Concerns about possible surges of COVID-19 patients, combined with the spread of value-based payment and companies offering technology and operational support, have prompted some health systems and health plans to take a second look at the hospital-at-home model.
In This Issue
Long before fears of infection from the coronavirus made people wary, hospitals were often not the best place to be treated and recover. Awareness of the risks of infections and the debilitating impacts of hospital stays, particularly on patients who are frail, have cognitive impairments, or other vulnerabilities, prompted Bruce Leff, M.D., a geriatrician and health services researcher at Johns Hopkins University, to establish the first hospital-at-home program in the United States 20 years ago.
The model, which offers people who would typically require hospitalization to treat problems such as acute pneumonia, dehydration, or exacerbations of conditions like heart failure or chronic obstructive pulmonary disease (COPD) the option of receiving acute-level care in their homes, has been one of the most studied health care delivery reforms. Multiple trials and meta-analyses have determined that it can be safer, cheaper, and more effective than institutional care for some patients. The first trials, held in the U.K. in the late 1970s, found that hospitalizations conferred no benefits over home-based acute care for people experiencing acute myocardial infarctions. Since then, hospital-at-home programs have been firmly established in the United Kingdom, as well as in Australia, Canada, Israel, and other countries with government-run health systems.
In recent years, a handful of U.S. health systems have launched similar programs, either because their hospitals are operating at capacity and/or they’ve taken on financial risk for the total costs of patients’ care and thus benefit from delivering services in a lower-cost setting. The Veterans Health Administration, which controls both payment and care delivery, has funded its own hospital-at-home program, as have some health systems that have their own health plans and/or substantial numbers of patients in accountable care organizations or managed care plans.
Several startup companies now offer logistical support and technology to facilitate hospital-at-home programs, as well as help contracting with commercial payers. Broader spread, however, has been stymied by the fact that Medicare does not pay for acute services provided outside of hospitals for fee-for-service beneficiaries. (For more detail on the financing of hospital-at-home programs, see our Q&A below with Harold Miller, president and CEO of the Center for Healthcare Quality and Payment Reform, a research organization that designs innovative models for health care payment and delivery.)
As in so many parts of health care, the COVID-19 pandemic has catalyzed change: not only has it created a clear rationale for avoiding hospitals when possible, it has prompted Medicare to allow providers to bill for acute treatments delivered in surgery centers, hotels, or other non-hospital facilities. Some are hoping waivers tied to the Hospital Without Walls initiative will open the door for Medicare to pay for acute care in homes, too.
In this issue of Transforming Care, we report on health systems that have adapted and adopted the hospital-at-home approach to help them respond to the pandemic while still ensuring access for all patients. In the past few months, the health systems have leveraged the model to facilitate early discharge of patients hospitalized for reasons other than COVID-19 and thus clear beds for COVID-19 patients; monitor lower-acuity COVID-19 patients at home; and avoid bringing frail, immunocompromised, or other vulnerable patients needing acute care to the hospital.
Leff attributes this uptick in interest both to the merits of the model and expediency: “As the economist Milton Friedman pointed out, in a crisis people go looking for ideas that have been around for a while because they don’t have time to develop something new.”
Clearing Hospital Beds to Prepare for COVID-19 Patients
Mount Sinai Health System
This spring in New York City, the Mount Sinai Health System leaned on its hospital-at-home program to help it cope with a surge of more than 2,250 COVID-19 patients. Providers were able to refer some patients who were acutely ill with COVID-19 as well as some who were acutely ill from other conditions to the program to clear beds — doubling its census compared with before the pandemic.
Mount Sinai Health System launched a hospital-at-home demonstration in 2014, funded by a $9.6 million grant from the Center for Medicare and Medicaid Innovation. Leaders were drawn to the model as a way to relieve pressure on their inpatient wards, which even before the pandemic were routinely filled beyond capacity. They also wanted to build a suite of home-based services, including rehabilitation, primary care, and palliative care, that appeal to patients and help the health system succeed in value-based contracts that reward providers for improving outcomes and reducing costs. Today, over 80 percent of the health system’s primary care patients and 40 percent of those treated in its hospitals are covered through some type of value-based payment.
The hospital-at-home team of nurses, physicians, therapists, social workers, and others provided services including X-rays, IV infusions, laboratory monitoring, and oxygen treatments over the three-year demonstration. According to Mount Sinai, compared with similar patients who received care in hospitals, they had 50 percent fewer unplanned readmissions and shorter lengths of stay, were more satisfied with their treatment, and accrued 20 percent to 30 percent lower costs. And, not surprisingly, there were no hospital-acquired infections.
As the demonstration wound down, Mount Sinai’s leaders looked for a way to keep the program afloat without revenue from Medicare’s fee-for-service program. In 2017, they set up a joint venture with Contessa Health, a Nashville-based startup launched in 2015 whose founders sought to make home hospitalizations financially sustainable by contracting with health plans willing to pay for them, namely Medicare Advantage plans, Medicaid managed care plans, and commercial health plans. Under the venture, Mount Sinai clinicians in partnership with clinicians from the Visiting Nurse Services of New York provide care to patients, while Contessa offers care management services and uses a proprietary platform to manage billing, supplies, and other logistics. Care coordinators hired by the joint venture work in four of Mount Sinai’s emergency departments to help enroll patients who have been referred to the program.

