Summary: Concerned that it was wasting financial resources that would be better spent on health care, a Wisconsin-based health system embarked on an ambitious plan to reduce its energy use by more than 30 percent and to offset its remaining consumption with renewable energy projects, including one with a local brewery that will convert the brewery's waste into electricity. The health system's goal is to produce as much clean energy as it consumes by 2014, using techniques that have quick paybacks so that savings from reduced energy use can be used to support the institution's health care mission.
By Sarah Klein
Issue: Commercial office buildings are often criticized for wasting energy by using inefficient methods to keep occupants cooled and rooms well lit. But hospitals, which operate 24 hours a day, seven days a week, consume two-and-a-half times as much energy as office buildings and emit two-and-a-half times as much carbon dioxide, according to the U.S. Department of Energy.
Such consumption is not only bad for the environment and local residents, it also puts hospitals and health systems at financial risk when prices for natural gas and electricity rise, as they have since 2000. Leaders at Gundersen Lutheran Health System, a La Crosse, Wis.–based integrated health system, estimated that if recent price trends held true, the system's energy bills would rise $500,000 every year (Figure 1).1
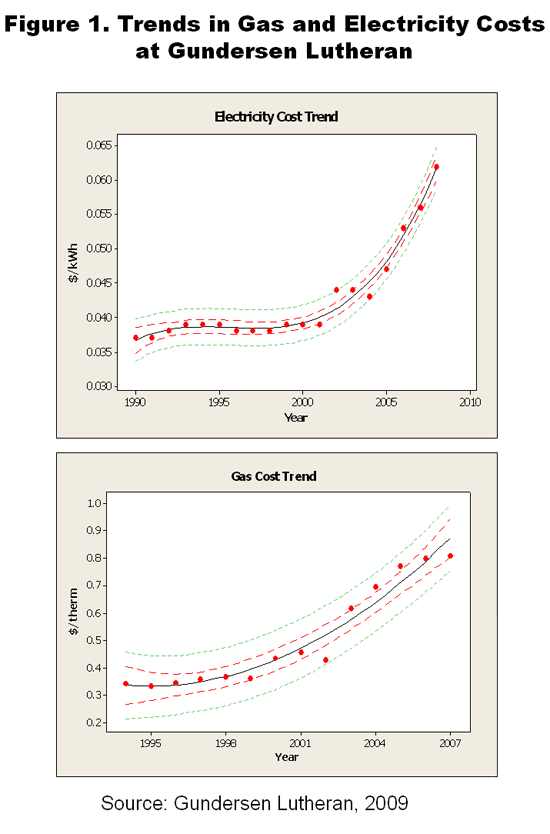
Concerned that the system was wasting resources that would be better spent on health care, Gundersen Lutheran's leaders set out to lower its energy use in a way that would save both energy and money. "A lot of organizations are buying carbon credits or buying green energy and they are paying a premium to do that. We don't believe that is the right solution because we are increasing the cost of health care if we do that," says Jeff Rich, Gundersen Lutheran's executive director of major projects and efficiency improvement.
Lowering health care costs, while improving community health, is part of Gundersen Lutheran's long-term strategy.
Objective: Gundersen Lutheran aims to be "carbon neutral" by 2014, meaning that it will not use more energy from fossil fuels than it produces from renewable sources by that year. To do so, the health system must reduce the demand for energy in its existing facilities by 30 percent and reduce the need for energy in new construction by 50 percent. Savings from those projects will be used to help finance renewable energy projects, which will offset the system's remaining energy use.
"Not only do we feel it is the right thing to do from an environmental standpoint, we think it will improve health," says Jeff Rich. "By dropping carbon emissions, we actually can improve the air quality and the health of the community, and we believe that it is a hedge against inflationary pressures we are seeing from energy prices. And we believe we can drop the cost of health care with this program."
