Summary: Health reform strategies such as creating patient-centered medical homes depend on an actively engaged and empowered patient population for success. To be fully engaged, patients must understand their conditions and what is involved in self-care. Researchers, health plans, and providers have been developing innovative assessment and self-management tools to help patients gain information and knowledge needed for effective self-care. Extending these tools to providers and patients nationwide will require considerable staffing resources, potentially different reimbursement policies, and other modifications to meet the needs of diverse populations.
By Deborah Chase
The Patient Protection and Affordable Care Act includes several provisions that increase the role of patients in managing their care. These include expanding the use of primary care medical homes, enhancing consumers' role in choosing health insurance, and publishing data to help patients make informed choices. For these initiatives to be successful, patients must understand their role in improving health outcomes and have the tools needed to make improvements. Health plans, delivery systems, and researchers have been developing patient engagement strategies over the past several years that successfully increase patient education, knowledge, and confidence—all of which have been shown to improve self-management of care.
The need for patients to be involved in their care has increased in recent decades because patients are living longer and in some cases handling greater disease burdens. Patients must navigate complicated health care systems and make multiple choices about their clinical care, including how to monitor and manage their own conditions. The Centers for Medicare and Medicaid Services has attempted to help consumers make better choices through its Hospital Compare Web site, as has the National Center for Quality Assurance with the publication of health plan comparison data. In addition, many state and local governments have focused on explicitly linking quality data to patient engagement strategies.
The Center for Advancing Health, a Washington, D.C.– based research and policy organization aimed at increasing consumer's involvement in health and health care, defines patient engagement as "actions individuals must take to obtain the greatest benefit from the health care services available to them."[1] Patients must be involved in the process of care, and their behavior is as important to health outcomes as provider or policy actions. The center has published specific guidelines on how patients should engage with providers in patient-centered medical homes. Strategies to promote patient engagement have resulted in greater self-reported medication adherence among diabetics, reduced medical costs and hospitalizations, and improved physical and mental health status of patients.[2] This issue of Quality Matters describes recent innovations that help patients engage in their care. Each operates on the premise that patient engagement is key to reaching quality goals.
Web-Based Survey Promotes Patient Engagement
John Wasson, professor of community and family medicine at Dartmouth Medical School, and his colleagues have created a Web-based tool (www.howsyourhealth.org) for patient self-assessment that provides "real-time" patient-reported data on functioning, overall health, and chronic conditions. The tool also enables patients to assess their confidence in managing and understanding their disease. Physicians can ask patients to complete the online health assessment before their next appointment, and the results are then sent to the physician's office. Patients receive a summary of findings and a list of resources for more information on their specific conditions. The summary also offers patients a list of questions to ask their doctor during the next visit.
Wasson believes that the information collected using the online tool is critical to building successful patient-centered medical homes because it identifies what is important for a specific patient. "We wanted to build a system where doctors and patients were on the same page," he says. "When you have the same information, the physician and patient can act more effectively on the patient's behalf." Information collected shows doctors which patients need coaching on self-management and who may need help to connect to additional resources. The tool also includes its own follow-up options (such as links to educational materials). If respondents opt for the service, they will receive text messages reminding them to take medicine or exercise.
Data compiled through the online tool have uses beyond an individual patient's self-management or a specific patient–physician encounter. More than 100,000 patients have completed the survey, and approximately 100 clinical sites are using aggregated data from the site. Some physician practices that have been using it for more than two years have close to 100 percent of their patients enrolled. Once a practice reaches this level of participation, physicians can look at their patient panel and determine, for example, how many have diabetes, are overweight, are low-income, or lack confidence in their ability to manage their conditions. Results can also be cross-tabulated for deeper analysis. The site is free and is used by provider offices, public health officials, employers, and chambers of commerce to aid their population health improvement initiatives. In aggregate, the data show regional differences as well as variations in patterns of care. The site also points users to interventions known to be effective in improving quality and maintaining health. Consumers access the online survey tool voluntarily using a code given to them by their provider. The results of the survey are sent to the individual provider with identifiers. When shared with other organizations or providers, the data are de-identified and aggregated.
