Issue: Early this month, the National Committee for Quality Assurance (NCQA) released a revised set of standards to assess a physician practice's use of patient-centered, coordinated care processes. The Physician Practice Connections—Patient-Centered Medical Home program was developed in collaboration with four medical societies, the American Academy of Family Physicians, the American Academy of Pediatrics, the American College of Physicians, the American Osteopathic Association, as well as the Patient Centered Primary Care Collaborative, a coalition that includes large employers (see In Focus). These groups have agreed to use the NCQA program to recognize practices as patient-centered medical homes in demonstration projects nationwide, giving it the potential to fundamentally shape the redesign of primary care practice.
This case study examines the steps Hudson River HealthCare took to adopt the features of a patient-centered medical home.
Organization: Hudson River HealthCare, a federally qualified health center, provides care to nearly 50,000 patients at 14 sites in New York State. Its first site, in Peekskill, was opened by local residents and religious leaders in 1975 to meet the needs of the community's underserved population. Hudson River HealthCare is governed by a consumer-majority board, whose composition mirrors the health center's diverse patient population. It provides 200,000 health care visits annually to patients in Peekskill, Beacon, Poughkeepsie, Amenia, Dover Plains, Pine Plains, New Paltz, Goshen, Walden, Monticello, and Greenport, L.I. The health center offers a range of medical specialties, as well as key support services like health education and transportation.
Anne Kauffman Nolon, M.P.H., president and CEO, who has provided guidance to the health center for more than 30 years, and Paul J. Kaye, M.D., a pediatrician and Hudson River HealthCare's chief medical officer, lead the health center's improvement efforts.
Target Population: The health center's mission is to increase access to comprehensive preventive and primary care and improve the health status of patients in medically underserved communities. Its patients include the rural and urban poor and uninsured, pregnant women, migrants and immigrants, agricultural workers, the homeless, children and adolescents, the elderly, and those with HIV or substance abuse problems.
Key Measures: Hudson River HealthCare is accredited by the Joint Commission. It is recognized through the NCQA Physician Practice Connections program, an enhanced model of care that features open scheduling, expanded hours, and communication between patients, physicians, and staff. The health center participates in several national quality improvement collaboratives.
It currently tracks seven strategic aims and measures, with the goal of providing safe, timely, effective, equitable, patient-focused, accessible, and vital care (Table 1).
Table 1: Hudson River HealthCare's Strategic Aims and Measures | |
| Safe | Aim: 100 percent of patients have electronic health records (EHRs) Measure: EHR reports of encounters by provider |
| Timely | Aim: Same-day appointment available with own provider; average office visit cycle time of 45 minutes or less Measure: Time to third next available appointment; average cycle time |
| Effective | Aim: Improve health outcomes through preventive and planned care model Measure: 90 percent of two-year-olds are fully immunized; 90 percent of diabetes patients will have two HbA1c tests performed within one year, with at least three months between tests |
| Equitable | Aim: Eliminate differences in clinical care and health status between racial, ethnic, and socioeconomic groups Measure: No disparity by race or socioeconomic characteristics for all effectiveness measures |
| Patient-focused | Aim: 100 percent of patients recommend the health center to friends and family Measure: 100 percent of patients reply "Agree" or "Strongly Agree" to the following statement on the patient satisfaction survey: "I would recommend this practice to my friends and family." |
| Accessible | Aim: Serve 50 percent of center's target population Measure: Evaluate the health service penetration rate for underserved and other target populations in specified service areas |
| Vital | Aim: Achieve high productivity and staff satisfaction Measure: 20 billable patient visits per primary care provider per day; 90% staff retention |
Process of Change: Hudson River HealthCare's efforts to measure and improve patients' care experiences began with its participation in the Bureau of Primary Health Care's Together for Tots Immunization Project. Using Centers for Disease Control and Prevention software, providers measured immunization rates for two-year-old children every six months and received coaching on strategies to increase these rates.
In 1996, the health center worked with Roger Coleman, M.B.A., currently the general manager of Coleman Associates, to reengineer patient visits. Clinic flow was redesigned so patients could go directly to the appropriate clinical areas to receive care and did not have to wait in long lines to arrange payment. "We learned some principles but we were still struggling with how do we get more efficient and make it easier for patients to get in," says Kaye.
In 1998, the health center joined 19 other practices in the Institute for Healthcare Improvement's (IHI) Access and Efficiency Breakthrough Series, which introduced it to the concept of open access. Also called "same-day scheduling," it involves redesigning scheduling systems to enable physicians to offer same-day appointment to patients, regardless of the nature of their medical need. To do this, the health center has focused on reducing its "time to third appointment," a standard measure of access to care that indicates how long a patient must wait to be seen. This is the average length of time, in days, from when a patient makes a request for an appointment to the third next available appointment for a new patient physical, routine exam, or return visit. "The whole principle of open access becomes see the patients when they want to be seen, preferably today if that's what they want," says Kaye. A second component of the IHI series was efficiency, and the health center worked to decrease its average office visit cycle time, focusing first on its Beacon site and later across the health center's sites.