Organization and Project Leadership: Gundersen Lutheran is a not-for-profit health system serving a tri-state region that includes parts of western Wisconsin, northeastern Iowa, and southeastern Minnesota. Created by the 1995 merger of the Gundersen Clinic and La Crosse Lutheran Hospital, it includes a 325-bed teaching hospital and 34 clinics, which provide medical, podiatry, behavioral health, eye, dental, and sports medicine services.
The health system's energy efficiency program, known as Envision, is led by Rich, a mechanical engineer, and Corey Zarecki, a chemical engineer. Both previously worked for Trane Inc., which manufactures heating and ventilation equipment for commercial and residential buildings. Tom Thompson, Gundersen Lutheran's sustainability coordinator, leads the health system's recycling, waste management, and environmental education programs.
Target Population: Gundersen Lutheran is located in the upper Midwest, an area of the country that experiences hot and cold temperature extremes, which creates a demand for air conditioning or heating year round. Despite high temperatures in summer months, the area lacks the consistently intense sunlight necessary to justify large-scale solar technology projects. The region does have other local resources suitable for renewable energy projects. Those include the Mississippi River, which can generate electricity through hydropower techniques, and sources of biomass such as forests and agricultural residues, which can be converted to fuel without creating greenhouse gases.
Plans are under way to construct a 156-bed critical care hospital using energy efficient glass, insulation, and ventilation equipment. However, many of the health system's existing facilities, including its hospital and the physical plant that supports it, were built more than three decades ago and need to be updated.
Key Measures: To determine the health system's energy use at the start of the project, the energy efficiency team analyzed more than 10 years' worth of site-specific utility bills. They found that the health system used 45 million kilowatt hours of electricity and 220 million cubic feet of natural gas, which cost $5 million in 2007 (the bill rose to $5.5 million last year). On a per square foot basis, this translates to an annual energy use of 250 to 235 kilo British thermal units (kBtu). The team believes that energy use in the new hospital can be reduced to 125 to 115 kBtu per square foot.
Process of Change: Gundersen Lutheran's energy efficiency program followed a phased approach, which began with small, easily achievable steps and progressed to more elaborate plans, which required time and capital to develop (Figure 2).
Figure 2
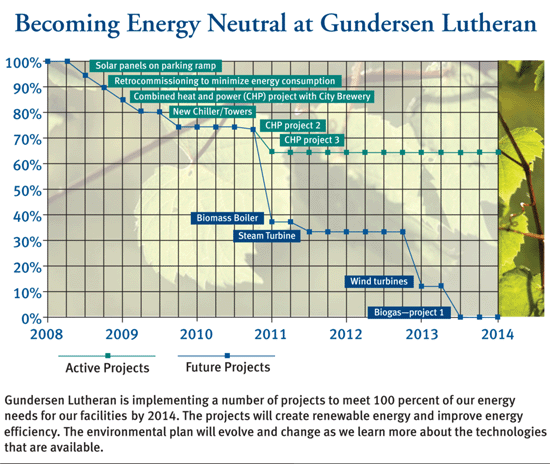
Source: Gundersen Lutheran, 2009
Phase I
The program began with an energy audit, which helped identify low- and no-cost ways to reduce energy use. Conducted in February 2008, the audit revealed a number of opportunities to save money and energy by optimizing the use of existing equipment. For instance, the health system switched from using three low-pressure boilers to create steam heat to warm buildings to using two high-pressure boilers, which were already running to sterilize equipment. The adjustment is saving the health system $64,000 per year.
The audit also showed that the clinic's chillers—which are used to cool campus buildings—would use less energy if a buildup of calcium carbonate were removed from their copper tubing. The calcium carbonate, which comes from the hard water supply, impedes heat transfer, increasing the amount of work the chiller motors must do. The addition of an acid feed—at a cost of slightly more than $2,000—has saved the health system more than $20,000 annually. Also, adding controls to the exhaust fans used to ventilate laboratories and pharmacies, and scheduling their use to ensure that equipment does not run unless it is needed, will save more than $30,000 per year.