Patient Activation Tool to Measure and Increase Patient Confidence
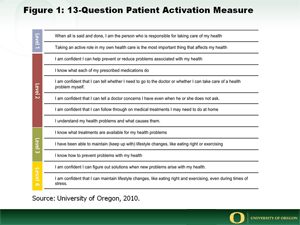
Judith Hibbard, Dr.P.H. professor in the department of planning, public policy, and management at the University of Oregon, and her colleagues also have been working to improve care for patients with chronic conditions using patient engagement techniques. "We're pretty good at clinical interventions, but we lag behind in behavioral interventions for chronic disease care," Hibbard says. To measure individuals' skill and competence in managing their health, as well as to gauge their beliefs about their role in managing their health, Hibbard and her colleagues developed the Patient Activation Measure (PAM)—a statistical measure used when precision and consistency are critical—based on a 13-question survey that assesses the level of a patient's confidence in chronic disease self-management (Figure 1). The PAM can be given to patients by their health team, health plan, or the health care system where they receive care. The results rank patients on a scale of 0 to 100, based on how engaged they are in managing their health, placing them in one of four activation categories. At the lowest level, patients often demonstrate low levels of confidence and weak problem solving skills. Programs for these patients tend to focus on small steps that build confidence, such as designing an exercise program that involves taking the stairs twice a day. At the highest activation level, patients are engaged in their care and the focus is on maintenance. Those patients may only need assistance in problem solving when unusually challenging situations arise, so that they may deal with those without compromising attention to their health.
Once a patient receives an individual PAM score, the health care team, health plan, or delivery system can provide support at his or her level through coaching or clinical interventions. (See case study in this issue for an example of a health plan's coaching program.) Coaches, many of whom are registered nurses, dieticians, social workers, or other health professionals, work with the patient, usually over the phone, to understand what will motivate him or her to change. The coach may also help design an intervention.
The power of the PAM tool is in its predictive power. It gives health care professionals a reliable starting point for designing specific interventions that will address an individual's needs and vulnerabilities for suboptimal care. Studies have found that those with higher PAM scores are more likely to follow recommendations for testing and medical utilization. Providers who invest in interventions tailored to PAM scores and those that focus on improving PAM scores are more likely to produce better health outcomes both in the short term and at 18 to 24 months in the future.[3] Research has also found that when conducting disease management programs with two groups—one that received coaching based on PAM results and one that didn't—the one that received coaching achieved better outcomes.
The PAM tool is now being used by approximately 50 organizations and government entities, including delivery systems, health plans, physician offices, federally qualified health centers, employers, Medicaid programs, and state government departments. It has also been translated into 16 languages for use domestically and internationally. Hibbard has found that approximately 30 percent of privately insured patients fall into the low activation category, while approximately 50 to 60 percent of Medicaid patients start there.
While health plans have been driving use of the tool, hospitals are also starting to look to the PAM as a means of reducing readmissions. As part of discharge planning, one New York hospital is administering the PAM to understand a patient's skill level for self-management once they arrive home, Hibbard says. "When thinking about self-management of chronic disease, we assume that everyone can jump in the deep end and swim laps," says Hibbard. "But we need to assume that not everyone can even swim."
Health Plan Uses Patient Activation Measure and Coaching to Increase Self-Management
ODS, a Portland, Ore.–based health insurer that serves members in Oregon, Alaska, and other regions of the Northwest, is using the PAM to develop tailored coaching interventions that help members with chronic conditions become better at self-management. ODS nurses and staff leverage pharmacy and medical claims data to identify members with gaps in care and non-adherence, as well as high utilization and high costs. The team of nurses and staff send welcome letters to members (about 11 percent of their 220,000 commercial populations) inviting them to participate in a coaching program to help manage their condition. Key areas of focus include depression, diabetes, and cardiovascular and respiratory disease. Approximately 1 percent of those contacted opt out of the program.