Some patients are admitted for one day of observation to determine if they require acute care, while others are admitted directly for 30-day episodes that include acute and some postacute care services. Certain patients, such as those needing dialysis or surgery, are not eligible and others are screened out because they lack reliable social supports. Since 2017, some 1,000 patients have enrolled; most people who are offered the option have accepted, says Niyum Gandhi, Mount Sinai’s chief financial officer. “People who turn it down have never been hospitalized before,” he says. “If you have ever had an inpatient stay, you would never want to be admitted again.”
The joint venture receives bundled payments from health plans that are based on a 30-day episode of care and pegged to historical costs for similar patients over this time frame. If the cost of delivering care is lower, Mount Sinai and Contessa share in the savings. If it’s higher, they are responsible for the overage.
Tufts Medical Center
Like Mount Sinai, Tufts Medical Center in Boston was bursting at the seams, pre-COVID-19; it routinely had to turn down requests to accept patients from other hospitals because no beds were free. To help expand access, leaders had begun partnership discussions with Medically Home, another hospital-at-home company founded in 2017 after eight years of research and development. Then, in March, Michael Apkon, M.D., Ph.D., Tufts Medical Center’s president and CEO, moved forward quickly. “At that point, we thought we may only have a matter of weeks before we needed every bed for COVID-19 patients,” he says.
Medically Home partners with its clients’ clinicians and also hires physicians and nurse practitioners, who work from a central hub from which they use remote monitoring, video, and other telehealth tools to oversee patients’ care. They confer with Tufts Medical Center’s attending physicians to make sure patients are good candidates for the program. Advanced practice providers, paramedics, nurses, phlebotomists, technicians, therapists, and other staff visit acutely ill patients in their homes, providing infusion, lab tests, imaging, nutrition, translation, and other services. “All the services they are used to getting in a hospital are dispatched at home rapidly — in less than an hour,” says founder Raphael Rakowski, an engineer by training who sees the challenge of home acute care as one of logistics rather than clinical practice.
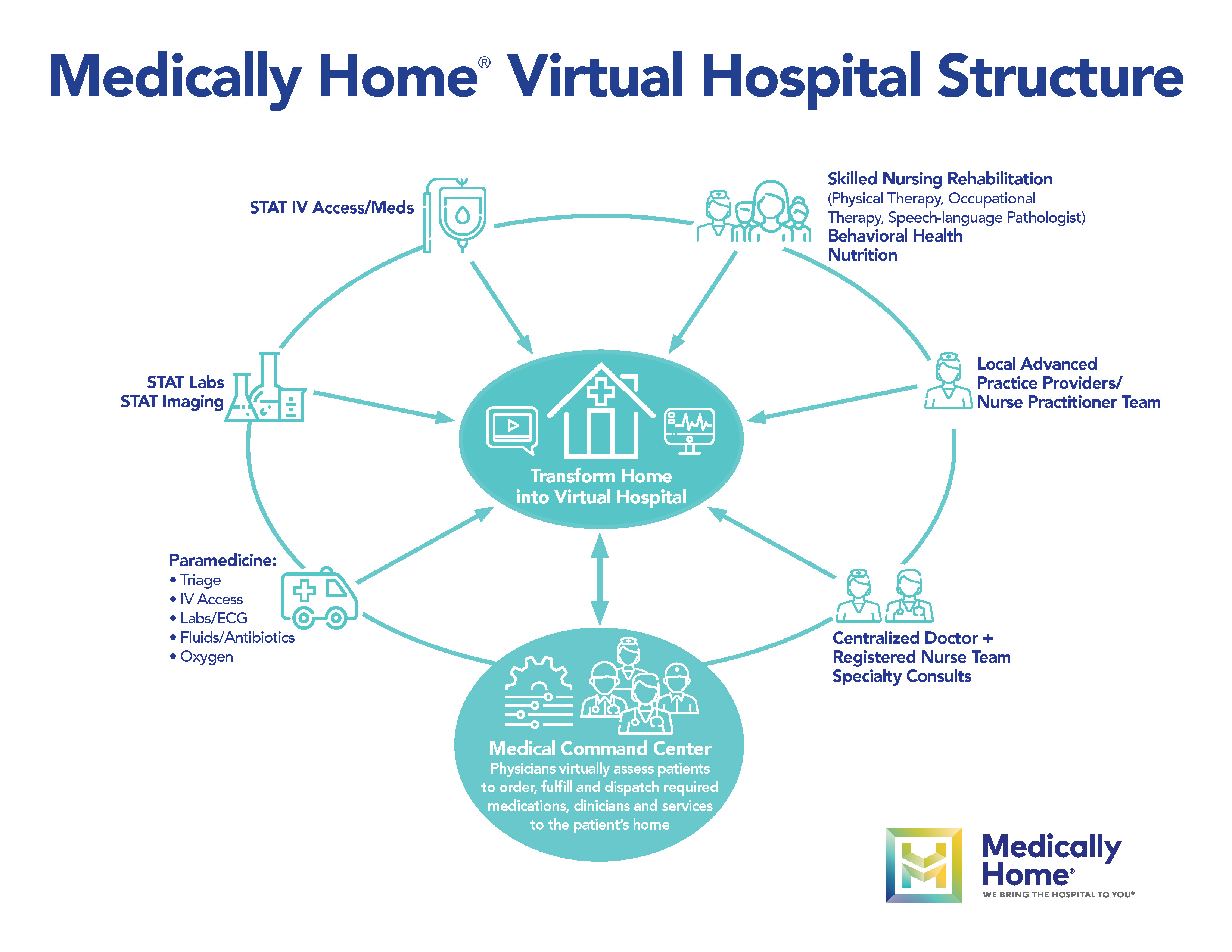
Medically Home draws on its health system partners and community resources, including local paramedics and equipment suppliers, to build a virtual hospital.
