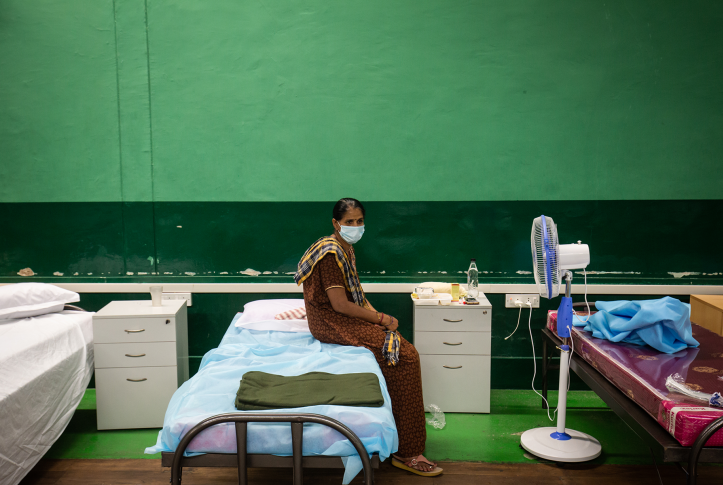
India and the United States have vastly different health care systems with one striking similarity: low-income people without adequate health insurance face significant financial barriers to health care. Neither of the world’s two largest democracies has universal coverage, which means that those who cannot afford to pay for medical care may go without or incur debt. In the event of a medical emergency — for instance, an accident or cancer — these challenges could prove catastrophic.
While systemic reform — like strengthening the social safety net and expanding health coverage — is necessary in the long term, one short-term fix is to provide direct cash transfers to low-income people facing medical emergencies.
Public Programs to Address the Problem Fall Short
In the U.S., half of all adults with lower incomes don’t get needed care because it’s too costly. Medicaid, the public insurance program for people with low incomes, covers one of five Americans for many — but not all — health services. Further, although the Affordable Care Act gave them the option, not all states expanded Medicaid eligibility. In 12 states that have not expanded, more than 2 million low-income Americans remain uninsured.
In India, there are a different set of obstacles, but a similar result: millions of low-income people cannot afford health care. While each Indian state is required to provide free universal access to health services, health care is chronically underfunded, meaning that although they are entitled to free care, many go without. Because of the severe shortages of staff and supplies at government health facilities, many people seek care from private providers and pay out-of-pocket.
As in the U.S., there are significant health, social, and income inequities. Many of the poor are daily wage laborers, or live in rural areas where health services are often out of reach; these challenges are compounded for women or people of low castes.
To be sure, the relative financial challenges are far greater in India: the current health expenditure per capita in the U.S. is the highest in the world. At $10,921 it is more than 170 times India’s $64, one of the world’s lowest. In both countries, the absence of an adequate safety-net system means that low-income people rely on family and friends or other private sources to cover medical expenses.
Cash Assistance Can Help
Historically, Americans have relied on private sources like religious institutions or other charities to fund medical emergencies. In recent years, there has been a rise in crowdfunding to cover medical expenses, but success is limited. GoFundMe pages, for example, raised more than $3 billion from May 2010 through December 2018. But more than $10 billion was sought for the same period, indicating many were not able to raise funds needed for medical care.
One model being piloted in India eliminates the need to crowdsource funds by providing direct grants to the working poor, who often sell land or possessions or borrow money at predatory rates to pay for care. Since most Indian health facilities require payment up front, this can be a life-or-death decision. The Soondra Foundation provides daily wage earners (who earn approximately $5 a day) with grants from $25 to cover a hand fracture to up to $1,500 for intensive care unit admission. The funds go directly to providers to cover patients’ medical bills. Accountability partner organizations oversee disbursement of funds to ensure they are spent appropriately.
During the COVID-19 pandemic, the foundation helped 15,600 people with food rations and medicines. Through partner nonprofit organizations, it also supported a community of more than 500 patients with tuberculosis and their families for the 21 days of India’s first lockdown, one of the most stringent in the world. As a result, these families could stay home and receive adequate nutrition as they continued with their medication. To date, the privately funded foundation has helped 120 families with emergency direct-cash grants.
Takeaways for the U.S.
Medical debt remains a significant barrier to health care for many, a problem exacerbated by the COVID-19 pandemic. Policy changes to shore up social programs are difficult and can take a long time; short-term cash grants could help.
The Indian government launched an initiative in 2017 to provide financial support for health expenditures to 500 million of the most vulnerable Indians but it faces implementation challenges.
The U.S. also has deployed short-term cash programs. Policymakers enacted sweeping pandemic relief measures in the form of stimulus payments and other measures, which produced positive health effects and reduced poverty. But these were specific to the pandemic and do not provide security for future medical emergencies individuals may encounter. As the pandemic enters a new phase, Congress is contemplating policy options for further COVID relief funding and increases to social and health care spending. However, there is no guarantee that additional, near-term public funds may be available. Although the Biden administration recently announced a plan to ease medical debt, it focuses on consumer protections and does not give direct grants to low-income people.
In the absence of a robust, publicly funded social safety net, direct payments to individuals and families can help, as the Soondra Foundation’s program in India demonstrates. At least 20 universal basic income pilots (publicly and privately funded) are underway in the U.S.; evidence from cash-assistance programs has found the monthly support increases positive health outcomes. Individuals who receive cash grants make rational decisions to support their health and well-being, according to an analysis of spending patterns of low-income New Yorkers who received an unconditional $1,000 cash transfer during the pandemic. These efforts demonstrate that providing direct cash grants to low-income people, while not a replacement for a publicly funded safety net, could be a short-term stopgap until the U.S. achieves systemic health reform.