Prior to engagement, participants complete the PAM questionnaire and are assigned a dedicated coach based on their results. The coach interviews the member to understand what motivates him or her in order to determine what interventions will be most successful. Interventions are based on the members' PAM scores and life goals.
"Utilizing patient activation measures, motivational interviewing techniques, and one-on-one coaching enables members to make realistic and meaningful decisions that reflect their personal needs and values," said William Johnson, M.D., M.B.A., FACS, ODS vice president and chief medical officer. "Based on the member's level of knowledge, skills, and confidence in managing their health condition, members needing higher levels of support may be offered care coordination and case management services."
ODS employs six coaches, who are trained as registered nurses, dieticians, or naturopaths. Since beginning the program in the fall of 2008, ODS has completed 2,000 PAM surveys, 500 of which include post-intervention assessments. Early results show that the PAM tool coupled with the coaching intervention has enabled ODS to migrate or shift approximately one-third of the population at the lowest activation levels to levels three or four. In addition, early trends of program participants show a 6 percent increase in levels of medication adherence. Preliminary data also demonstrate a decrease in emergency and urgent care utilization and slight decreases in lengths of stay.
Physician Practices Strive to Increase Patient Engagement
Martin's Point Health Care, a Portland, Me.–based primary care provider and health plan, has been testing a variety of methods to increase patient engagement. In its Portsmouth, N.H., clinic, a team of providers has been developing a self-care report for patients that extracts information from the electronic health record. The report provides patients with an indication of how they are faring at managing cardiovascular disease, diabetes, and asthma. It also helps patients understand the metrics physicians and nurses use to monitor their progress and several actionable steps to improve their results. These patients also fill out a survey on their self-management abilities. From these reports, the local "population health nurse" identifies patients who are newly diagnosed, elderly, non-compliant, or in need of significant medication changes. These patients receive a phone call from the primary care nurse within one week of their visit to discuss questions and self-management needs.
The project began in June 2010 and its leaders have set specific goals: they want to see the number of patients who indicated they feel confident to manage their conditions rise from 76 percent when the project started to 87 percent. The results reflect the goals of the Triple Aim (an Institute of Healthcare Improvement Program that seeks to improve the health of the population, enhance the patient experience of care, and reduce or at least control the cost of care), as well as internal corporate goals. By the end of the third quarter, 84 percent of patients indicated they felt confident to manage their conditions.
That same Portsmouth office is working to increase shared decision-making through the use of "decision aids," which help patients explore their options, particularly for conditions for which there is no clear-cut approach. The decision aids are multifaceted: they include DVDs that explain treatments for different conditions and population-specific tools for identifying/answering questions about depression, menopause, and back pain. This pilot, which is only in its sixth or seventh month, aims to increase patient confidence so that patients are more likely to be active participants in their care.
Harvard Vanguard Medical Associates, a nonprofit, multispecialty medical group practice in eastern Massachusetts, created shared medical appointments so that patients could extend their time with physicians, have greater opportunity to ask questions, and learn from interacting with other patients. By listening to the concerns and strategies of other patients during the group visits, consumers report that they are able to gain useful information on self-care and management of their conditions.
Between eight and 15 patients meet with a physician as part of their follow-up care for a 90-minute visit (this compares with the 10 minutes they would receive individually). Vital signs and other personal information are taken behind a curtain and then all patients meet together in a circle with the physician. Patients come with a full range of conditions related to specialties such as nephrology, pain management, and dermatology. Blue Cross Blue Shield of Massachusetts reimburses for these visits at traditional rates (i.e. there is no group discount per patient).
