Since it was first made available in the beginning of 2006, Medicare's Part D prescription drug benefit has succeeded in extending prescription coverage to the majority of beneficiaries who previously lacked it. But a major study involving more than 16,000 U.S. seniors finds that the new benefit provides less protection than private insurance coverage. Moreover, it has failed to reach many of the elderly who could benefit most.
Writing in the online edition of Health Affairs, researchers reported that enrollees in Part D plans pay considerably more out-of-pocket for their coverage than those with either employer-sponsored coverage or Veterans Administration benefits, and they are more likely to skip medications because of those costs. And too many low-income seniors, the researchers say, are still without drug coverage—despite the availability of a subsidy designed to defray their out-of-pocket costs.
The study, conducted by Tufts-New England Medical Center with support from the Kaiser Family Foundation and The Commonwealth Fund, amounts to a progress report on the biggest expansion of the Medicare benefit package since the program was founded in 1965.
More Have Drug Coverage, But Costs Are Concern
The Medicare drug benefit seems to have achieved its initial goal: increasing the number of seniors with drug coverage. According to study findings, fewer than 10 percent of seniors lacked prescription coverage in the fall of 2006, compared with one-third who said they had no drug coverage in 2005.
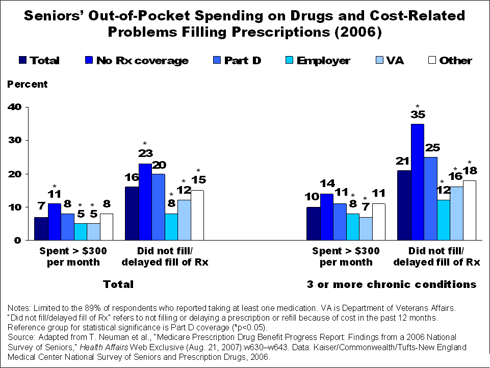
Not surprisingly, seniors without any prescription coverage at all reported higher out-of-pocket spending, with cost-related "nonadherence"—forgoing or delaying the filling or refilling prescriptions—being more common among this group than among seniors who either are in Part D plans or have other sources of private or public coverage.
But seniors in Part D plans had higher rates of potentially burdensome out-of-pocket drug spending than those enrolled in employer-sponsored plans or coverage through the Veterans Administration: 8 percent reported spending at least $300 on their medications in the most recent month, compared with 5 percent of those with employer-sponsored or VA coverage. Moreover, rates of cost-related nonadherence among Part D enrollees were about twice as high as they were for seniors with employer plans or VA benefits.
Trouble Reaching Low-Income Seniors
Based on analysis of the survey responses, elderly Americans who lacked drug coverage in 2006 fell into two groups: those who are potentially vulnerable but hard to reach—including people age 75 and older, African Americans, individuals with income at or below 150 percent of the federal poverty level, those with no education beyond high school, or those living in rural areas—and seniors in good health.
Perhaps most troubling is the high number of impoverished seniors who are eligible for but not enrolled in Part D's low-income subsidy program. Despite the effectiveness of the subsidy—according to the survey, rates of out-of-pocket spending in excess of $100 and $300 per month were significantly lower for seniors receiving the subsidy than for other Part D enrollees—an estimated 3.4 million to 4.7 million eligible beneficiaries are not receiving it. Only half of the low-income seniors who did not receive the subsidy said they were aware of the program, a clear sign that the government's education and outreach efforts need to be improved.
"Low-income subsidies really make a difference for those seniors who receive them, but there are still millions of low-income seniors who are eligible for this help but not getting it," said Tricia Neuman, Sc.D., the study's lead author and a vice president at the Kaiser Family Foundation.
In an editorial discussing the survey results, the New York Times (Sept. 3) acknowledged Part D's achievements while noting that it has "fallen short in providing subsidies to low-income Americans, in protecting people from high out-of-pocket costs, and in matching the benefits offered by other private and public sources of coverage." Echoing the study's authors, the Times concluded, "These shortcomings will need attention as the program rolls forward."