information, instructions, and explanations provided during the care process were "very good" (Figure 1).
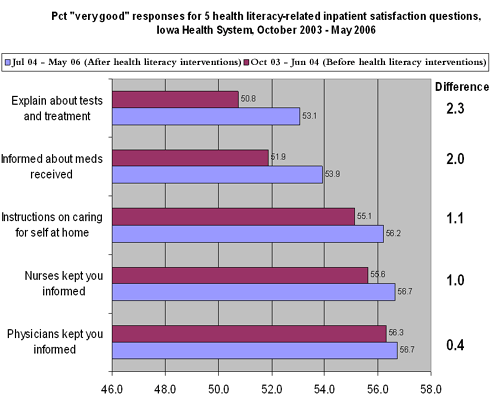
A 2005 pilot study at a Des Moines hospital found small improvements in 10 patient satisfaction measures related to health literacy after an Ask Me 3–based intervention was introduced.
The continued engagement of collaborative team members in workshops, training, and monthly conference calls suggests that they have learned to recognize and respond to the problems associated with health literacy. Abrams believes that a commitment to health literacy "is becoming hard-wired throughout the system." The IHS was one of eight hospitals and health systems recognized by AMA Ethical Force Program's Patient-Centered Communication Initiative for conducting innovative and exemplary communication programs.
Lessons Learned: Several factors were critical to the success of the Iowa collaborative, including senior leadership involvement, local literacy and evaluation data, personal stories about health communication, and feedback from its partners, including patients, adult learners, and literacy organizations.
Engaging busy physicians in the process, however, proved to be a challenge. Abrams recommends identifying early adopters and involving them in meaningful ways at the outset of the intervention. For example, physicians were willing to become involved in modifying the consent form because of its critical role in obtaining patient consent for surgery and other procedures.
Other guiding principles include:
- Though a comprehensive approach to low health literacy is recommended, the collaborative does not advocate routine health literacy screening as it might undermine efforts to create a shame-free environment in which patients feel comfortable asking questions or acknowledging that they don't understand information.
- Problems associated with health literacy can involve culture, language, and sensory processing. This calls for multifaceted interventions that address the care environment, interpersonal interactions between patients and providers, and written materials for patients and their families.
- Multiple points of care need to be involved in the intervention to generate traction among staff and providers, as its effectiveness is dependent on initiating and sustaining activity, from admission and discharge to medication changes, new diagnoses, procedures, and home care.
- Cultural competence plays a role in health literacy. The IOM report found that culturally influenced perceptions, definitions, and barriers have an impact on "how people interact with the health care system and help to determine the adequacy of health literacy skills in different settings."
To sustain these improvements, the Iowa collaborative has begun including health literacy concepts in job descriptions, new employee orientation, and competency standards for performance evaluation. Further, physicians are being trained to use teach backs with patients as part of an effort to see that health literacy is addressed at multiple points of care within the system.
Implications: "Improving health literacy is a cross-cutting priority that needs to be addressed at all levels to drive organizational changes," says Abrams. "As our population ages and as chronic diseases continue to affect more individuals, a greater focus on health literacy will be critical to prevention efforts and the drive to help people manage their own care."
Current performance measurement, however, may not capture efforts such as these to create more productive interactions between patients and providers. Quality indicators that measure whether heart failure patients received discharge instructions, for example, do not assess the quality of the communication process. AHRQ plans to develop a new module for the Consumer Assessment of Healthcare Providers and Systems (CAHPS) survey that measures how effectively health plans, hospitals, group practices, and clinicians address their patients' health literacy needs. In the meantime, hospitals can use the new CAHPS hospital survey and a new three-item Care Transitions Measure, recently endorsed by the National Quality Forum, to detect problems in patient–provider communication.
An increased emphasis on health literacy among health plans and government agencies, including the Centers for Medicare and Medicaid Services, is helping to drive change. The Joint Commission on Accreditation of Healthcare Organizations (JCAHO) has charged its Health Literacy and Patient Safety Roundtable with making recommendations for "stakeholders and policymakers to minimize the risks to patients with low health literacy and/or low English proficiency."[4] JCAHO also has teamed with the Iowa Health System on a National Institutes of Health grant proposal "to develop new evidence-based performance measures that can provide critical information about how well hospitals address the health literacy needs of patients."[4]
Health literacy is also being addressed in physician training, with three of the six core competencies for medical residents directly relating to physicians' communications with patients. In the future, competence in health literacy might play a role in physicians' maintenance of board certification.
Ultimately, health outcomes are the measures that count. Through its health literacy collaborative, IHS will continue to ask providers to consider the health literacy level of their patients, acknowledge health literacy deficits, and work to improve health communication. The system's leadership expects these efforts will improve health outcomes, save resources, and improve quality of care.
For Further Information: Contact Mary Ann Abrams at [email protected] or see the Iowa Health Literacy Collaborative Toolkit.
References
[1] Institute of Medicine (2004) Health Literacy: A Prescription to End Confusion. Washington, D.C.: National Academies Press.
[2] Agency for Healthcare Research and Quality (2004) Literacy and Health Outcomes. Evidence Report/Technology Assessment Number 87. AHRQ Publication No. 04-E007-2.
[3] H. Osborne (2005) In Other Words…How Do You Know? Measuring the Effectiveness of Health-Literacy Interventions. Boston Globe, On Call Magazine, January/February (Reprint).
[4] Joint Commission on Accreditation of Healthcare Organizations. Public Policy: Health Literacy and Patient Safety.