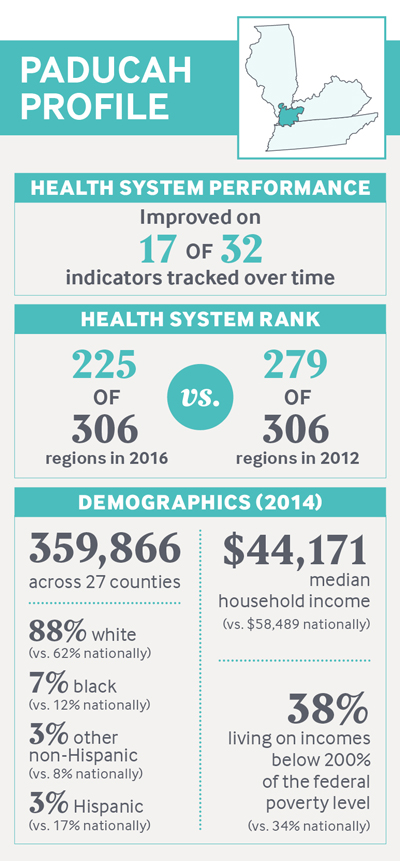
Source: D. Radley, D. McCarthy, and S. L. Hayes, Rising to the Challenge: The Commonwealth Fund Scorecard on Local Health System Performance, 2016 Edition, The Commonwealth Fund, July 2016; American Community Survey, 2014 1-year estimates, www.factfinder.census.gov.
Background
Paducah has a history of reimagining itself. Nearly 20 years ago, this small city at the hub of the nation’s inland waterways on Kentucky’s westernmost border joined a vanguard of U.S. communities that used the arts as an economic engine by offering artists from around the world incentives to purchase and restore dilapidated housing. In what has become the Lower Town Arts District now stand the National Quilt Museum, an 1,800-seat performing arts venue, art galleries, restaurants, and retail shops. This renaissance helped Paducah, a town of just 25,000, garner the fifth-place spot in National Geographic’s 2014 list of World’s Smart Cities.
Murals on the city’s flood barrier commemorate other pivotal moments in Paducah’s history, including a Civil War–era battle that forced the demolition of the Lower Town district and a 1937 flood that forced residents to flee. They also celebrate the ways Paducah has capitalized on its geography with industries built around transportation rather than coal, the decline of which produced economic and social challenges in other parts of the state.
The Paducah region was one of only a handful in the United States to distinguish itself for improving on a majority of indicators tracked by the Commonwealth Fund’s Scorecard on Local Health System Performance, 2016 Edition. In comparing the performance of 306 regional markets for medical care, known as hospital referral regions (HRRs), the Scorecard found wide variation on indicators of health care access, quality, avoidable hospital use, costs, and outcomes across the U.S.
The Paducah HRR improved on 17 of 32 performance measures — elevating its rank from 279th nationally to 225th. This profile is part of a case study series that seeks to understand the drivers of performance on the Scorecard, especially in communities facing socioeconomic challenges. Since the Paducah region was a standout in improving access to care, this case study focuses on the access dimension and the community’s response to the Affordable Care Act.

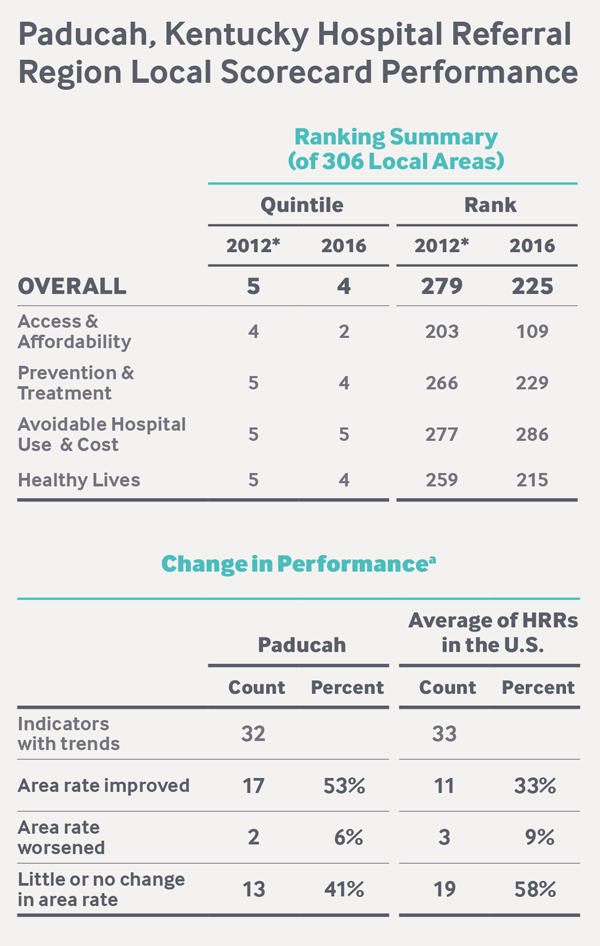
Source: D. Radley, D. McCarthy, and S. L. Hayes, Rising to the Challenge: The Commonwealth Fund Scorecard on Local Health System Performance, 2016 Edition, The Commonwealth Fund, July 2016.