Medically Home uses its videoconferencing platform to link Medically Home clinicians with a patient’s family members and his or her regular clinicians. “We knew from the beginning the family in the household was as important to us as the patient because the family often drives utilization,” says Rakowski. “They are the ones who call 9-1-1 when they don’t understand what is happening.”
Since April, Tufts Medical Center has referred 10 patients to this program, including those who are acutely ill but want to avoid coming to the hospital and those who were hospitalized but could be discharged sooner than normal with home care.
Monitoring COVID-19 Patients Remotely
MetroHealth
In Cleveland this spring, the MetroHealth county health system began offering patients who test positive for the novel coronavirus but appear to be relatively stable the option of receiving oversight from clinicians at home — inspired by the hospital-at-home approach. “We had been thinking about the hospital-at-home model since 2016, but there wasn’t a burning platform for us to do it,” says Nabil Chehade, M.D., MetroHealth’s senior vice president for population health. “When the COVID-19 crisis came, we saw our opportunity.”

MetroHealth monitors COVID-19 patients in their homes with low-cost devices, including a Bluetooth-enabled tablet, pulse oximeter, thermometer, and spirometer. Source: MetroHealth.
So far, 22 patients have been sent home with a Bluetooth-enabled tablet, pulse oximeter, thermometer, and a spirometer if indicated and receive regular calls from nurses and doctors to ensure they’re recovering; very few have needed to be transferred back to the traditional hospital setting. MetroHealth also plans to make the service available for COVID-19 positive patients who are discharged from the intensive care unit but need ongoing monitoring as they recover. While the effort so far is modest, leaders hope it will offer a foundation on which to grow a broader hospital-at-home program. They are looking into how they may be able to bill for some of these services under a Hospital Without Walls waiver but for now are only able to bill for some of the services they provide and are subsidizing the rest. “We’re doing it because it’s better for the patient,” Chehade says.
Providing Urgent and Emergent Care in the Home
DispatchHealth
DispatchHealth, a startup company that has adapted the hospital-at-home model to provide urgent, emergent, and acute care in people’s homes, has experienced a 40 percent increase in volume during the pandemic, driven by more referrals from health plans and providers and people’s fears of going to emergency departments (EDs) or hospitals.
DispatchHealth was founded in 2013 by Mark Prather, M.D., M.B.A., an emergency medicine physician who believed that because EDs are the entry points for most hospital admissions, disrupting traditional pathways to admission would require bringing emergency services to people’s homes. Its clients include commercial health plans, Medicare Advantage, and Medicaid managed care plans as well as accountable care organizations and other provider groups taking on risk — parties that have incentives to help people avoid hospitals as a means of controlling costs. Most of DispatchHealth’s clients pay bundled fees for episodes of emergent, acute, and/or postacute care, which are 75 percent, 10 percent, and 5 percent less, respectively, than the average costs among public and private payers for that type of care in that region, according to the company. Clients then offer their members access to DispatchHealth services.

For example, someone with COPD who becomes short of breath and develops a productive cough may call their primary care provider, a DispatchHealth client. That provider can then call DispatchHealth to help them determine if they can safely treat the patient in their home. “We want to make sure we are not delaying care and that someone with a complaint that is truly emergent, such as sepsis, gets to the hospital,” Prather says. If determined to be safe, DispatchHealth sends a physician assistant or nurse practitioner, accompanied by a medical technician, to the patient’s home to provide lab tests, X-rays, and other treatment. An ED physician makes virtual consults to help make diagnosis and treatment decisions.
Should patients require acute care (about 5 percent do), DispatchHealth sends a different team, which includes a hospitalist physician, physician assistant or nurse practitioner, and a nurse, to oversee their care over the next 14 to 30 days.
