The U.S. Congress made good on its promise to deliver the initial building blocks for health care reform early in Barack Obama's presidency. This issue of States in Action takes an in-depth look at how states will be affected by the American Recovery and Reinvestment Act of 2009 (ARRA), known as the stimulus package, and the Children's Health Insurance Program (CHIP) Reauthorization Act of 2009.
American Recovery and Reinvestment Act of 2009
On February 18, President Obama signed into law a $789 billion economic stimulus bill, which was the result of a compromise between House and Senate Democrats and the three Senate Republicans who voted for the bill's passage. While the total cost was $31 billion less than earlier House versions and $49 billion less than earlier versions in the Senate, most provisions to boost state spending remained intact, including $87 billion to help states meet rising Medicaid costs.
"The proposal contains an unprecedented series of opportunities—as well as challenges—in the health arena," says Ray Scheppach, executive director of the National Governors Association. "States will receive immediate relief through enhanced federal funding for the Medicaid program to preserve coverage for low-income Medicaid enrollees and help stave off some troublesome cuts that would otherwise have been needed to balance their budgets."
The health-related provisions of the stimulus plan focus primarily on providing these temporary, additional federal funds for states for Medicaid, subsidized coverage options for the unemployed, and investments in health information technology. The direct impact of the ARRA on states is summarized below, though details on many aspects of the law will not will not be known until federal administrative action is taken.
Temporary Medicaid FMAP Increase. Currently, every state receives federal medical assistance percentage (FMAP) reimbursement that covers between 50 percent and 76 percent of Medicaid costs. The ARRA increases FMAP funding for a 27-month period beginning October 1, 2008 and ending December 31, 2010, with an across-the-board increase to all states of 6.2 percentage points and a similar increase for territories. In addition, a bonus payment structure that is based on increases in the state's unemployment rate will further reduce state financial obligations for Medicaid. For example, if the state's unemployment rate increases 3.5 percentage points or more in any three-month period, the state’s share of Medicaid match will be reduced an additional 11.5 percent. Overall, states are expected to receive an additional $87 billion in federal funds as a result of the FMAP increase, as shown in Figure 1.
The FMAP increase applies to Medicaid benefits, foster care, and adoption assistance. It does not apply to administration, CHIP, or Medicaid disproportionate share hospital (DSH) payments for hospitals that treat significant numbers of indigent patients. The enhanced FMAP rate may be adjusted up but not down—if a state is a high-unemployment state for any calendar quarter, then it remains a high-unemployment state for the purposes of calculating enhanced FMAP until July 1, 2010. To receive enhanced FMAP, a state's Medicaid eligibility standards must be no more restrictive than the standards that went into effect on July 1, 2008. The state also must agree not to deposit enhanced FMAP into any reserve or rainy day fund.
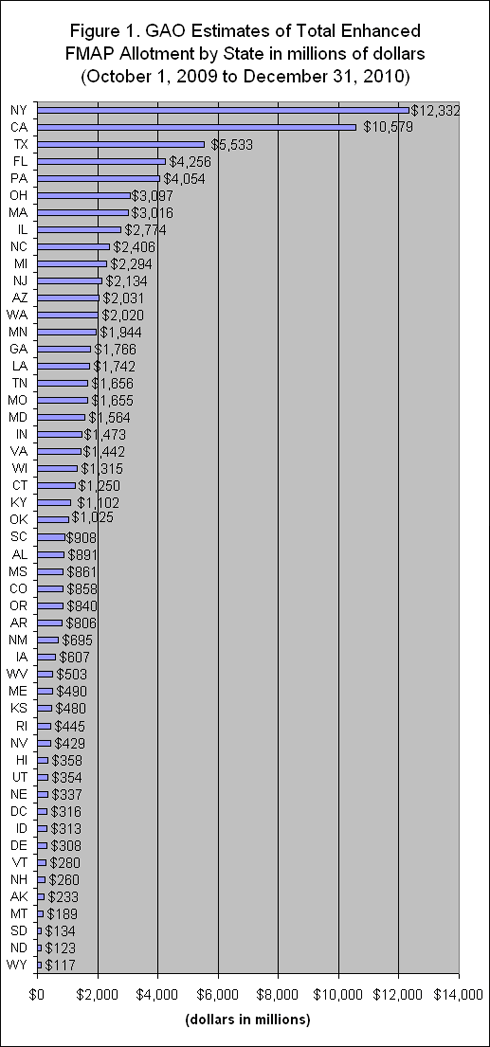
Note: Estimates are based on a February 4, 2009, GAO report that used a slightly higher across-the-board FMAP increase than the final conference agreement, which will result in slight changes in the final allocation among states (the total amount of spending is the same, $87 billion).
