By Martha Hostetter
During the last decade, ambulatory practices, hospitals, and health systems have begun to adopt innovative management strategies and systems engineering tools to improve their health care processes. Using such approaches as the Baldrige National Quality Program, the Toyota Production System, or "Lean," and Six Sigma, health care organizations have been able to expand access to care (by reducing waiting times and increasing throughput); improve the quality and safety of care (by reducing variation and ensuring the delivery of evidence-based care); and reduce costs (by eliminating waste and increasing productivity).
There is considerable evidence that health care needs a new way of doing business. A 2005 report from the National Academy of Engineering and the Institute of Medicine, Building a Better Delivery System: A New Engineering/Health Care Partnership, found that "an estimated thirty to forty cents of every dollar spent on health care ... a half trillion dollars a year ... is spent on costs associated with: overuse, underuse, misuse, duplication, system failures ... and inefficiency." It also found that just over half of patients receive evidence-based care, and each year 98,000 patients die and 1 million are injured as the result of medical errors. The complexity of medicine has increased to the point where no one person can ensure it is delivered reliably and safely; instead, standardized approaches are needed to guide patients from provider to provider throughout the system.
Companies in other industries, such as Toyota, Motorola, and Boeing, have used process improvement tools to dramatically reduce errors and create highly reliable systems. For example, the commercial airline industry sees just 3.4 defects—or crashes—per million opportunities. But it's unclear whether such performance levels can be achieved in health care; healing bodies and flying planes are quite different propositions as no two patients are ever the same.
After a June 2002 trip to Japan, the leaders of Seattle's Virginia Mason Medical Center decided to aim for "zero defects" by following principles of the Toyota Production System—one of the first health care organizations to do so. Even a 4 percent defect rate at a hospital with 17,000 annual admissions and 16,000 surgical procedures could result in 640 surgical defects a year, 501 transfusion defects, and 40,000 errors in medication administrations. Virginia Mason implemented a Patient Safety Alert system, which requires staff who encounter a situation likely to harm a patient to "stop the line" and cease any activity that could result in further harm. Since 2002, this has resulted in more than 8,000 reported alerts—most due to communication breakdowns rather than mistakes on the part of individuals—as well as improved patient safety and fewer medical claims.
"Medicine is a highly complex system with a lot of human factors, including people who are sick, vulnerable, and often afraid," says Jennifer Graves, R.N., M.S., administrative director of nursing practice at Virginia Mason. "We're trying to focus on improving the production processes, so that we can increase the value-added time that providers can spend with patients."
Getting Started
While process improvement tools aren't new, many health care organizations have not taken advantage of them. Back in 2005, Building a Better Delivery System concluded that the health care sector has been slow to embrace systems engineering and management tools that have proven effective in manufacturing, telecommunications, transportation, and other industries. This is primarily because of health care's lack of financial incentives, regulatory frameworks that discourage innovation, a dearth of knowledge about these tools among health care leaders, and a widespread belief that health care is a unique industry.
Yet, there are signs that such tools are gaining a foothold in health care. Half of the applications made this year for the Baldrige National Quality Award came from health care organizations, a greater percentage than in previous years. There were just nine applications from health care organizations in 1999, compared with 43 this year. And according to Karen Feinstein, Ph.D., director of the Pittsburgh Regional Health Initiative (PRHI), which was formed in 2000 by a group of hospitals, insurers, and employers, a growing number of staff from community hospitals are enrolling in PRHI's Perfecting Patient Care University. Enrollees learn how to eliminate errors and streamline and improve care, following Toyota's principles. In previous years, the courses mainly attracted staff from large hospitals.
Mounting evidence of quality and safety shortfalls, growing demands for accountability and public reporting, and declining profits are among the factors pressuring health care organizations to change. But with so many brand-name systems and commercial consulting services available, how should health care leaders get started on improving their work processes?
Harry Hertz, Ph.D., director of the Baldrige National Quality Program, advises health care leaders to begin by creating an organizational profile. "Most organizations can say what they do, but not how they do it," he says. A Baldrige self-assessment clarifies "how you do business, how your leaders provide direction, strategize, engage the workforce, manage processes, serve customers, and reward excellence." In many cases, organizations focus on operational issues related to customer service, labor, and supply. Yet, increasingly, health care organizations are using process improvement techniques to improve the quality and safety of clinical care.