While DispatchHealth treats a wide range of people, it has carved out a space in serving those who may cycle in and out of EDs because of their social circumstances, as well as medical conditions. DispatchHealth staff screen all patients for unmet social needs then partners with local food banks to deliver groceries to those who are food insecure and connect those who are socially isolated to supportive programs. “We spend on average 55 minutes with emergent patients,” says Prather. “We say to our providers, ‘When you are there, solve as many problems as you can.’ This approach is the exact opposite of what I used to do in the ED, which was fix the immediate problem and decide if patients needed to be admitted. Our approach is more aligned with value-based care.”
Thus far this year, DispatchHealth has provided services to 170,000 people in 12 different states, including 4,000 patients with COVID-19. Recent venture capital funding is helping the company expand rapidly.
Expanding Acute Care, Not Hospital Beds
Marshfield Clinic
As they watched COVID-19 cases fill hospital wards in other states, leaders of Marshfield Clinic in Wisconsin were reassured that their hospital-at-home program would offer a relief valve, should they experience a surge.
Marshfield Clinic, which began as a multispecialty group practice and went from owning one hospital in 2015 to nine today, adopted hospital at home to expand acute care services without building new beds. It formed a joint venture with Contessa Health in 2016 and began offering members of its own health plan (which includes people covered through their employers as well as Medicare Advantage and Medicaid managed care beneficiaries) the option of what it calls Home Recovery Care, a 30-day episode that includes acute care as well as postacute rehabilitative services. Having this option makes it possible for Marshfield to operate its hospitals with fewer beds. Marshfield reserves traditional hospital beds for higher-acuity patients who require continuous monitoring or highly specialized procedures, such as those with sepsis or an acute myocardial infarction.
Marshfield began by offering Home Recovery Care to patients needing acute treatment for one of six conditions: cellulitis, pneumonia, COPD, congestive heart failure, urinary tract infection, and deep vein thrombosis/pulmonary embolism. Over time, it expanded home acute care to 150 different diagnoses and now treats some 250 patients a year at the Marshfield location; it is expanding to Eau Claire and other facilities starting this year. The program is overseen by a dedicated team of six hospitalist physicians employed by Marshfield who make virtual visits to patients from a central hub and oversee the work of specially trained home health nurses who visit patients, spending anywhere from four hours to most of a day with them.
Marshfield leaders report that during the program’s first three years, patients receiving home care had 44 percent fewer unplanned readmissions than other members of their health plan with the same conditions treated in the hospital as well as shorter lengths of stay (defined as the number of days they required acute-level care). Costs were lower, even after accounting for the 30-day episodes.
Narayana S. Murali, M.D., Marshfield’s executive vice president for care delivery and chief strategy officer, says that patients treated at home are also more satisfied with their care, with scores on the Hospital Consumer Assessment of Healthcare Providers and Systems, or HCAHPS, of 95 percent compared with 75 percent among traditionally treated patients. Murali attributes this to the fact patients’ services through acute treatments and rehabilitation are coordinated and seamless. “Patients have easy, 24/7 access to their providers,” he says “Over the 30-day episode, we make sure that every ‘T’ is crossed and every ‘I’ is dotted.”
Implications for the Future of Acute Care
It remains to be seen whether the 40-year-old hospital-at-home model will gain broader traction in the U.S. now that vendors have developed turnkey systems to operationalize it and the pandemic has normalized the idea of receiving acute care outside of hospitals, in part via telehealth platforms.
Many programs still face immediate challenges, including the need to secure enough personal protective equipment and coronavirus tests for staff to safely treat patients in their homes. Succeeding may also require education and incentives for clinicians and care managers to actively recruit patients — a hurdle the startup company DispatchHealth overcame by helping patients avoid the ED altogether.
A critical mass of patients and economies of scale are needed to make acute care in homes feasible.
While startup companies create efficiencies through supply chain management, use of care protocols, and technology, one of their largest expenses is staffing. The Johns Hopkins hospital-at-home program and some early adopters, including Presbyterian Healthcare Services in Albuquerque, N.M., have sent physicians to patients’ homes, while the newer programs reduce costs by having a small team of physicians and/or nurse practitioners oversee care via virtual rounding and sending nurses and other less highly paid staff to patients’ homes. “The doctor-in-a car idea is not scalable,” says Rakowski of Medically Home.
Programs also require a critical mass of patients to be viable. Murali at Marshfield says the minimum for achieving economies of scale is 100 per hospital per year. With funding from all payers, Murali thinks up to a third of Marshfield’s acutely ill patients can safely be cared for in their homes. This high a census would make it easier to train staff to work in both hospital and home settings and move between them as demand changes, rather than relying on dedicated group of clinicians for at-home care.
Building hospital-at-home programs may also be easier if they are part of a continuum of home-based services, as they are at Mount Sinai and Presbyterian. If patients in skilled nursing facilities continue to become seriously ill from the coronavirus, patients and providers may be more receptive to models that enable postacute rehabilitation at home. And working in different settings could help reduce clinician burnout.