Phase 2
The audit identified additional changes the health system could make that would require more significant investment but would reap greater savings over time. One example was upgrading all the lighting devices in the hospital and clinic. By switching to more efficient fluorescent lamps (from T-12 tubes to T-8) and ballasts, the health system got "better light for half the cost or less," Zarecki says. The new equipment will save the health system $250,000 per year in reduced energy costs. Because re-lamping will cost more than $1 million, it will take nearly six years for the health system to recover its initial investment. "The paybacks are a little bit longer than what you would expect a normal business to have. We have the kind of commitment where you can stomach some of those longer paybacks," Rich says.
Gundersen Lutheran is also updating its existing power plant to replace decades-old equipment with high-efficiency machinery. Doing so will lower maintenance costs and ensure that the power plant is properly sized to meet the needs of the new critical care hospital the system plans to open in 2012. The new cooling equipment, which will be operational in June, will save 800,000 kilowatt hours per year—the equivalent of 2 percent of the campuses' energy use in 2007. The health system is also considering installing a biomass boiler, which relies on renewable sources of fuel rather than natural gas. Such boiler projects are expensive (ranging in price from $1 million to $6 million, depending on size and features), but using one could save the health system 150 million cubic feet of natural gas, or $600,000 annually. Because the biomass boiler project would offset as much as 40 percent of the health system's energy use, "it could make a big impact on our energy neutral goal," Rich says.
The health system is already using some renewable energy. A parking ramp on the La Crosse campus, which opened in 2008, uses a limited number of solar panels to generate 73,000 kilowatt hours of electricity per year, enough to light the parking garage. A new data center, under construction to house the health system's servers, is designed to capture heat generated by the equipment and vent it to a chiller. That building will also have a white roof to reflect the heat of the sun. A new clinic in La Crescent, Minn., will use high-efficiency heating, cooling, and lighting systems and will have a white roof to reflect sunlight.
Another renewable energy project is a partnership with the La Crosse–based brewery City Brewing Co. LLC. The health system is installing equipment that will use microbes to convert the brewery's waste into electricity. Methane gas, which is produced when microbes digest the waste, will be used as fuel for the generator that produces electricity. The electricity will be sold to the local utility to offset the electricity used by the health system.
Gundersen Lutheran estimates that the equipment will produce 3 million kilowatt hours of electricity per year, enough to offset 8 percent of the electricity used annually at the health system's campuses in La Crosse and Onalaska. The brewery benefits, too. Without the system, it is forced burn off the methane gas in a flare, which bothers community residents, Zarecki says. "They were questioned all the time: Why just let it go into the atmosphere?"
The health system is also considering other approaches to generate clean energy, including using turbines to harness the kinetic energy of the Mississippi River, which flows past the hospital. The health system may also be able to use landfills to produce biogas, which can be converted into electricity and fuel. Payback on such systems varies from five to 15 years, significantly less than the 50 to 100 years it would take to recover money from large-scale photovoltaic projects.2
The health system also encourages recycling of its waste, though it is technically exempt from any requirement to do so because it falls under a recycling waiver intended for a local utility. The system recycled 29 percent of its waste in 2008, which amounted to 440 tons of paper, cardboard, metal, and batteries. The health system also encourages carpooling by offering preferential parking spots to employees who travel together. Its lab couriers use hybrid vehicles.
Financing: The majority of Gundersen Lutheran's energy plan has been self-financed. It has invested roughly $5 million in efforts to upgrade its existing equipment or make it more efficient and to build the system's renewable energy projects. Its strategy is to use savings from no- and low-cost energy reduction efforts to invest in energy renewal programs, which have a longer payback period.
The system hopes to obtain some federal money from the stimulus package for its efforts. But, to date, it has only received support from the state of Wisconsin's Focus on Energy program, which helps support energy efficiency efforts. That program typically covers 10 percent of projects costs, Rich says.