Denver Health and Hospital Authority, Colorado's primary safety net institution, chose "Lean" manufacturing, based on Toyota's approach, to redesign its delivery systems. "I became frustrated that we were doing things in the same way as when I was an intern almost 40 years ago—there are new drugs, new technologies, but the core health care processes are essentially the same," says Patricia Gabow, M.D., CEO of Denver Health. Gabow was attracted to Lean because it offers a philosophy as well as a set of tools to put it into place. "The philosophy fits with health care in general and Denver Health's mission in particular. At the core, Lean is about respect: the president of Toyota has said waste is disrespectful because it squanders scarce resources and asks workers to do work without value. I'd add to that that it's disrespectful to patients, since it asks them to undergo care processes with no value."
So far, Denver Health has trained 160 employees—from department heads to frontline staff—as "black belts," or experts in process improvement. Among other achievements, they have used Lean to enhance efficiency in primary care clinics and increase the number of patients who receive antibiotics within the appropriate time frame before surgery. Black belts are trained to use Lean tools in their everyday work and to submit monthly reports demonstrating how they do this.
Mapping Work Processes
Most improvement approaches emphasize the need to visualize work processes in order to reveal problems, rather than hide them through workarounds and business as usual. Many organizations hire industrial engineers to help them track their workflow, pinpoint bottlenecks, and develop streamlined processes. Tools such as queuing theory are often used to help predict the demand for services in settings such as emergency departments or open-access clinics.
Mapping workflow at Denver Health was crucial to gaining buy-in among staff. "Our chief of medicine said, 'The reason we're doing things this way is because it's the right way,'" says Gabow. "But the engineer was able to show that a nurse does hundreds of different, often disjointed tasks, each lasting a few minutes, and that a trauma resident walks up to eight and a half miles in a shift. These are processes you would never design from scratch." The chief of medicine is now a champion of the Lean approach.
ThedaCare, a health system based in Wisconsin, used "spaghetti charts" to track the paths that medical technicians, nurses, and other staff traverse in the operating room during surgery; Figures 1 and 2 show the paths before and after a redesign.
Figure 1
Figure 2
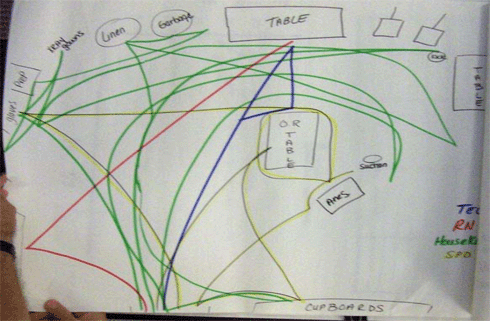 Source: ThedaCare Center for Healthcare Value, 2008.
Source: ThedaCare Center for Healthcare Value, 2008.
While much of medicine relies on clinical expertise and decision-making, many processes are repeated and highly predictable. Training staff to "do the right thing" can work for a while, but standardized processes are likely to prove more reliable and sustainable, as new nurses, residents, or other providers arrive. Tools such as checklists or color-coded supply systems are designed to make health care delivery as "error-proof" as possible.
Staff-Driven Changes and Patient-Centered Care
Many of the ideas for improving health care processes are developed on the ground level, among the employees actually doing the work. Most approaches follow some version of the Plan-Do-Study-Act cycle, which aims for rapid and continuous improvement.
"Virginia Mason's system is centered on the idea that staff closest to the work know the work best and can make improvements that benefit patients," says Graves. As a result of staff-driven changes, Virginia Mason reduced the time it takes to report lab results to patients by more than 85 percent and increased the amount of time nurses spend providing direct patient care from 35 to 90 percent.
Some have criticized systems such as Six Sigma or Lean for requiring specialized language or complex mathematical models. Derrick Suehs, chief quality officer at Syracuse's Crouse Hospital, says it's important to talk about health care improvement in ways that resonate with staff. At Crouse, staff are encouraged to report "Oh My God" moments—errors or near misses—and to apply the "momma test" to their work: If this patient were your momma, would you be happy with the care she's getting? "We try to use language that grabs at the heart," says Suehs. "What most places miss is the psychology around work—people have a need to achieve. You need to combine the technical improvement tools with the people side to make real change." To promote trust and accountability, Crouse created a "performance dashboard" to communicate clinical, administrative, and financial data to staff (Figure 3).
Figure 3

Source: Crouse Hospital, 2008.
Taking a cue from other industries, health care organizations have made customer service a focus of their improvement efforts. For example, "value-stream" maps are used to identify the steps taken to deliver a certain service, such as a clinic visit. Processes that bring value to patients are highlighted, while efforts that add time or resources without improving care are reduced or eliminated. Rapid Improvement Events in Denver Health's pediatric clinics led to medical office assistants and providers working in parallel, rather than sequentially—reducing the cycle time from 45 to 25 minutes while maintaining value for patients. As a result, clinics were able to expand patients' access to care by adding nearly two appointment slots for each provider.
