| Please take a moment to answer this six-question survey to help us improve the States in Action newsletter. We appreciate and welcome your feedback. |
The theme of the August/September 2008 States in Action is quality improvement, with a particular emphasis on chronic care management, medical homes, and the tools necessary to support them. We highlight the new State Quality Improvement Institute and some leading states' innovative efforts to redesign their health care systems, using such tools as incentive-based payment reform and information technology. The Federal Activity section describes the quality-related elements of the 2008 Medicare Improvement for Patients and Providers Act.
The State Quality Improvement Institute (SQII), launched in April 2008, is intended to help states plan and implement concrete efforts to improve health system performance and to share best practices among states. It is sponsored by The Commonwealth Fund and led by AcademyHealth. SQII leaders are hoping to address the wide variability in quality and value across the United States, evidenced in the Fund's State Scorecard on Health System Performance.
"The release of our State Scorecard spurred a great deal of discussion about what states could do to improve their rankings," says Anne Gauthier, assistant vice president at The Commonwealth Fund. "We heard significant interest in learning about innovative approaches other states were taking that could help improve their health system performance."
Nine states were selected to participate in the Institute through a competitive process: Colorado, Kansas, Massachusetts, Minnesota, New Mexico, Ohio, Oregon, Vermont, and Washington. Each will focus on improving performance on at least two quality indicators from the State Scorecard. The efforts are led by SQII teams of state officials and other stakeholders, with leaders designated by the governors. Team members include senior officials of the state's health/human service agency, Medicaid agency, quality councils, governor's office, state employee health agency, hospital association, major health plans, and others.
The Institute aims to "go beyond narrowly targeted quality improvement projects to really engage in delivery system redesign," according to Enrique Martinez-Vidal, SQII project director and vice president of AcademyHealth. Opening sessions took place in Chicago in late June, where experts in quality improvement gave presentations about prior and current state initiatives and offered advice and guidance. The sessions focused on:
- chronic care management and care coordination;
- payment reform and purchasing strategies; and
- transparency/data collection and reporting.
Following the plenary sessions, each of the teams worked independently with a quality improvement expert to develop their plans. Participants learned some important lessons from the meeting. For example, Washington team leader Maryanne Lindeblad says, "the sessions gave us an opportunity to step back and think through our initial plan for implementing medical homes and the steps needed. They helped us refine our thinking about how we could move forward in a meaningful way."
The teams learned the importance of having a long-term vision as well as short-term actionable and achievable goals. States will begin with initiatives that could have positive returns on investment to build support among legislatures and other stakeholders for longer-term reforms. Kansas' team leader Marcia Nielson says she "realized we need a model specifically designed to a rural state," where it may be harder to develop and nurture team-based care.
"We also encouraged the teams to examine their state's existing public and private quality improvement projects, and to coordinate efforts in order to align incentives and attain economies of scale," says Martinez-Vidal. Participants were particularly appreciative of having one-on-one time with experts, and learning about past and current quality initiatives around the country.
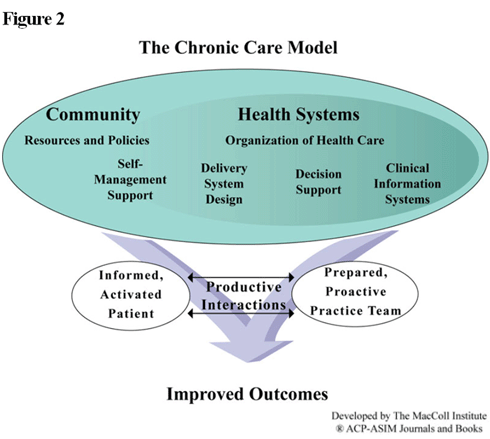
Incorporating what they learned, each state team developed an Action Plan defining goals, concrete steps, and measurable outcomes (Figure 1). Below we summarize the Action Plans from Massachusetts, Kansas, and Washington State. Each of the states plans to promote medical homes emphasizing chronic care management, supported by payment reforms and other tools (Text Box and Figure 2). They will pilot these strategies in Medicaid and, in some cases, state employee health plans. But the definitions of medical homes, methods for engaging consumers and other stakeholders, and goals and steps to achieve them vary among the states.
|
|
Massachusetts' Action Plan
Realizing that coverage expansion, the focus of the state's 2006 health reform legislation, is not enough to improve overall health system performance, Massachusetts is undertaking what some policymakers are calling "Health Care Reform 2.0," with a focus on improving health care quality. Massachusetts aims to implement the chronic care model in medical homes statewide, with the help of the State Quality Improvement Institute.