To maximize access for its underserved patients, the health center locates its sites in downtown areas, on public transportation routes, and in economically disadvantaged communities. It has evening, Saturday, and Sunday appointments, as well as a 24/7 answering service with physicians on call. Pediatric nurse practitioners also are available to take first calls from patients.
Other access initiatives include Casa de Salud, modeled after care systems in Mexico, which offers open appointments on Wednesday nights to meet the needs of a new Ecuadoran immigrant population; a mobile medical van to reach out to migrant workers; a mobile dental van to address patients' oral health needs; and co-locating social services, health plan enrollment, and other ancillary services at its sites.
Recently, Hudson River HealthCare has found that group visits with multiple health disciplines, a component of the patient-centered medical home model, are very effective for providing care to its population. These visits enable patients to obtain all the services they need under one roof, from dental care to diabetes education. As the visits are not reimbursed, the health center charges patients a $25 fee. "We're doing it even though we're losing money," says Kathy Brieger, vice president of quality operations.
In 2000, Hudson River HealthCare participated in the Bureau of Primary Health Care and Health Resources and Services Administration Diabetes II Health Disparities Collaborative. It learned how to use the Chronic Care Model, which outlines components of good care for chronic illness: self-management support, or providing information and systems to help patients and their families manage their illness; delivery system design, including organized visits and multidisciplinary care teams; decision support, such as reminders and standing orders; and use of clinical information systems, including disease registries, to improve patient care. The health center has since disseminated this knowledge to additional sites and other chronic conditions.
Also in 2000, the health center adopted a first-generation electronic health record (EHR) system.
Hudson River HealthCare participated in the Health Resources and Services Administration HIV Collaborative, beginning in 2002, and was one of five community health centers nationwide participating in the National Prevention Pilot Collaborative in 2004. A further effort was its participation in the Primary Care Development Corporation Redesign Collaborative, which helped leadership at the health center's two Poughkeepsie sites understand their role in transforming care. "The team that had been chosen to work on the whole process came together and started to talk our language," says Nolan. "They proved the case for redesign of the patient visit and their involvement in it."
Also, as part of the IHI Planned Care Innovation Community in 2005, Nolan and Kaye attended IMPACT network meetings and were exposed to IHI's white paper, written by James L. Reinertsen, M.D., "Seven Leadership Leverage Points for Organization Level Improvement in Health Care." (IMPACT is a membership network that brings health care organizations together to improve clinical outcomes, patient and provider satisfaction, and financial performance.) This further opened their eyes to "what you need to do to move an entire organization in the direction of quality care," says Kaye.
Results: By 2006, those involved in the various quality improvement collaboratives came to a similar conclusion. "You have to change the efficiency of your system to get enough staff time and enough resources to be able to do something different for every patient," says Kaye. The health center's leadership decided to bring staff members together for a day-long "harvesting meeting," at which they ranked the key changes that had to be made in order to transform the practice. These changes included:
- the need for chart preparation and visit planning;
- care team huddles, for example, regular meetings between members of multidisciplinary care teams;
- technology to support communication across systems of care;
- cross-training of staff members to enable them to perform more than one team function;
- EHR implementation;
- standing orders, or a course of treatments and tests each patient with a given diagnosis receives, unless a physician feels there is a reason to change or augment the order; and
- establishing a phone line that patients can call to refill prescriptions.
The health center, which has 493 employees, has ongoing staff development programs and measures staff satisfaction annually. Full-day training programs are an important component of this process, as they increase staff members' competency and satisfaction with their roles. Hudson River HealthCare has worked, through staff wellness and other programs, to reduce turnover rate. As a result, it has dropped from 25 percent in 2005 to 21 percent in 2006, and down to 11 percent last year. Its goal is to achieve 10 percent staff turnover annually.
Childhood immunization rates have been tracked continuously since 1995, and Hudson River HealthCare now has 12 years of improvement data for this measure (Figure 1).
Access has continued to be an important issue for the health center. Despite its efforts to offer extended hours and an after-hours call service, many patients still seek care in the emergency room. Hudson River HealthCare responded to this issue by having community care partners in several local emergency rooms to schedule follow-up visits and other appointments with patients at the health center sites. This effort to bridge outreach and primary care was recognized by a New York State Patient Safety Award in 2006.