Engaging Consumers by Improving Health Literacy
Outside of the provider or payer realm, organizations are also working to increase patient self-management by improving knowledge, confidence, and effectiveness. According to the Institute of Medicine (IOM), more than 90 million Americans (one of three adults) find it difficult to understand and use health information. The IOM has started a Roundtable on Health Literacy to work on policy and local solutions that will increase health literacy, which it defines as "the degree to which individuals have the capacity to obtain, process, and understand basic health information and services needed to make appropriate health decisions."[4] Some research estimates that the annual costs of low health literacy are between $106 billion and $238 billion.[5]
One of the IOM Roundtable members, Health Literacy Missouri (HLM), is working locally to educate providers and patients, fund grassroots efforts, and advocate for policy change. HLM estimates that low health literacy costs the Missouri economy between $3.3 billion and $7.8 billion annually.[6] The organization creates materials for clinics and hospitals that will help them communicate more effectively with patients. It has also developed a health literacy curriculum in a St. Louis suburban school district. HLM also funds community-based demonstration projects, including: an effort to teach rural Missouri seniors how to talk to their physicians and pharmacists about their health concerns; an initiative to train church leaders to reduce the stigma associated with mental health so that patients will communicate their needs to providers; and a program to teach low-income, urban African Americans how to read nutrition and prescription labels.
Implications
Rigorous assessment tools are important when designing effective self-management programs for patients with chronic disease. Patients with chronic diseases present with varying levels of education and confidence in their ability to manage their condition. Health professionals benefit from understanding the patient's level of knowledge and willingness to tackle care at home. Gaining an accurate read on a patient's abilities to self-manage can make interventions more effective and efficient. There are tools available to assess a patient's confidence and skill level, but they require dedicated staff and outreach to be successful.
Increasing patient self-management creates additional effort for providers. They must assess patient engagement on a regular basis, follow up with patients at home, and extract and track information electronically. These efforts require additional staff time, and they require the use of electronic health records and other sophisticated claims extraction, which may prove more challenging for smaller practices.
Expense is also a big concern. Some health care organizations, such as Cambridge Health Alliance, have pursued efforts to gain additional reimbursement for this time and effort, but there is no standard for such payments. Payment reform strategies, including the payment of care management fee to providers, may help address this issue.
As patients are expected to take a greater role in health management, patient engagement initiatives will need to take into account increasingly diverse patient populations. Efforts such as Health Literacy Missouri target programs to specific cultural, income, and geographic groups. However, delivery systems and health plans will need to tailor their materials and initiatives as well.
Notes
[1] See http://www.cfah.org/blog/2011/defining-patient-engagement
[2] R. Q. Wolever, M. Dreusicke, J. Fikkan et al., Integrative Health Coaching for Patients with Type 2 Diabetes: A Randomized Clinical Trial, The Diabetes Educator, July/August 2010 36(4):629–39; D. E. Wennberg, A. Marr, L. Lang et al., A Randomized Trial of a Telephone Care-Management Strategy, New England Journal of Medicine, September 2010 363(13): 1245–55; S. Butterworth, A. Linden, W. McClay et al., Effect of Motivational Interviewing–Based Health Coaching on Employees' Physical and Mental Health Status, Journal of Occupational Health Psychology, October 2006 11(4):358–65; and C. N. Melko and P. E. Terry, Diabetes Health Coaching Improves Medication Adherence: A Pilot Study, American Journal of Lifestyle Medicine, March/April 2010 4(2):187–194.
[3] C. Remmers, J. Hibbard, D. M. Mosen et al., Is Patient Activation Associated with Future Health Outcomes and Healthcare Utilization Among Patients with Diabetes?, Journal of Ambulatory Care Management, Oct./Dec. 2009 32(4):1–8.
[4] Institute of Medicine, Health Literacy: A Prescription to End Confusion (Washington, D.C.: National Academies Press, 2004).
[5] J. Vernon, A. Trujillo, S. Rosenbaum et al., Low Health Literacy: Implications for National Policy (Washington, D.C.: George Washington University School of Health Policy, October 2007).
[6] J. A. Vernon, A. Trujillo, and W. Keener Hughen, "The Health Policy Brief: The High Economic Cost of Low Health Literacy in Missouri," Health Literacy Missouri, 2009.