Early Results: By the end of 2008, Gundersen Lutheran had reduced its electricity use by 4 million kilowatt hours and its natural gas use by 16.5 million cubic feet, resulting in $409,000 in annualized savings. By the end of the second quarter of 2009, the health system expects to double those savings. By the end of 2009, it will have offset its energy use by 25 percent, saving the institution $1.25 million on expenses of $5 million. The health system is on target to reach its goal of being carbon neutral by 2014. To reach that goal, the health system may spend between $20 million and $30 million, but will recover that investment through lower energy bills within five to eight years, Rich says.
Lessons Learned: Gundersen Lutheran has moved quickly to establish an energy efficiency program. Less than a year after conducting its initial energy audit, the health system committed to spending $5 million on equipment to make its operations more efficient and to invest in renewable energy. The health system's plans have changed frequently, as the energy efficiency team discovered new technologies with faster paybacks. Because energy technology is rapidly evolving, such programs require flexibility. They may also require a willingness to pursue partnerships, as most health systems don't have the resources—such as rivers or landfills and other commercial waste streams—to produce clean energy on site.
Lowering energy use in new buildings requires collaboration among architects, engineers, and institutions, as those parties' designs and plans influence one another. To ensure that Gundersen Lutheran's new buildings meet the system's 50 percent energy use reduction target, it is planning to hold the architects and contractors to this goal through a written contract. The architects "sweat a little bit when I talk about it," Rich says. "They know hospitals can be kind of fickle about what they request and won't make the tradeoffs that are kind of tough. But if we don't set a target, we'll never get there and we [may] end up with a building that is less efficient than our current space and has a worse carbon footprint."
The energy efficiency team at Gundersen Lutheran only selects approaches that save the institution money. But, because energy costs make up only 1 to 2 percent of the health system's budget, the team is evaluating whether its time would be better spent on improving hospital operations. "We continually ask ourselves: should we be doing this?" Zarecki says. The health system believes energy independence is an important goal, one that resonates not only with community members, but also with politicians.
When "we announced our environmental program and the lead piece of it…[that] we're going to take waste methane gas from the brewery and we're going to generate electrical power to power the hospital -- people were so excited," says Jeffrey E. Thompson, M.D., Gundersen Lutheran's CEO. "I got 10 times as many calls and notes about that as I did about the fact that [we had gotten five stars from Health Grades for outstanding clinical performance]."
Such attention builds goodwill. "It's a great sign of stewardship," he says.
Implications: Energy efficiency programs have the potential to reduce health care system expenses. But programs such as these must be carefully structured to ensure that they do not increase health system expenses or energy use. Gundersen Lutheran's example shows this can be done with careful monitoring of energy use before and after the project. While energy efficiency programs are not a substitute for quality improvement in direct patient care areas, such efforts can be an important part of a health care organization's mission to set an example of corporate citizenship.
For Further Information: Contact Jeff Rich at [email protected] or Corey Zarecki at [email protected].
References
1. The health system had net income $34.7 million on net patient revenues of $732 million in 2008; this estimate is conservative because it assumes the health system will make no new hires, add no new buildings, and pursue no expansion plans.
2. Because the health system is tax exempt, it does not qualify for tax credits, which shorten the time it takes to recoup an investment in a solar project.
This study was based on publicly available information and self-reported data provided by the case study institution(s).
The aim of Fund-sponsored case studies of this type is to identify institutions that have achieved results indicating high performance in a particular area, have undertaken innovations designed to reach higher performance, or exemplify attributes that can foster high performance. The studies are intended to enable other institutions to draw lessons from the studied organizations' experiences in ways that may aid their own efforts to become high performers. The Commonwealth Fund is not an accreditor of health care organizations or systems, and the inclusion of an institution in the Fund's case studies series is not an endorsement by the Fund for receipt of health care from the institution.