Temporary Medicaid DSH Increase. Medicaid provides special funding to hospitals that treat significant populations of indigent patients through disproportionate share hospital (DSH) programs. The ARRA increases states' DSH annual allotments for fiscal year 2009 by 2.5 percent and increases the allotments by 2.5 percent more for fiscal year 2010. After fiscal year 2010, states' annual DSH allotments would return to the funding levels determined under current law. States are expected to receive an additional $460 million in DSH payments.
Premium Subsidies for Unemployed Workers. Under the Consolidated Omnibus Budget Reconciliation Act (COBRA), laid-off workers can buy into their former employer's health insurance. But the premiums are often prohibitively expensive. A recent Fund analysis found just 9 percent of laid-off workers take up COBRA coverage.
To help people maintain their health coverage, the ARRA provides a federal subsidy that covers 65 percent of COBRA continuation premiums for up to nine months for workers who have been involuntarily terminated, and for their families. This subsidy also applies to health care continuation coverage for former employees of small employers, if states require it.
To qualify for premium assistance, a worker must be involuntarily terminated between September 1, 2008 and December 31, 2009 and have an annual income at or below $125,000 ($250,000 for families). The subsidy terminates upon offer of any new employer-sponsored health care coverage or Medicare eligibility. The final version of the bill eliminated a House-passed provision that would have let states offer temporary Medicaid coverage to unemployed individuals who are not eligible for COBRA.
Comparative Effectiveness Research. The ARRA appropriates $1.1 billion to accelerate the development and dissemination of research assessing the comparative effectiveness of health care treatments and strategies. The Institute of Medicine (IOM) is required to submit a report by June 30, 2009 that will provide recommendations for spending the comparative research funds. Based on the IOM recommendations, the Department of Health and Human Services (HHS), the Agency for Healthcare Research and Quality (AHRQ), and the National Institutes of Health (NIH) will spend the funds to "conduct, support, or synthesize research that compares the clinical outcomes, effectiveness, and appropriateness of items, services, and procedures that are used to prevent, diagnose, or treat diseases, disorders, and other health conditions." Funds can also be used to encourage the development and use of clinical registries, clinical data networks, and other forms of electronic health data collection that can be used to obtain outcomes data.
Extension of Moratoria on Medicaid Regulations. The bill extends a Congressional prohibition through June 30, 2009 on the implementation of regulations proposed by the Bush Administration related to hospital outpatient services, school-based administration and transportation, targeted case management, and provider taxes.
Health Information Technology for Economic and Clinical Health Act
The ARRA includes a $19 billion investment in health information technology (IT) and a number of related policy changes. The health IT provisions, collectively named the Health Information Technology for Economic and Clinical Health Act (HITECH), require that the federal government take a leadership role in developing standards for electronic health information exchange and strengthening federal privacy and security law. Unlike the FMAP increase and other one-time spending boosts in the economic stimulus package, HITECH policy changes set a long-term course for health IT adoption in the states.