It’s important to recognize that as with other tech-enabled care models, hospital at home could leave some patients on the wrong side of the digital divide. To make its program accessible, the MetroHealth system, which serves predominantly publicly insured or uninsured patients, pays to set up a dedicated broadband lines in patients’ homes and partners with AT&T, which has donated tablets that patients use to report their symptoms and communicate with providers. It also won a $900,000 grant from the Federal Communications Commission in mid-June to expand its efforts; the grant enables the health system to purchase new tablets, webcams, and tools such as blood pressure cuffs and pulse oximeters needed to offer home care to both COVID-19 positive patients and high-risk non-COVID-19 patients. (MetroHealth also routinely screens patients for unmet social needs and has been making deliveries of food and other supplies.)
Hospital-at-home programs could be adapted to benefit particular groups of patients.
Medically Home has begun testing other use cases for the model as a means of expanding its business beyond acute and postacute care. It has partnered with clinicians at Massachusetts General Hospital to offer home visits and telehealth supports to patients with pancreatic cancer participating in a clinical trial. Patients use Medically Home’s platform to report their symptoms, such as pain and fatigue, and vital signs, such as heart rate and blood pressure, throughout their time on treatment. Medically Home clinicians then follow up, for example by deploying staff to provide fluids as needed and address concerning symptoms that may occur.
Home-based models that offer coordinated episodes of care — including for emergent, acute, and postacute needs — could be of particular benefit to patients who have frequent emergency department visits or hospitalizations. “We need a single episode of care, with a single team caring for the patient, being accountable, creating a relationship of trust, and really attacking social determinants, which is often how people get into the hospital in the first place,” says Rakowski.
Such models may be easier to establish for large, integrated delivery systems in dense metropolitan areas and harder for smaller provider groups, particularly in rural areas with dispersed populations.
New payment models and clear regulatory guidance from the Centers for Medicare and Medicaid Services (CMS) are needed.
While startup companies report an uptick of interest in home hospitalizations from health systems looking to prepare for potential future waves of COVID-19 patients, they say lack of payment for acute care outside of hospitals for fee-for-service Medicare beneficiaries remains the largest barrier to spreading this model.
The Physician-Focused Payment Model Technical Advisory Committee (PTAC), tasked with evaluating physicians’ ideas for how they could work differently if they were paid differently, has in recent years reviewed and recommended to CMS two proposals for hospital at home, one submitted by Marshfield Clinic and one by Mount Sinai. Both would provide bundled payments for episodes of acute and postacute care. CMS has not acted on these proposals (or any others submitted by PTAC), but has reportedly inquired how one health system accounts for its costs for home-based acute care for certain conditions.
CMS’s Hospital Without Walls initiative could provide a means by which hospitals can provide some care in homes, but it’s unclear how long the waiver will remain in place. To qualify as acute care, hospital providers need to deliver home services themselves and must deliver a certain level of services (e.g., oxygen, durable medical equipment, radiology, and meals).
A CMS spokesperson says the agency has shown its commitment to expanding health care services through the Hospital Without Walls initiative and is continuing to think carefully about the potential of the hospital-at-home model to expand capacity during possible future waves of COVID-19. "CMS is currently assessing this with a focus on making sure that we are leveraging the latest technology and modernizing the Medicare program to provide high-quality care to beneficiaries,” the spokesperson says.
In the short term, spread of the model may depend on the course of the coronavirus and hospitals’ desires to prepare for potential surges. In the longer term, it may find broader interest if value-based payments gain broader traction.
“My fear is that the turmoil ensuing from the pandemic will just be viewed as a temporary aberration — that as soon as it’s over, we’ll go back to the way things were before, and the crisis opportunity to change things for the better will have been lost,” says Harold Miller, president and CEO of the Center for Healthcare Quality and Payment Reform.
Q&A with Harold Miller, President and CEO of the Center for Healthcare Quality and Payment Reform

Harold Miller, president and CEO of the Center for Healthcare Quality and Payment Reform, spent four years serving on the Physician-Focused Payment Model Technical Advisory Committee (PTAC). The committee was created by Congress in 2015 to evaluate physicians’ ideas for new Medicare payment models and recommend promising ones to the Department of Health and Human Services (HHS). In recent years, PTAC recommended that HHS implement two hospital-at-home programs that demonstrated patients given acute services in their own homes had fewer complications and accrued lower costs than similar patients treated in a hospital. HHS elected not to, citing among other things concerns about the payment methodology and the feasibility of establishing programs in rural communities, where it may be hard to find sufficient staff and supplies. We asked Miller whether he thought the model might have a better chance of adoption during the pandemic, as hospitals seek ways to quickly expand capacity and some patients remain leery of coming to hospitals.
Transforming Care: The limiting factor for hospital-at-home programs seems to be CMS’s reluctance to pay for home-based acute care for fee-for-service Medicare beneficiaries. Why do think there’s so much resistance to it after so many studies have demonstrated its effectiveness and other countries have used the approach for decades?