The Bottom Line
Process improvements can bring significant savings by more efficiently using space or supplies, reducing labor costs, and increasing productivity. Denver Health, Virginia Mason, and Crouse Hospital have realized millions in savings without laying off staff or curtailing access to care.
For example, in 2001, Crouse Hospital filed for bankruptcy; by 2007, after making several changes based on Baldrige criteria, it had achieved an operating margin of 3.5 percent. One area that hospital leadership targeted was worker's compensation claims. Employees often were injured in the course of moving patients from gurneys to beds or operating tables. The hospital invested in "HoverMatts," which use a cushion of air to make it easier to lift and move patients. Within nine months, the hospital recovered $1.2 million from the lower costs of worker's compensation insurance and reduction in lost employee time that resulted; there have been no injuries among employees who use the HoverMatt technology.
The Pittsburgh Regional Health Initiative has enabled its members to gain a competitive advantage in the region. "We wanted to see if we could deliver the highest-value in health care, in terms of the best outcomes at a reasonable cost," says its director, Karen Feinstein. Participating providers have reduced infection rates and errors, improved clinical quality, and expanded access to care. In addition, says Feinstein, improving health care processes has been an effective workforce recruitment and retention strategy.
In some cases, improving work processes may curtail earnings for providers, for example if it means reducing the average length of stay for hospital patients. But, increasingly, health care leaders are weighing such concerns against the costs of unnecessary variation, inefficiency, and poor-quality care. Later this year, the Centers for Medicare and Medicaid Services (CMS) will stop paying for certain types of "never" events, including pressure ulcers and infections acquired during hospital stays. Further, moves by CMS and other payers to adopt performance-based payments or bundled payments for episodes of care or patient populations create incentives for hospitals to improve the effectiveness and efficiency of care.
Islands of Improvement in a Broken System
Improving health care processes at individual practices, hospitals, or health systems can have a big impact on the local level, as has been shown through the Pittsburgh Regional Health Initiative. But health care organizations need to be given far-reaching incentives to change, and there may be limits to how far engineering and management tools can go. In the end, many say, health care needs to be reengineered at the community, state, and national levels—something that will require financial incentives, changes to the regulatory and professional environments, and support for new infrastructure such as health information technology.
"Health care in America is not sustainable the way it is now," says Denver Health's Gabow. "We need to start developing different models."
During the last decade, ambulatory practices, hospitals, and health systems have begun to adopt innovative management strategies and systems engineering tools to improve their health care processes. Using such approaches as the Baldrige National Quality Program, the Toyota Production System, or "Lean," and Six Sigma, health care organizations have been able to expand access to care (by reducing waiting times and increasing throughput); improve the quality and safety of care (by reducing variation and ensuring the delivery of evidence-based care); and reduce costs (by eliminating waste and increasing productivity).
There is considerable evidence that health care needs a new way of doing business. A 2005 report from the National Academy of Engineering and the Institute of Medicine, Building a Better Delivery System: A New Engineering/Health Care Partnership, found that "an estimated thirty to forty cents of every dollar spent on health care ... a half trillion dollars a year ... is spent on costs associated with: overuse, underuse, misuse, duplication, system failures ... and inefficiency." It also found that just over half of patients receive evidence-based care, and each year 98,000 patients die and 1 million are injured as the result of medical errors. The complexity of medicine has increased to the point where no one person can ensure it is delivered reliably and safely; instead, standardized approaches are needed to guide patients from provider to provider throughout the system.
Companies in other industries, such as Toyota, Motorola, and Boeing, have used process improvement tools to dramatically reduce errors and create highly reliable systems. For example, the commercial airline industry sees just 3.4 defects—or crashes—per million opportunities. But it's unclear whether such performance levels can be achieved in health care; healing bodies and flying planes are quite different propositions as no two patients are ever the same.
After a June 2002 trip to Japan, the leaders of Seattle's Virginia Mason Medical Center decided to aim for "zero defects" by following principles of the Toyota Production System—one of the first health care organizations to do so. Even a 4 percent defect rate at a hospital with 17,000 annual admissions and 16,000 surgical procedures could result in 640 surgical defects a year, 501 transfusion defects, and 40,000 errors in medication administrations. Virginia Mason implemented a Patient Safety Alert system, which requires staff who encounter a situation likely to harm a patient to "stop the line" and cease any activity that could result in further harm. Since 2002, this has resulted in more than 8,000 reported alerts—most due to communication breakdowns rather than mistakes on the part of individuals—as well as improved patient safety and fewer medical claims.