A Stronger Economy Than Other Parts of the State
The Paducah region’s economy revolves around agriculture, professional services, barge companies that ferry goods up the nearby Mississippi, and businesses like Computer Services Inc., which develops the technology banks and financial institutions need to process transactions. “Our economy has a history of being very stable — it doesn’t swing wildly from one extreme to another,” says John Williams, Sr., who founded Computer Services in 1965.
The area is not without its challenges, however. Though not beset with the opioid epidemic that plagues Eastern Kentucky, regional rates of obesity, suicide, and smoking (even among pregnant women) are high. Poverty is also a concern. When Williams observed that the number of children qualifying for free lunches was steadily increasing, he joined other community leaders in forming the Impact Poverty Task Force in 2010. Operating under the aegis of the United Way of Paducah-McCracken County, the task force seeks to address the underlying causes of poverty. One early finding was that poor residents lacked access to medical care.
That has changed with the state’s Medicaid expansion, which tripled the number of adults enrolled statewide.1 With that and other coverage provisions introduced by the Affordable Care Act, the percentage of uninsured adults in the HRR encompassing Paducah declined from 20 percent in 2012 to 12 percent in 2014, according to the Scorecard. Paducah was among the most improved regions in the U.S. on this measure — one of 32 regions where the uninsured rate dropped by 8 percentage points or more. (Kentucky as a whole experienced the greatest reduction of any state in the nation.)
During this period, the Paducah area outpaced the state on other measures of access. Most notably it achieved among the greatest declines nationally in the percentage of adults who went without care because of cost (from 20% to 13%) and at-risk adults who went without a routine medical visit in the past two years (from 17% to 13%).”
New Coverage Leads to New Clinics
Kentucky’s Medicaid expansion, initiated by former Democratic Gov. Steve Beshear in 2014, added close to 500,000 adults to the rolls in a state of roughly 4.4 million.2 By the end of 2015, the uninsured rate for adults ages 19 to 64 in the Paducah region had fallen to 7.8 percent, just below the statewide rate of 8.2 percent — both historic lows.
The Medicaid expansion galvanized efforts to establish federally qualified health centers (FQHCs) in the region, helping to address longstanding shortages of primary care providers that have been particularly acute in the poorer counties that run alongside the Mississippi River. “Previously, we had struggled to get any of the federally qualified health center networks in Kentucky to come this far over from the capitol,” says Brandi Harless, who was elected Paducah’s mayor in November 2016.
Before the Affordable Care Act, the St. Nicholas Family Clinic, a free clinic in Paducah that Harless previously ran, had attempted to fill the gap, relying on a roster of volunteer doctors and nurses and grants from local hospitals to provide medical care to the working poor. With Medicaid expansion on the horizon, clinic and civic leaders reached out to ARCare, an Arkansas-based FQHC operator. The nonprofit had already crossed state lines in 2012 to establish a health center in Bardwell, Kentucky, some 30 miles southwest of Paducah, at the behest of that county’s top elected official.