Every two weeks the health center assesses the time to third next available appointment for each primary care provider, including physicians, nurse practitioners, and physician assistants, across its 14 sites. These efforts have reduced the average time to third next available appointment for an office visit to four days (Figure 2). In addition, six sites have attained the goal for this measure, achieving an average time of zero to one day. "We've paid a lot of attention to appointment access and there's a lot of work to be done because it really requires a total mind shift on the part of the staff. You have to be willing to lay back and let stuff happen," says Kaye. "It's a real culture change because it's around giving up control." Also, the center has found that open access has had a beneficial effect on its "no show" rate, reducing it to about 5 to 7 percent.
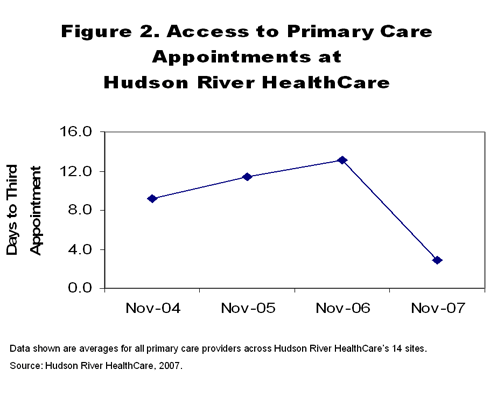
Its focus on efficiency, initiated through the IHI series, led to a reduction in the average office visit cycle time at its Beacon site from about 60 minutes to 39 minutes. Subsequent efforts across its sites have dropped the average length of a visit to about 50 to 60 minutes. (Some specialty visits, including prenatal care, can run as long as 90 minutes, raising the health center's overall cycle time.)
The health center has a PECS (Patient Electronic Care System) registry that it uses to monitor diabetic patients. As its diabetic population has grown from about 300 patients to nearly 2,200, the number of patients with poorly controlled diabetes has dropped (Figure 3).
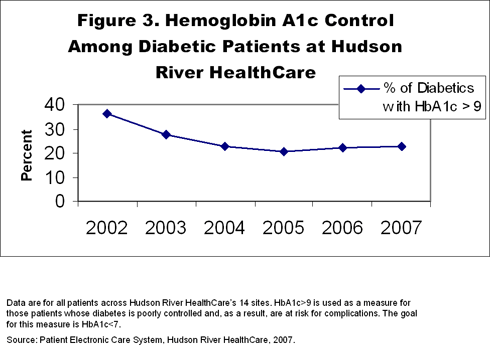
Ensuring there are enough staff to answer patient phone calls at peak times continues to be one of the thorniest issues affecting patients at many of Hudson River HealthCare's sites. "I don't think the problem is technological," says Kaye. "We're trying variable staffing and having an extra person who's working in the back to answer phones at peak times." Among other options, it has considered creating a call center.
Through its efforts to adopt an EHR, the health center learned that a poorly structured system can make it difficult for providers to improve quality of care. "If you get an alert that says, 'Mrs. Jones needs a mammogram,' in most of the [first-generation] EHRs, you've got four more steps to order the test," says Kaye. "When the doctor's in hurry, and they get six alerts, they're going to just close them all. You need a system that, when you click on the alert, it orders the mammogram." Hudson River HealthCare recently chose to adopt eClinicalWorks, which will have such public health and reporting functionality features built in to its next version, to be released this spring.
Implications: Hudson HealthCare learned about many elements of the patient-centered medical home through its participation in national quality improvement collaboratives. But, in order to transform the practice by matching patients to personal physicians, implementing open access scheduling, offering extended hours, and making other related changes, providers had to be brought on board. "Clinicians don't get excited by efficiency," says Kaye. "The buy-in of provider champions probably happened because we picked a clinical topic of relevance to our patients—diabetes."
It also found that it's important to educate all team members about the change process. For example, the front desk has a key role to ensure open access scheduling appropriately matches patients to their personal physicians. "It's often easier for the receptionist to put patients in the first available appointment they see on a screen, then to take the time to have a conversation with the patient about, 'Wouldn't you really like to see Dr. Jones?,'" says Kaye. "They've got to understand its importance and also be supported by providers."
Even though they're an important quality improvement tool, EHRs shouldn't come first. "One lesson I would pass on is that system change ought to precede technology," says Kaye. "People ought to know how they want to change their systems, have some insight into what they want to accomplish, and then put the technology in."
While EHRs will likely be necessary to achieve the highest patient-centered medical home recognition—level three—practice management systems will be sufficient for many practices to reach the first two levels of recognition, says Kaye. "Health centers will achieve level one if they are in compliance with [Health Resources and Services Administration] program expectations. If they've done a collaborative, and are using a registry to manage patients, I think achieving level two will not be difficult."
For Further Information: Contact Paul Kaye, M.D., chief medical officer, Hudson River HealthCare, at [email protected].