"Medicine is a highly complex system with a lot of human factors, including people who are sick, vulnerable, and often afraid," says Jennifer Graves, R.N., M.S., administrative director of nursing practice at Virginia Mason. "We're trying to focus on improving the production processes, so that we can increase the value-added time that providers can spend with patients."
Getting Started
While process improvement tools aren't new, many health care organizations have not taken advantage of them. Back in 2005, Building a Better Delivery System concluded that the health care sector has been slow to embrace systems engineering and management tools that have proven effective in manufacturing, telecommunications, transportation, and other industries. This is primarily because of health care's lack of financial incentives, regulatory frameworks that discourage innovation, a dearth of knowledge about these tools among health care leaders, and a widespread belief that health care is a unique industry.
Yet, there are signs that such tools are gaining a foothold in health care. Half of the applications made this year for the Baldrige National Quality Award came from health care organizations, a greater percentage than in previous years. There were just nine applications from health care organizations in 1999, compared with 43 this year. And according to Karen Feinstein, Ph.D., director of the Pittsburgh Regional Health Initiative (PRHI), which was formed in 2000 by a group of hospitals, insurers, and employers, a growing number of staff from community hospitals are enrolling in PRHI's Perfecting Patient Care University. Enrollees learn how to eliminate errors and streamline and improve care, following Toyota's principles. In previous years, the courses mainly attracted staff from large hospitals.
Mounting evidence of quality and safety shortfalls, growing demands for accountability and public reporting, and declining profits are among the factors pressuring health care organizations to change. But with so many brand-name systems and commercial consulting services available, how should health care leaders get started on improving their work processes?
Harry Hertz, Ph.D., director of the Baldrige National Quality Program, advises health care leaders to begin by creating an organizational profile. "Most organizations can say what they do, but not how they do it," he says. A Baldrige self-assessment clarifies "how you do business, how your leaders provide direction, strategize, engage the workforce, manage processes, serve customers, and reward excellence." In many cases, organizations focus on operational issues related to customer service, labor, and supply. Yet, increasingly, health care organizations are using process improvement techniques to improve the quality and safety of clinical care.
Denver Health and Hospital Authority, Colorado's primary safety net institution, chose "Lean" manufacturing, based on Toyota's approach, to redesign its delivery systems. "I became frustrated that we were doing things in the same way as when I was an intern almost 40 years ago—there are new drugs, new technologies, but the core health care processes are essentially the same," says Patricia Gabow, M.D., CEO of Denver Health. Gabow was attracted to Lean because it offers a philosophy as well as a set of tools to put it into place. "The philosophy fits with health care in general and Denver Health's mission in particular. At the core, Lean is about respect: the president of Toyota has said waste is disrespectful because it squanders scarce resources and asks workers to do work without value. I'd add to that that it's disrespectful to patients, since it asks them to undergo care processes with no value."
So far, Denver Health has trained 160 employees—from department heads to frontline staff—as "black belts," or experts in process improvement. Among other achievements, they have used Lean to enhance efficiency in primary care clinics and increase the number of patients who receive antibiotics within the appropriate time frame before surgery. Black belts are trained to use Lean tools in their everyday work and to submit monthly reports demonstrating how they do this.
Mapping Work Processes
Most improvement approaches emphasize the need to visualize work processes in order to reveal problems, rather than hide them through workarounds and business as usual. Many organizations hire industrial engineers to help them track their workflow, pinpoint bottlenecks, and develop streamlined processes. Tools such as queuing theory are often used to help predict the demand for services in settings such as emergency departments or open-access clinics.
Mapping workflow at Denver Health was crucial to gaining buy-in among staff. "Our chief of medicine said, 'The reason we're doing things this way is because it's the right way,'" says Gabow. "But the engineer was able to show that a nurse does hundreds of different, often disjointed tasks, each lasting a few minutes, and that a trauma resident walks up to eight and a half miles in a shift. These are processes you would never design from scratch." The chief of medicine is now a champion of the Lean approach.
ThedaCare, a health system based in Wisconsin, used "spaghetti charts" to track the paths that medical technicians, nurses, and other staff traverse in the operating room during surgery; Figures 1 and 2 show the paths before and after a redesign.
Figure 1
The referenced media source is missing and needs to be re-embedded.