The free clinic offered its space to the nonprofit, which operates under the banner KentuckyCare, as well as a stipend to cover care for its patients until they could enroll in the Medicaid program. “Had St. Nicholas not been willing to recruit us, it might have taken us longer to get here,” says Emerson Goodwin, KentuckyCare’s corporate regional director. Since 2012, KentuckyCare has opened five clinics in Western Kentucky, including a second clinic in Paducah.
Staffed by physicians and nurse practitioners, KentuckyCare now serves roughly 20,000 patients, 60 percent of whom are covered by Medicaid, up from 30 percent in 2012. In Paducah, it quickly outgrew the St. Nicholas Family Clinic’s space and moved to a new building with twice as many exam rooms, a drive-thru pharmacy, and the latest in X-ray equipment.
KentuckyCare is planning to establish family health centers serving each of the counties that make up the Jackson Purchase, a region bounded by the Mississippi, Ohio, and Tennessee Rivers.

The expansion of coverage and the additional support for FQHCs provided by the Affordable Care Act also encouraged already established health clinics in the area to expand, says David Bolt, deputy director of the Kentucky Primary Care Association, which negotiates insurance contracts for its members, including FQHCs and rural clinics. One was the Pennyroyal Center, a community mental health center, which helped launch an FQHC in Princeton, Ky., in 2013. Health First Community Health Center, which was launched in 2010, opened another clinic early in 2016.
The Medicaid expansion has changed the operations of local free clinics, which have historically limited services to residents who are working but lack insurance. In Calloway County, Angels Community Clinic saw its patient census drop from 600 a year before the expansion to 100 after. “The people who really needed Medicaid seem to have gotten it,” says Heather Glisson, office manager of the clinic, which still provides basic medical services — including exams, diagnostic tests, and prescription medicine — to the working poor with help from volunteer clinicians and support from nearby Murray-Calloway County Hospital. Since the expansion, its focus has been on providing short-term assistance — filling a prescription or arranging for a test at the hospital.
The organization that ran St. Nicholas Family Clinic, meanwhile, has shifted its focus to helping working adults who earn too much to qualify for Medicaid but can’t afford to purchase insurance on their own. “Our clients want to have insurance but have been priced out of the market,” says Rayla Bridges, executive director of the St. Nicholas Healthcare Payment Assistance Program. The nonprofit’s clients receive care from a handful of area providers who offer services at reduced charges and pay between 25 percent and 75 percent of the total bill, depending on household size and income. St. Nicholas makes up the difference. “Our goal is to help clients improve their overall health so they can keep working and ultimately earn their way out of needing us,” Bridges says.
Other Efforts to Increase and Direct Access
During the period the Scorecard tracked — roughly 2011 to 2014 — Lourdes Hospital in Paducah, a 281-bed hospital affiliated with the Mercy Health system, partnered with KentuckyCare in an effort to direct certain patients to the health center. These included uninsured patients, those on Medicaid, and the working poor who used the hospital’s emergency department as a source of primary care. The Purchase District Health Department, which serves five counties including some of the region’s poorest, also employed navigators to help uninsured patients obtain Medicaid coverage if eligible. Together, these efforts may be part of the reason that the region outpaced the state in decreasing the number of at-risk adults who went without a routine doctor visit in the past two years.
Baptist Health, Lourdes’ competitor, which operates two tertiary care hospitals in the region, extended its primary care reach by opening a family medicine practice with two physicians and by committing six nurse practitioners to nine school-based clinics. The clinics provide urgent-care services to students and their siblings, parents, and faculty — billing for services when possible. The local behavioral health agency — Four Rivers Behavioral Health — has deployed staff to the school clinics as well to provide behavioral health services, including substance abuse counseling.
The community also has rallied to improve vaccination rates for the flu, says Michael Muscarella, executive director of ambulatory services for Baptist Health. “We had free flu shot events for the longest time—anyone could come in and get one. Then other providers and pharmacies began similar flu shot programs and, as a result, during the cold and flu season we had very few people in our hospital who were admitted with the flu,” he says. The vaccination push may explain some of the improvement in the percentage of adults with age-appropriate vaccines, which increased from 33 percent in 2011–12 to 38 percent in 2013–14, placing it in the second quintile of hospital referral regions nationwide.