Miller: One reason is that it’s hard to guarantee significant savings outside of large metropolitan areas where you have the population density to enroll enough patients to support the costs. The enabling legislation for the Center for Medicare and Medicaid Innovation allows implementation of programs that improve quality as long as they don’t increase spending. But as a practical matter, the actuaries will not approve a program that improves quality unless it also saves enough money to guarantee statistically that the program won’t increase spending. It’s nearly an impossible standard to meet for programs and models that don’t involve large numbers of patients, since even a small number of unusually expensive patients can throw off the results in any given year. So even if you can provide better care in the home at lower cost for most patients — it doesn’t clear the statistical bar.
Transforming Care: Do we need to redefine the standard by which innovations are measured to put more emphasis on value as opposed to strictly cost?
Miller: It’s important that we find ways to control cost but we have to be realistic about what is feasible. It’s not just the statistical standard that’s a barrier. There’s also been unwillingness to consider an innovative payment model unless it can generate billions of dollars in savings. There are a number of proposed models that could both improve quality and reduce costs for Medicare patients with specific health problems, such as inflammatory bowel disease or neurological conditions, but there aren’t enough patients with any one of those conditions to produce billions of dollars of savings. In fact, except for joint replacements and a few other conditions, no individual health problems are big enough individually to produce billions of dollars of savings. On the other hand, implementing all of those separate initiatives for individual conditions would, together, generate large amounts of savings. The hospital-at-home model falls into this category because initially it would be focused on a small group of patients, which limits the magnitude of the initial savings, but over time, it could be expanded to additional conditions with greater savings.
Transforming Care: Could hospital-at-home programs be supported through bundled payments for discrete conditions?
Miller: Trying to do hospital-at-home through condition-specific payments creates the opposite problem. There probably wouldn’t be enough patients to make the hospital-at-home program viable if it could only admit patients with one or two conditions. There are fixed costs to a hospital-at-home program, just like there are fixed costs for a hospital, and there have to be enough patients to justify engaging nurses to make home visits and setting up the monitoring systems et cetera. A better solution would be to implement multiple home-based care models simultaneously — not just hospital-at-home for acute patients, but also home-based palliative care for patients with serious illness and home-based postacute care for postsurgical patients. This would create economies of scale that would allow programs to deploy staff to a larger number of patients in a region, and it would also enable a better continuum of care for patients.
Transforming Care: Do you think COVID-19 creates an imperative to support the model?
Miller: The pandemic showed that we need more ways to deliver care to patients in their own home, and it also showed that CMS can change its payment systems almost overnight if it wants to. CMS issued thousands of pages of regulations in the course of two months that dramatically changed the way Medicare pays for a wide range of services. Physicians and patients have been asking for years for the ability to deliver more services in patients’ homes through telehealth, but before this spring, Medicare wouldn’t pay for it. As soon as Medicare started paying for it, it was implemented rapidly and effectively, and large numbers of patients are now getting care in a better way than they were before. We should do the same thing with the hospital-at-home concept. The pandemic made it clear that we need that kind of capability. The model has already been used successfully in many places, so it doesn’t need more testing or evaluation through the Innovation Center. CMS and other payers should simply start paying for it. If any problems develop, we can make adjustments just like we do with every other payment system, but there is no reason to continue denying patients the ability to receive care in this desirable and cost-effective way.
Publications of Note
Adding Social Workers to Primary Care Teams Reduces Hospitalizations, ED Visits
Adding social workers to the primary care teams at Veterans Health Administration facilities serving rural communities increased social work encounters by 33 percent among all veterans who received care. Among high-risk patients, the researchers observed a 4.4 percent decrease in the number of veterans who had any acute hospital admission and a 3.0 percent decrease in veterans who had any emergency departments visits. Portia Y. Cornell, “Embedding Social Workers in Veterans Health Administration Primary Care Teams Reduces Emergency Department Visits,” Health Affairs 39, no. 4 (April 2020):603–12.
Birth Centers Improve Birth Outcomes Among Medicaid Women and Reduce Costs
A study of the federal ‘Strong Start for Mothers and Newborns’ initiative, which enhanced service delivery for Medicaid-covered women through the use of birth centers, group prenatal care, and maternity care homes, found women who received prenatal care in birth centers had lower rates of preterm and low-birthweight infants, lower rates of cesarean sections, and higher rates of vaginal birth after cesarean than did women in the comparison groups. The authors also found the improved outcomes were achieved at lower costs. There were few improvements in outcomes for participants who received group prenatal care, although their costs were lower in the prenatal period. The authors also found no improvements in outcomes for participants in maternity care homes. Lisa Dubay et al., “Improving Birth Outcomes and Lowering Costs for Women on Medicaid: Impacts of ‘Strong Start for Mothers and Newborns,’” Health Affairs 39, no. 6 (June 2020):1042–50.