State Planning Grants. HITECH provides new federal funding for states to expand the use of health information technology and accelerate the adoption of health information exchange. States are required to match $1 for each $10 of federal funds in 2011, $1 for each $7 in 2012, and $1 of state match for each $3 of federal funds in 2013 and beyond. To get the federal funds, a state must submit a strategic plan to HHS and receive approval. In its plan, the state must designate a not-for-profit grant administrator with broad stakeholder representation on its governing board. The grant administrator is required to consult health care providers, health plans, consumer organizations, health IT vendors, health care purchasers, public health agencies, and others as it builds its health IT infrastructure.
HITECH also provides funding to create Regional Extension Centers that will provide technical assistance to health care providers that are implementing health IT and health information exchange. HHS will competitively select regional centers; any U.S. non-profit organization can apply.
State Loan Programs. HITECH also offers new competitive grants to states for the development of loan programs to facilitate the widespread adoption of certified electronic health record technology. States are required to match not less than $1 for each $5 of federal funds for the loan program. The state may use the funds for low-interest loans to help providers purchase or enhance certified electronic health record technology, train personnel, or improve the secure electronic exchange of health information.
Provider Payment Incentives. Through Medicare and Medicaid, HITECH provides significant financial incentives to encourage doctors and hospitals to adopt and use certified electronic health records. Physician practices will be eligible for annual bonus payments in the range of $40,000 to $65,000 if they show that they are meaningfully using health IT, such as through the electronic reporting of performance on quality measures. Hospitals, federally qualified health centers, rural health clinics, children's hospitals, and others will also be eligible for extra funding through the Medicaid program. Incentive programs for both physicians and hospitals will continue for several years and be phased out after five years. Eventually, Medicare payments will be reduced for physicians and hospitals that do not use a certified electronic health record that allows them to electronically communicate with others.
Children's Health Insurance Program (CHIP) Reauthorization Act of 2009
On February 4, President Obama put an end to a two-year impasse between Congress and the Executive Branch when he signed the Children's Health Insurance Program Reauthorization Act of 2009. The CHIP reauthorization provides $32.8 billion in new spending through 2013 and is largely financed by a 61-cent increase in the federal tobacco tax. It will cover 6.5 million more children under Medicaid and CHIP.
"CHIP is a very successful program, ensuring millions of children have access to health care coverage," the National Governors Association's Scheppach says. "During this national economic and state fiscal crisis, now more than ever, CHIP reauthorization was essential to protect the health of our nation's most vulnerable children."
Financing. The reauthorization increases the federal CHIP appropriation from $7.0 billion in fiscal year 2008 to $10.6 billion in fiscal year 2009, and steadily increases the amount every year, up to $17.4 billion in fiscal year 2013. The national appropriation will be allotted to states based on the largest of the state's: 1) fiscal year 2008 federal CHIP spending, 2) fiscal year 2008 federal CHIP allotment, or 3) a projection of federal CHIP spending for fiscal year 2009. The largest of these three amounts will be increased by 10 percent and serve as the state's fiscal year 2009 federal CHIP allotment. Figure 2 shows the estimated growth in each state's CHIP allotment as a result of the reauthorization.
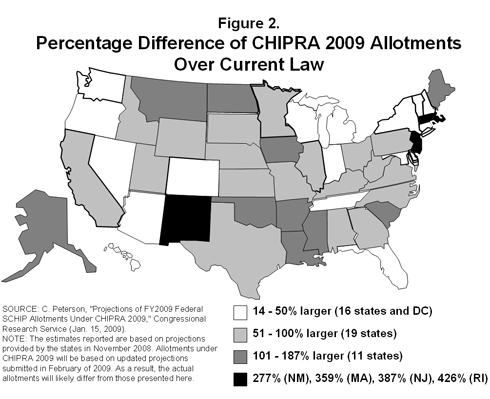
Eligibility. CHIP preserves state flexibility to decide the income eligibility level for children that need assistance in each state. Figure 3 shows current CHIP income eligibility levels by state. States will receive the CHIP matching rate on eligibility expansions to children in families with incomes up to 300 percent of the federal poverty level (FPL). For families with incomes above 300 percent, states will receive the lower Medicaid matching rate, with exceptions for New Jersey and New York, which already cover these children and will continue to receive a higher CHIP rate for families above 300 percent FPL.
