Abstract
Case studies of three organizations participating in the Institute for Healthcare Improvement's Triple Aim initiative shed light on how they are partnering with providers and organizing care to improve the health of a population and patients' experience of care while lowering—or at least reducing the rate of increase in—the per capita cost of care. The organizations—CareOregon, a nonprofit managed health care plan serving low-income Medicaid enrollees; Genesys Health System, a nonprofit integrated delivery system in Flint, Mich.; and QuadMed, a Wisconsin-based subsidiary of printer Quad/Graphics that develops and manages worksite health clinics and wellness programs—were selected to illustrate diverse approaches. Lessons from these organizations can guide others who wish to undertake or promote transformation in health care delivery.
Introduction to the Triple Aim
In October 2007 the Institute for Healthcare Improvement (IHI) launched the Triple Aim initiative, designed to help health care organizations improve the health of a population patients' experience of care (including quality, access, and reliability) while lowering—or at least reducing the rate of increase in—the per capita cost of care. Pursuing these three objectives at once allows health care organizations to identify and fix problems such as poor coordination of care and overuse of medical services. It also helps them focus attention on and redirect resources to activities that have the greatest impact on health.
Without balanced attention to these three overarching aims, health care organizations may increase quality at the expense of cost, or vice versa. Alternatively, they may decrease cost while creating a dissatisfying experience for patients. Many problems that health care systems face can be linked to one or more of these objectives. Problems like supply-driven care, preventable readmissions, and overbuilding may represent a failure on all three counts.
While easy to understand, the Triple Aim is a challenge to implement. Various forces and traditions have encouraged physicians and hospitals to focus on acute and specialized care over primary and preventive care and to think narrowly about care for particular conditions or episodes of care for individual patients, without considering the health of a population. To achieve the Triple Aim, health care organizations must broaden their focus to organize care to meet the needs of a defined population. Payers, especially those with little direct influence on health outcomes and patient satisfaction, find they must forge new kinds of partnerships with providers. Success requires a willingness to take on new roles and a commitment to honest self-appraisal—otherwise it is easy for health care organizations to continue to work on objectives that play to their existing strengths and neglect those that do not.
In developing the first phase of the Triple Aim initiative, IHI sought out organizations that could serve as prototypes of "macro-integrators" by linking providers across a continuum of care to optimize service for a defined population. Each of these organizations demonstrated a commitment or willingness to bring together different constituencies—including nursing and medicine, medical care and public health, and specialty care and primary care physicians—to accomplish the Triple Aim's goals. These objectives are carried out at the frontlines by "micro-integrators"—the care providers and teams or community organizations that interact with individual patients and families. 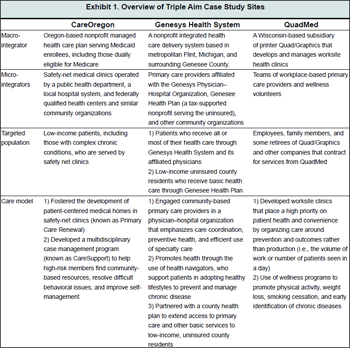
The first group of macro-integrators in the Triple Aim initiative, which began in October, 2007, represented a broad spectrum of health care organizations in the United States, England, and Sweden. It included 15 hospital-based systems, health plans, integrated health systems, public health care departments, safety-net systems, employers, social service agencies, and single-payer national systems. In the summer of 2008, participation in the initiative expanded to 40 organizations, including sites from the U.S. and abroad. In March 2010, IHI embarked on the fourth phase of the project. There are now 60 sites from all over the world participating in the initiative.
IHI helped the participating organizations translate the Triple Aim concept into a specific plan for change. This required each organization to first define the population on which to focus testing and learning activities. Then, each participating site was asked to develop measures of per capita cost, experience of care, and health status for that population. The process shifted the focus away from individual institutions and providers—and their outcomes—to population health. IHI encouraged participants to adapt five principles when designing a new model of care:
- Involve individuals and families when designing care models;
- Redesign primary care services and structures;
- Improve disease prevention and health promotion;
- Build a cost-control platform; and
- Support system integration and execution.
Key Insights
The unique journeys taken by the Triple Aim case study sites highlight the importance of local context as a critical factor in implementing the Triple Aim initiative. On the other hand, common concerns and shared elements across Triple Aim organizations illustrate the fact that the approaches are replicable across care settings with appropriate adaptation. For example, all three sites engaged physicians and other providers (whether employed, contracted, or affiliated) in new ways of delivering care through extrinsic and intrinsic motivators that helped them internalize the goals of Triple Aim.
The methods these organizations used to achieve Triple Aim goals build and expand upon traditional quality improvement and change management techniques to achieve broad system redesign goals, some of which have antecedents in the chronic care model. Many relied on fostering a culture of mutual accountability through transparency in measurement, applying evidence-based standards to improve the quality of care, improving access to primary care and enhancing coordination of care at the patient level, using payment incentives to support patient and provider behavior changes, connecting patients to community resources to meet nonmedical needs, and adapting techniques from other sectors to support more reliable processes.
The distinguishing factor was a population-based approach, which requires building a strong partnership between the macro-integrator organization (health plan, health system, purchaser) and the micro-integrators (care providers or community organizations) to evaluate whether resources were being optimally deployed to meet population needs. It is through these decisions and discussions that defects and perverse incentives can be addressed and cured. As an example, Genesys Health System consolidated and "right-sized" its hospital bed capacity to reduce oversupply in the community. It is now focusing on increasing primary care capacity to support more efficient and effective care, including support for healthy behaviors that reduce the need for expensive acute and specialty care.
Conclusion
As more organizations adopt the goals of Triple Aim and share unique and successful approaches to the challenging problems of coordination of care, chronic disease management, and preventive health, the program is likely to yield more innovations that can be extended to a variety of settings. With time, evidence is likely to accumulate on the effectiveness of such models in improving population health, controlling costs, and improving patients' experience of care. With that combination of experience and evidence, the programs they have pioneered may become more commonplace.
This study was based on publicly available information and self-reported data provided by the case study institution(s). The aim of Commonwealth Fund–sponsored case studies of this type is to identify institutions that have achieved results indicating high performance in a particular area of interest, have undertaken innovations designed to reach higher performance, or exemplify attributes that can foster high performance. The studies are intended to enable other institutions to draw lessons from the studied institutions' experience that will be helpful in their own efforts to become high performers. Even the best-performing organizations may fall short in some areas or make mistakes—emphasizing the need for systematic approaches to improve quality and prevent harm to patients and staff. The Commonwealth Fund is not an accreditor of health care organizations or systems, and the inclusion of an institution in the Fund's case study series is not an endorsement by the Fund for receipt of health care from the institution.