Quality Gains in Hospital Sector
During the Scorecard period, the Paducah region also saw improvements on measures of hospital quality, including risk-adjusted 30-day mortality rates among Medicare beneficiaries hospitalized for heart attack, heart failure, pneumonia, or stroke; a hospital safety composite score; the percentage of patients who were given information about what to do during their recovery at home; and hospitalized patients who reported their pain was managed well.
Being part of a larger hospital system that provides resources for quality improvement initiatives and benchmarking tools has helped, says Catherine Sivills, Baptist Health’s marketing director. “That pushes us all forward,” she says.
An Uncertain Future
While Kentucky’s Medicaid program now covers nearly one of four adults between the ages of 19 and 64, its future is unclear. Beshear’s successor, Republican Gov. Matt Bevin, views the program as financially unsustainable given the state’s pension crisis, its high poverty rates, and low rate of labor force participation. He’s submitted a proposal to restructure it, which would preserve the expansion but require many who are newly covered to contribute to premiums and to work, pursue education, or perform community service to qualify for benefits, a move that could shrink enrollment (see sidebar).
How health care providers and the region as a whole will respond to a possible Medicaid reconfiguration or repeal of other parts of the Affordable Care Act remains to be seen. The pace at which KentuckyCare has opened clinics — one per year since 2012 — may slow to one every two or three years if there is a repeal or restructuring of the program, Goodwin says, but KentuckyCare is committed to the region. “We existed before there was an Affordable Care Act and we’ll exist after the Affordable Care Act or other permutation.…We just won’t get to move as fast as we’d like to serve the residents of Kentucky.”
A History of Collaboration
While the Paducah region’s improvement on the Scorecard reflects its nimble response to the Affordable Care Act, its efforts to invest in the community have been under way for some time and are indicative of strong social ties that can be leveraged to solve problems. These ties may be most apparent in the way local businesses, city and county government, and the philanthropic community in Paducah came together in 2010 to create a scholarship program that provides five semesters of free tuition at West Kentucky Community and Technical College to high school graduates who have at least a 2.5 GPA, a record of good attendance, and no major disciplinary actions. “When a community the size of Paducah can do that, anyone can,” Muscarella says.
The Impact Poverty Task Force also has focused on education, helping to promote literacy in children, as well as building bridges between those in poverty and those who are not so they can better understand one another. Similarly, the community has forged alliances among nonprofits in an effort to reduce duplication of services. Since 2012, charities have been meeting quarterly at a local bank to find opportunities to collaborate, says Monique Zuber, executive director of the local United Way. “People are very giving and they want to see people succeed,” Zuber says.
Community coalitions focused on improving health outcomes — by promoting physical activity, reducing obesity, and addressing social determinants of health — are just getting started. The Rotary Club and the Foundation for a Healthy Kentucky have contributed to building a new health park in a low-income neighborhood, including a playground, outdoor gym, walking trail, and community garden. And the Purchase Area Connections for Health — a coalition of local hospitals, health departments, representatives of city government, the schools, and the United Way — is considering programs to promote community health improvement, including the possibility of pursuing Blue Zones certification for Paducah. (The Blue Zones Project encourages city planners to work with schools and worksites to promote healthy choices in eating and exercise.) Changing health outcomes in Paducah will be a long-term effort, says Goodwin, and it will require more residents to change longstanding behaviors. “You can’t change where you’re ranked nationally if a handful of people change their behavior. You need a bunch of folks to say, ‘Let’s start walking. Let’s start riding. Let’s start running. Let’s put down the cigarette and pull away from the table. All those things that Grandma said — we need to do those things.’”
Lessons
Federal and state policy enabled local action to improve access to care. The Paducah region was able to respond quickly to the state’s Medicaid expansion and take advantage of the infusion of federal funding that accompanied it because local leaders had already identified access as a problem they were committed to addressing. Progress in this area may be compromised by proposed changes to the state’s Medicaid program.
Strong social ties and a record of success in achieving ambitious goals provided a foundation for collective action. Paducah has a history of setting and achieving goals for civic improvement — from attracting world-class artists to building a performing arts center and funding a college scholarship program. Burgeoning efforts to collectively address local health challenges, together with local investments in education and the economy, may pay dividends in improving health outcomes down the line.