Figure 2

While much of medicine relies on clinical expertise and decision-making, many processes are repeated and highly predictable. Training staff to "do the right thing" can work for a while, but standardized processes are likely to prove more reliable and sustainable, as new nurses, residents, or other providers arrive. Tools such as checklists or color-coded supply systems are designed to make health care delivery as "error-proof" as possible.
Staff-Driven Changes and Patient-Centered Care
Many of the ideas for improving health care processes are developed on the ground level, among the employees actually doing the work. Most approaches follow some version of the Plan-Do-Study-Act cycle, which aims for rapid and continuous improvement.
"Virginia Mason's system is centered on the idea that staff closest to the work know the work best and can make improvements that benefit patients," says Graves. As a result of staff-driven changes, Virginia Mason reduced the time it takes to report lab results to patients by more than 85 percent and increased the amount of time nurses spend providing direct patient care from 35 to 90 percent.
Some have criticized systems such as Six Sigma or Lean for requiring specialized language or complex mathematical models. Derrick Suehs, chief quality officer at Syracuse's Crouse Hospital, says it's important to talk about health care improvement in ways that resonate with staff. At Crouse, staff are encouraged to report "Oh My God" moments—errors or near misses—and to apply the "momma test" to their work: If this patient were your momma, would you be happy with the care she's getting? "We try to use language that grabs at the heart," says Suehs. "What most places miss is the psychology around work—people have a need to achieve. You need to combine the technical improvement tools with the people side to make real change." To promote trust and accountability, Crouse created a "performance dashboard" to communicate clinical, administrative, and financial data to staff (Figure 3).
Figure 3

Source: Crouse Hospital, 2008.
Taking a cue from other industries, health care organizations have made customer service a focus of their improvement efforts. For example, "value-stream" maps are used to identify the steps taken to deliver a certain service, such as a clinic visit. Processes that bring value to patients are highlighted, while efforts that add time or resources without improving care are reduced or eliminated. Rapid Improvement Events in Denver Health's pediatric clinics led to medical office assistants and providers working in parallel, rather than sequentially—reducing the cycle time from 45 to 25 minutes while maintaining value for patients. As a result, clinics were able to expand patients' access to care by adding nearly two appointment slots for each provider.
The Bottom Line
Process improvements can bring significant savings by more efficiently using space or supplies, reducing labor costs, and increasing productivity. Denver Health, Virginia Mason, and Crouse Hospital have realized millions in savings without laying off staff or curtailing access to care.
For example, in 2001, Crouse Hospital filed for bankruptcy; by 2007, after making several changes based on Baldrige criteria, it had achieved an operating margin of 3.5 percent. One area that hospital leadership targeted was worker's compensation claims. Employees often were injured in the course of moving patients from gurneys to beds or operating tables. The hospital invested in "HoverMatts," which use a cushion of air to make it easier to lift and move patients. Within nine months, the hospital recovered $1.2 million from the lower costs of worker's compensation insurance and reduction in lost employee time that resulted; there have been no injuries among employees who use the HoverMatt technology.
The Pittsburgh Regional Health Initiative has enabled its members to gain a competitive advantage in the region. "We wanted to see if we could deliver the highest-value in health care, in terms of the best outcomes at a reasonable cost," says its director, Karen Feinstein. Participating providers have reduced infection rates and errors, improved clinical quality, and expanded access to care. In addition, says Feinstein, improving health care processes has been an effective workforce recruitment and retention strategy.
In some cases, improving work processes may curtail earnings for providers, for example if it means reducing the average length of stay for hospital patients. But, increasingly, health care leaders are weighing such concerns against the costs of unnecessary variation, inefficiency, and poor-quality care. Later this year, the Centers for Medicare and Medicaid Services (CMS) will stop paying for certain types of "never" events, including pressure ulcers and infections acquired during hospital stays. Further, moves by CMS and other payers to adopt performance-based payments or bundled payments for episodes of care or patient populations create incentives for hospitals to improve the effectiveness and efficiency of care.
Islands of Improvement in a Broken System
Improving health care processes at individual practices, hospitals, or health systems can have a big impact on the local level, as has been shown through the Pittsburgh Regional Health Initiative. But health care organizations need to be given far-reaching incentives to change, and there may be limits to how far engineering and management tools can go. In the end, many say, health care needs to be reengineered at the community, state, and national levels—something that will require financial incentives, changes to the regulatory and professional environments, and support for new infrastructure such as health information technology.
"Health care in America is not sustainable the way it is now," says Denver Health's Gabow. "We need to start developing different models."