Executive Summary
U.S. health care expenditures have risen rapidly in the last six years, imposing increasing stress on families, businesses, and public budgets. Health spending is rising faster than the economy as a whole and faster than workers' earnings. In recent years, insurance administrative overhead has been rising faster than other components of health spending, while pharmaceutical spending has increased more rapidly than spending on other health care services.
The U.S. spends 16 percent of gross domestic product (GDP) on health care, compared with 8 to 10 percent in most major industrialized nations. The Centers for Medicare and Medicaid Services (CMS) projects that growth in health spending will continue to outpace GDP over the next 10 years. Wide variations in cost and quality across the U.S. underlie these national trends, indicating opportunities to increase efficiency.
This report reviews trends in U.S. health care expenditures in the last 25 years, examines variations in costs, and considers explanations for high costs and fast growth in spending. It then examines strategies that could achieve savings and slow spending growth and discusses their potential for improving overall health system performance.
From a public perspective, the most desirable strategies to address high and rising health care costs would involve: 1) eliminating duplicative or unnecessary care and reducing administrative overhead; 2) preventing illnesses or complications and detecting conditions at an early stage; 3) avoiding unneeded hospitalizations; and 4) enhancing productivity and efficiency in the provision of care. Although there may come a time when the nation is compelled to make a tradeoff between spending on health care and other high priorities, there is currently ample evidence that we can achieve savings and efficient payment, insurance, and care delivery systems and still improve health outcomes, quality of care, and access to care.
Health care costs vary substantially across the United States. For example, the Dartmouth Atlas of Health Care shows that Medicare outlays per beneficiary adjusted for area wage costs ranged from $4,530 in Hawaii to $8,080 in New Jersey in 2003. Yet studies find no systematic relationship between spending more and achieving longer lives or higher quality of care for Medicare beneficiaries. Evidence of extensive variations in costs and quality and studies documenting provision of duplicative, inappropriate, and unnecessary care have led the Institute of Medicine (IOM) and other experts to conclude that the U.S. health care system could improve quality, access, and cost performance. The IOM defines efficiency as achieving the highest level of quality for a given level of resources. Whether comparing U.S. performance to international benchmarks of high value or to benchmarks set within the U.S., it is clear there are opportunities to improve the yield we reap given the resources we invest in health care.
One-time savings are likely to derive from approaches that address factors that contribute to current high levels of U.S. expenditures, inefficiency, and waste. These factors include:
- overuse, inappropriate, or ineffective use of care;
- payment incentives that reward the delivery of more services, without consideration to clinical value or cost-effectiveness;
- market power of insurers, providers, and the health industry, including pharmaceutical companies, device manufacturers, and other suppliers to set prices above competitive market levels;
- a low ratio of primary to specialty care physicians and services;
- access barriers to preventive and primary care that contribute to avoidable hospital admissions, emergency department use, and complications of chronic and acute disease;
- a lack of well-coordinated care that leads to unsafe, duplicative, or conflicting care;
- inadequate information systems and information exchange; and
- high administrative costs, including the high proportion of insurance premiums used to cover overhead costs, the complexity of insurance benefit design and duplicative and uncoordinated requirements, and administrative costs for providers.
The principal factors that contribute to long-term trends in rising expenditures that might be amenable to policy change are somewhat different. They include:
- introduction of new technologies/innovations without comparative information on clinical outcomes or cost-effectiveness to guide decisions on adoption and use;
- wages and prices of other hospital-purchased goods and services;
- growing market power and consolidation of insurers, providers, and the health industry including pharmaceutical companies, device manufacturers, and other suppliers contributing to less choice and higher prices; and
- the increasing prevalence of chronic diseases.
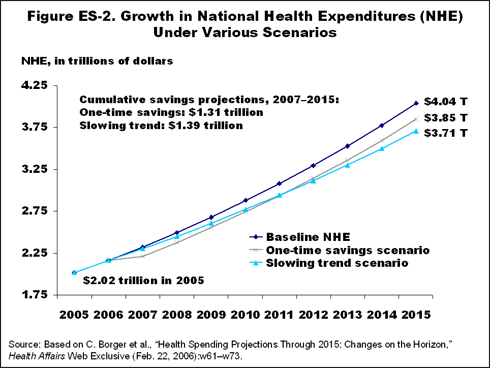
Both strategies that achieve one-time savings as well as those that address cost trends could yield substantial cumulative gains over time. A policy option that has the effect of achieving a one-time reduction in the level of health care spending by 5 percent in 2007 would achieve cumulative savings over the eight-year period from 2007 to 2015 of $1.31 trillion. A policy option that has the effect of lowering the average rate of increase in health care outlays by one percentage point a year would yield cumulative savings of $1.39 trillion over the same period. In combination, one-time changes in spending levels plus even small changes in projected rates of increase interact to produce even more substantial long-term yields (Figure ES-2).
To achieve long-term gains in efficiency, new policies will need to counteract factors contributing to high levels of spending, poor quality, and inefficient care, as well as factors contributing to upward pressures on expenditures over time. Potential strategies to move the U.S. to a higher value, more efficient health care system cluster into six main areas:
- increasing the effectiveness of markets by improving access to information on the quality and costs of care, promoting greater competition, and developing better information on the cost-effectiveness of health care technology and procedures;
- reducing high insurance administrative overhead and achieving more competitive prices;
- providing payment incentives to promote efficient and effective care;
- changing the health care system to promote patient-centered primary care;
- investing in infrastructure such as health information technology and information exchange systems; and
- investing strategically to improve access, affordability, and equity.
Effective policy options should focus on changing total national expenditures rather than simply shifting costs from one payer source to another. Some policies may have a greater effect on federal budget outlays, while others may affect outlays by state government, employers, or households. Achieving improved value for the national investment in health care requires policies that achieve net gains for the whole country. At the national level, the policies should:
- be amenable to federal policy action;
- improve health outcomes, quality, access, efficiency, or equity;
- have a high likelihood of significant reduction in expenditure levels and/or trends compared with current projections, or achieve a net improvement in value;
- be evidence-based and feasible to implement; and
- be reasonable first steps toward longer-term reforms.
At the federal level, there are a range of legislative proposals that seek to improve efficiency and contain health expenditures. Legislative proposals which have been introduced in Congress address four major areas: simplifying, standardizing, and introducing negotiated pricing into Medicare Part D; enhancing the utilization of health information technology and building a national interoperable technology system; integrating value-based purchasing into Medicare payments; and improving public access to information on the quality and price of medical services.
There is a compelling need for a coherent public and private sector strategy, with all parties working in concert toward agreed-upon health system aims. Such a strategy should place high priority on policies and practices that have the potential to move our nation toward benchmark levels of performance on access, quality, and efficiency, so that the U.S. health system could achieve commensurate value for the significant resources it commands.