The Massachusetts SQII team, led by JudyAnn Bigby, M.D., the state's Secretary of Health and Human Services, and including public and private health care leaders, plans to promote coordinated, integrated care using a team-based approach. Its action plan is guided by the following principles:[1]
- Pursue a multifaceted approach: Clinical (care of the individual); Public Health (care of populations/communities); and Health Policy (payment for, organization of, and delivery of services);
- Seek a critical mass. No single actor has enough dominance to change provider behavior. Public and private partnerships/collaboratives are necessary to effect change.
- There are multiple and complex determinants of health and health care. Non-traditional health actors (housing, parks, transportation, urban planning) should be included "at the table."
- Coverage is not enough. An accountable health care system should focus on the patient by optimizing services and payment to maximize health outcomes.
- Think broadly—act incrementally.
- Collaborative participation and shared commitment by non-SQII team members (e.g., Department of Public Health, Healthy Massachusetts Compact, Massachusetts Medical Society, and other external stakeholders) are essential in order to align priorities and actions.
One of the state's key strategies for achieving its goals is payment reform. "Aligning quality measurement across payers and reforming payments to primary care physicians are essential to redesigning medical practices and implementing the medical home model," says Bigby. For example, practitioners could receive additional care management payments over the typical service reimbursements. The team hopes that, by the spring of 2009, they will have a statewide, multi-payer coalition to sponsor and test this approach.
The team also plans to work with the state's Medicaid agency, the Group Insurance Commission (the state employee and retiree health plan), and the Connector (the state's health insurance exchange) to explore opportunities to promote self-management of chronic conditions.
Additional planned interventions include educating primary care providers about evidence-based diabetes care standards, creating a diabetes patient registry, and working with the Department of Health to launch a consumer education campaign.
|
Kansas' Action Plan
The Kansas SQII team has developed a plan to define, test, and evaluate a medical home delivery model through payment reform. Phase 1, from July 2008 through July 2009, focuses on "attaining a clearer understanding of what constitutes a medical home and its importance," according to Marcia Nelson, executive director of the Kansas Heath Policy Authority and leader of the SQII team. The plan involves working closely with physicians, consumers, Medicaid managed care plans, foundations, and other stakeholders to define and gain support for the medical home model. The model will focus on children, elderly and disabled patients, and other populations. Team members will prepare specific timetables and goals to present to the state legislature in January 2009.
During Phase II, July 2009 through July 2010, the state plans to phase in payment incentives to practitioners for adopting certain elements of the medical home model. Initially, the awards will be targeted at providers serving certain groups of Medicaid beneficiaries and state employees through the State Employee Health Benefit Program, with further populations to be added over time. There will be ongoing evaluations, and the state will make mid-course corrections depending on the results.
The team has selected two quality goals, to be achieved by 2012:
- 85 percent of all children in Kansas will have a medical home; and
- avoidable hospitalizations for pediatric asthma in Kansas will be reduced to no more than 82 per 100,000 for children ages 0 to 17 years.
|
Washington's Action Plan
Like the teams in Massachusetts and Kansas, Washington State's SQII team is focusing on patient-centered medical homes. It has developed an Action Plan with three critical interventions:
- create an operational definition of medical home in order to measure and improve medical home capacity;
- develop reimbursement strategies to support providers in adopting a medical home model of patient-centered care; and
- engage consumers and providers in participating in patient-centered medical homes.
For each of these interventions, the team has developed specific steps and a timetable. Many of these steps involve coordinating with other initiatives already in place in the state. By the end of the summer, the team expects to have reached consensus on an operational definition of a medical home and identified performance measures for medical homes and patient outcomes that can be demonstrated and rewarded.
Over the coming years, the state plans to evaluate data sources, performance indicators, reimbursement models, and ways to engage practitioners and consumers. As part of a broader health reform package, it plans to pilot a payment system that rewards providers who incorporate evidence-based practices and elements of patient-centered care by 2011.
"We're interested in models to effectively use resources to create medical homes that are more community-based," says team leader Maryanne Lindeblad, director of Washington's Division of Healthcare Services. She adds that the team looks forward to assistance from the Quality Institute in identifying best practices in reimbursement design, data sources, and ways to measure the effectiveness of patient-centered medical homes.
|
Next Steps for the State Quality Improvement Institute
During the coming year, the State Quality Improvement Institute will provide technical assistance, such as conducting background research and bringing experts to the states to help them address specific challenges. Bimonthly conference calls will enable the teams to share their successes and challenges. A project Web site provides an additional vehicle for communication among the teams; four Web seminars are being planned. The state teams will convene for a final meeting next spring to assess progress and enable the participants to learn from each others' experiences.
"If at the end of the year the states have taken concrete steps toward redesigning their health care systems, and have established relationships and ongoing communication with each other, we'll consider the Institute a success. And if they do these things, we would also expect to see movement in their Scorecard indicators in a few years," says Gauthier.
Reference
[1] State Quality Institute Action Plan, "Implementing a Chronic Care Model for the People of Massachusetts," July 2008.
|