North Carolina’s Efforts to Address the Nonmedical Drivers of Health
Beginning in 2017, the North Carolina Department of Health and Human Services began building a statewide infrastructure for addressing the nonmedical drivers of health, including food, housing, transportation, employment, interpersonal safety, and toxic stress. This article outlines several interconnected initiatives, which include a standardized screening process to identify people with unmet social resource needs; a statewide network linking health care and human service providers through a shared technology platform; mandates for Medicaid to move toward value-based contracts; and a large-scale Medicaid pilot to evaluate the impact of nonmedical health interventions on health outcomes and health care costs. Zachary Wortman, Elizabeth Cuervo Tilson, and Mandy Krauthamer Cohen, “Buying Health for North Carolinians: Addressing Nonmedical Drivers of Health at Scale,” Health Affairs 39, no. 4 (April 2020):649–54.
Will COVID-19 Finally Prompt U.S. to Address Health Disparities?
In a Viewpoint article, Clyde Yancy, M.D., a cardiologist at Northwestern University’s Feinberg School of Medicine and a Black man, calls for an urgent response to growing evidence that COVID-19 is having a disproportionate effect on African Americans — with a sixfold increase in the rate of death among this group. He notes that while hypertension, diabetes, obesity, and the higher prevalence of cardiovascular disease are likely driving some of the virus’ disparate impacts on Black Americans, where Black people live and other social determinants may also make them vulnerable. A commitment to public health and equity is needed, he says: “The U.S. has needed a trigger to fully address health care disparities; COVID-19 may be that bellwether event.” Clyde W. Yancy, “COVID-19 and African Americans,” Journal of the American Medical Association 323, no. 19 (April 2020):1891–2.
Addressing COVID-19 Risk in Jails and Prisons
To flatten the curve of COVID-19 cases among incarcerated populations and limit transmission both inside correctional facilities and in the community after incarcerated people are released, the authors of this commentary recommend jails and prisons begin releasing those least likely to commit additional crimes, as well as the elderly and infirm; begin segregating those infected and those under investigation for possible infection; and identify correctional staff and health care providers who became infected early and can help with custodial and care effort. They also suggest police and courts suspend arrests and sentences for low-level crimes and misdemeanors. Matthew J. Akiyama, Anne C. Spaulding, and Josiah D. Rich, “Flattening the Curve for Incarcerated Populations – Covid-19 in Jails and Prisons,” New England Journal of Medicine 382, no. 22 (May 2020):2075–7.
Long-Term Buprenorphine Treatment Cuts Hospital, ED Use and Overdose Events
Researchers compared the health outcomes of two groups of Medicaid beneficiaries receiving buprenorphine treatment for opioid use disorder: those whose treatment was discontinued around the National Quality Forum benchmark (six to nine months) and those whose treatment lasted at least 15 months. They found longer-term treatment was associated with relative reductions in the risk of having all-cause inpatient (−52%) and emergency department (−26%) use, opioid-related hospital use (−128%), overdose events (−173%), and opioid prescriptions (−120%) and in the rate of prescription opioid use (−124 %). Hillary Samples et al., “Impact of Long-Term Buprenorphine Treatment on Adverse Health Care Outcomes in Medicaid,” Health Affairs 39, no. 6 (May 2020):747–55.
More PCPs Prescribing Buprenorphine, But Access Barriers Remain
Researchers found buprenorphine prescribing rates by primary care providers increased from 12.9 per 10,000 people in 2010 to 27.4 per 10,000 in 2018. The numbers for psychiatrists and addiction medicine specialists increased from 8.7 to 12.0 per 10,000 and those for other prescribers from 5.8 to 16.3 per 10,000 over the same period. For younger populations (ages 15–24), they found treatment by primary care providers, psychiatrists, and addiction medicine specialists declined significantly. Also, across all patient age and provider groups, most patients were not retained on buprenorphine for the benchmark period of at least 180 days, suggesting patients face ongoing challenges maintaining access to treatment. Mark Olfson et al., “Buprenorphine Treatment by Primary Care Providers, Psychiatrists, Addiction Specialists, and Others,” Health Affairs 39, no. 6 (June 2020):984–92.
An Approach for Understanding How Social Determinants Combine Together to Put People at Risk
In a Viewpoint article, the authors note that researchers’ efforts to quantify precisely how certain social factors, such as income or neighborhood conditions, affect health have failed, mainly because social determinants of health are complex and interconnected. They suggest a new approach, borrowed from the field of genetics in which researchers describe “polygenic risk,” or risks that people will develop certain diseases as a result of multiple interlocking genes. They posit that a “polysocial risk score” may be needed to help researchers understand how various social conditions work together to put people at risk. Jose F. Figueroa, Austin B. Frakt, and Ashish K. Jha, “Addressing Social Determinants of Health: Time for a Polysocial Risk Score,” Journal of the American Medical Association 323, no. 16 (April 2020):1553–4.
Changing How We Pay for Care: Progress After 10 Years
On the 10th anniversary of the signing of the Affordable Care Act (ACA), the authors look back at the law’s efforts to promote new ways of paying for health care, both through direct reforms to Medicare payment and by encouraging broader tests of alternative payment models through the Center for Medicare and Medicaid Innovation. Based on a review of these efforts, the authors conclude that several programs generated some savings and maintained or improved health care quality, though they did not attract sustained participation. There is less conclusive evidence about the impact and spread of alternative payment models. The authors say that the ACA has had moderate success to date. Moving forward, payment reforms that aren’t working should be discontinued and promising models should be further developed. Michael E. Chernew, Patrick H. Conway, and Austin B. Frakt, “Transforming Medicare’s Payment Systems: Progress Shaped by the ACA,” Health Affairs 39, no. 3 (March 2020):413–20.