CHIP covered 7.1 million children and 587,000 adults in fiscal year 2007. The Congressional Budget Office (CBO) estimates the reauthorization will increase CHIP enrollment by 5.7 million and Medicaid enrollment by 800,000, for a total of 6.5 million newly enrolled individuals in 2013. Overall, CBO estimates that of the individuals covered, 4.1 million (63%) would have been uninsured without the legislation and 2.4 million (37%) would have had private coverage.
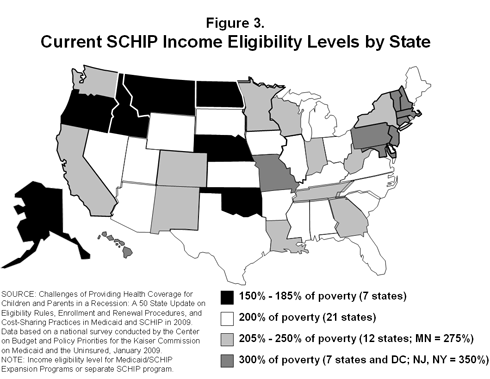
In addition to the eligibility changes described above for children who are U.S. citizens, the CHIP reauthorization also:
- gives states the option to cover pregnant women with CHIP funds;
- eliminates the federal five-year waiting period previously imposed on legal immigrant children and pregnant women in Medicaid or CHIP and requires a state that does not use a five-year waiting period to demonstrate that those enrolled provide evidence of lawful residence in the U.S.;
- extends Medicaid citizenship documentation requirements established by the Deficit Reduction Act to CHIP and provides states with a new option to document citizenship status by tapping into information that already has been gathered by the Social Security Administration; and
- bans any new waivers to cover parents with CHIP funds and phases out existing parent waivers in fiscal year 2011. (In 2008, 12 states—Arizona, Arkansas, Colorado, Idaho, Michigan, Minnesota, Nevada, New Jersey, New Mexico, Oregon, Rhode Island, and Virginia[1]—covered 335,000 adults in CHIP.)
Performance Bonus Payments. States that streamline their enrollment and retention procedures will receive a federal bonus payment for each child enrolled above a target level. The target level is based on fiscal year 2007 enrollment in Medicaid, adjusted over time by growth in a state's child population, plus 4 percentage points in 2009. The percentage-point add-on phases down to 2 percentage points after 2015. Bonus payments can vary from 15 percent to 63 percent of the average state cost of enrolling a child, with the higher percentage provided for the number of children enrolled in excess of 110 percent of the target level.
To be eligible for performance bonus payments, a state must implement at least five of the following practices for children in CHIP and Medicaid:
- 12-month continuous eligibility, elimination of the asset test;
- elimination of in-person interview requirements;
- use of a joint application;
- use of streamlined renewal;
- use of presumptive eligibility; and
- use of a new "Express Lane" option that allows states to apply eligibility determinations made by other public agencies to Medicaid.
The reauthorization also provides $100 million for a national enrollment campaign and state and local outreach and enrollment grants.
Benefits. The reauthorization requires CHIP plans to include coverage of dental services. It also now allows states to provide dental benefits as a wrap-around service for children enrolled in private coverage, a significant change from the current policy which prohibits any coverage for those already insured. Mental health benefits are not required but—if a state provides mental health or substance abuse services through CHIP—then the financial requirements and treatment limitations for those benefits cannot be more restrictive than those for medical and surgical benefits. CHIP plans that include Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) coverage would satisfy this new requirement.
Quality. The CHIP reauthorization establishes a new Medicaid commission, similar to the Medicare Payment Advisory Committee, to evaluate children's access to care and payment policies in Medicaid and CHIP. It includes $225 million for a new five-year quality initiative within HHS to develop, test, and disseminate child health quality measures; demonstration grants on quality and obesity prevention initiatives; creation of a model electronic medical record; and federal studies and state reporting on quality.
|