Comparing Health Care Quality in Community Health Centers, Private Practices
Community health centers, which offer services to all regardless of their ability to pay, are an integral part of the safety net, but does the quality of care their patients receive measure up to that in private practices? Researchers used data from the National Ambulatory Medical Care Survey from 2010 through 2012 to compare how often patients at each of the practices received treatment considered to be of high and low value; the data were adjusted for age, sex, race/ethnicity, insurance, number of chronic illnesses, rural versus urban location, region of country, and survey year. They found that community health centers performed on par with or better than private practices on several measures: community health center clinicians were more likely than those in private practices to order beta blockers for heart failure, or prescribe statins for diabetes. They were also more likely to avoid low-value screening EKGs or urinalyses. The authors conclude that community health centers are well positioned to provide high-value health care. Carlos Irwin A. Oronce and Robert J. Fortuna, “Differences in Rates of High-Value and Low-Value Care Between Community Health Centers and Private Practices,” Journal of General Internal Medicine 35, no. 4 (April 2020):994–1000.
Does the Medical Home Model Function Differently in Different Settings?
Researchers reviewed 64 studies of patient-centered medical home (PCMH) interventions to determine how the types of delivery systems in which PCMHs operate differentially impact outcomes, including measures of utilization, quality, and patient satisfaction. Comparing outcomes for PCMHs in integrated delivery and finance systems (IDFS), government systems including the Veterans Health Administration, and non-integrated delivery systems, they found IDFS studies reported decreased emergency department use, primary care use, and cost relative to other systems after PCMH implementation. Government systems reported increased primary care use relative to other systems. Clinical outcomes, processes, and quality of care as well as patient satisfaction were assessed in different ways, limiting the ability to perform direct comparisons. Clark A. Veet et al., “Impact of Healthcare Delivery System Type on Clinical, Utilization, and Cost Outcomes of Patient-Centered Medical Homes: A Systematic Review,” Journal of General Internal Medicine 35, no. 4 (April 2020):1276–84.
Advance Care Planning Needed Now More Than Ever
In a Viewpoint article, the authors urge clinicians to focus even more on eliciting patients’ goals of care during the pandemic for several reasons. First, patients who are older and have chronic conditions are more likely to develop serious complications from COVID-19 and may find their quality of life unacceptable after life support interventions. Second, avoiding unwanted treatments may be important should health capacity be strained by surges of COVID-19 cases. Finally, provision of unwanted treatment puts health care workers and potentially other patients and family members at risk of virus transmission. J. Randall Curtis, Erin K. Kross, and Renee D. Stapleton, “The Importance of Addressing Advance Care Planning and Decisions About Do-Not-Resuscitate Orders During Novel Coronavirus 2019 (COVID-19),” Journal of the American Medical Association 323, no. 18 (May 2020):1771–2.
Editorial Advisory Board
Special thanks to Editorial Advisory Board member Timothy Ferris for his help with this issue.
Anne-Marie J. Audet, M.D., M.Sc., senior medical officer, The Quality Institute, United Hospital Fund
Eric Coleman, M.D., M.P.H., professor of medicine, University of Colorado
Marshall Chin, M.D., M.P.H., professor of healthcare ethics, University of Chicago
Timothy Ferris, M.D., M.P.H., CEO of Massachusetts General Physician Organization and professor of medicine at Harvard Medical School
Don Goldmann, M.D., chief medical and scientific officer, Institute for Healthcare Improvement
Laura Gottlieb, M.D., M.P.H., assistant professor of family and community medicine, University of California, San Francisco, School of Medicine
Carole Roan Gresenz, Ph.D., senior economist, RAND Corp.
Allison Hamblin, M.S.P.H., vice president for strategic planning, Center for Health Care Strategies
Thomas Hartman, vice president, IPRO
Clemens Hong, M.D., M.P.H., medical director of community health improvement, Los Angeles County Department of Health Services
Lauren Murray, director of consumer engagement and community outreach, National Partnership for Women & Families
Kathleen Nolan, M.P.H., regional vice president, Health Management Associates
J. Nwando Olayiwola, M.D., M.P.H., associate professor of family and community medicine, University of California, San Francisco, School of Medicine
James Pelegano, M.D., M.S., assistant professor of healthcare quality and safety, Thomas Jefferson University
Harold Pincus, M.D., professor of psychiatry, Columbia University
Chris Queram, M.A., president and CEO, Wisconsin Collaborative for Healthcare Quality
Sara Rosenbaum, J.D., professor of health policy, George Washington University
Michael Rothman, Dr.P.H., executive director, Center for Care Innovations
Mark A. Zezza, Ph.D., director of policy and research, New York State Health Foundation
