Presidential candidates, governors, and members of Congress are advancing proposals to address the nation's most important health policy issue: the steady increase in the number of uninsured individuals. This is a welcome development, and augurs well for reversing the steady climb in the numbers of uninsured. Since 2000, the number of uninsured has increased by more than 20 percent, reaching 47 million in 2006. In addition, rising health care costs are squeezing many middle-income Americans with insurance, who report difficulties paying medical bills due to a lack of adequate coverage.
Extending health insurance coverage to all Americans is the most important step in improving access to quality health care. However, there is also an opportunity to achieve this goal in a way that helps the United States achieve a high performance health system that simultaneously yields better access, higher quality, and greater efficiency. This report, prepared for The Commonwealth Fund Commission on a High Performance Health System, investigates the ways in which our current health insurance system fails to promote high performance in the areas of access, equity, quality, efficiency, and cost control. It explains why universal coverage is essential to improving performance measures in each of these core areas. The report also describes the different ways in which policymakers may design universal coverage and how each option will have long-range implications for the system's ability to consistently achieve higher-quality and more efficiently delivered care, as well as its ability to gain control over health care cost growth.
The report presents principles for health insurance reform to help the public assess proposals based not only on their ability to achieve universal coverage, but also on their potential to move the nation's health care system toward high performance. It outlines the questions that all Americans should consider in evaluating the reform proposals suggested by federal and state policy leaders, and it contrasts proposals built around three distinct philosophies:
- Tax incentives for individual market insurance. Proposals that rely primarily on individuals' responsibility for obtaining coverage, with tax incentives to subsidize purchase of insurance in the individual insurance market.
- Mixed privatepublic group insurance with shared responsibility for financing. Proposals that build on our current mixed privatepublic system of health insurance with shared responsibility for financing coverage by government, employers, and households.
- Public insurance. Proposals that would cover nearly all Americans under public insurance programs, such as Medicare, with everyone covered through the same public system.
In the Commission's view, both the mixed privatepublic group insurance and the public insurance reform proposals have the greater potential to move the health care system toward high performance. Both approaches have the potential to provide everyone with comprehensive and affordable health insurance, achieve greater equity in access to care, realize efficiencies and cost savings in the provision of coverage and delivery of care, and redirect incentives to improve quality. From a pragmatic perspective, however, the mixed privatepublic approach would cause far less dislocation by allowing the more than 160 million people who now have employer-based health coverage to retain it, instead of asking them to enroll in a new program. This approach would build on the best features of our current system while addressing its most serious shortcomings: gaps in coverage and the absence of the incentives, organization, and infrastructure required for a high performance health system.
Why Does the Current Health Insurance System Fail to Promote High Performance?
Access to Care Is Unequal. The most important determinant of access to health care is adequate health insurance coverage. People with low and moderate incomes are most at risk of lacking coverage through an employer and most at risk of being uninsured. They also spend the largest share of their incomes on premiums and out-of-pocket health care costs.
Poor Access to Care Is Linked to Poor Quality. People who lack health insurance are much less likely to have a regular source of care, use fewer and less appropriate health services, are less likely to receive timely preventive and screening services, are less likely to receive appropriate care for management of their conditions, and have worse clinical outcomes. People without coverage have both poorer health status and shorter life expectancies.
Care Delivery Is Inefficient. Lacking adequate coverage impedes the delivery of efficient care once a person without coverage enters the health care system. Uninsured adults report the highest rates of test results or records not being available at the time of their appointment, as well as the highest rates of receiving duplicate tests. Physicians also report inefficiencies in securing pharmaceuticals and follow-up medical care for uninsured patients.
A Fragmented Health Insurance System Makes It Difficult to Control Costs. The U.S. spends a far greater share of its gross domestic product on health care and its citizens spend more out-of-pocket than other industrialized countries, which all have universal health insurance. The highly fragmented way in which we purchase health services in the U.S. allows prices to climb above those in other industrialized nations. In addition, a significant percentage of the cost of health insurance goes toward administrative activities. An estimated 10 percent to 40 percent of premiums is consumed by claims administration, underwriting, marketing, profits, and other administrative costs. Costs of insurance administration are the fastest-growing component of U.S. national health expenditures.
Financing of Care for Uninsured and Underinsured Families Is Inefficient. The total costs of uncompensated care in the United States were nearly $41 billion in 2004. This figure would be far higher if uninsured people received as much health care as insured people do. Uninsured adults and children receive just 55 percent of the medical care that those who are insured for the full year receive. Research suggests that private payers finance uncompensated care costs that are not covered by public funds through surcharges to private payers, ultimately resulting in higher private insurance premiums. Estimates of this "hidden tax" range from 8.5 percent of premiums nationally to up to 10.6 percent in California.
Positive Incentives in Benefit Design and Insurance Markets Are Lacking. Incentives in benefit design and in provider reimbursement are not consistently aligned to encourage the use of effective services, discourage the use of ineffective services, and reduce over-utilization, duplication, and waste. Adverse selection encourages insurance companies to expend considerable resources avoiding health risks in the small group and individual insurance markets.
Design Matters: Key Principles to Consider in Developing and Evaluation Health Reform Proposals
Extending health insurance coverage to people who currently lack it is a necessary, but not sufficient, condition for achieving high performance. The way in which a universal coverage system is designed will have a deep impact on its ability to make sustainable and systematic improvements in access to care, equity, quality of care, efficiency, and cost control. With these goals in mind, the following are some key principles policymakers and the public should consider in developing or evaluating health reform proposals:
Access to Care
- Provides equitable and comprehensive insurance for all.
- Insures the population in a way that leads to full and equitable participation.
- Provides a minimum, standard benefit floor for essential coverage with financial protection.
- Premiums, deductibles, and out-of-pocket costs are affordable relative tofamily income.
- Coverage is automatic and stable with seamless transitions to maintain enrollment.
- Provides a choice of health plans or care systems.
Quality, Efficiency, and Cost Control
- Health risks are pooled across broad groups and over lifespans; insurance practices designed to avoid poor health risks are eliminated.
- Fosters efficiency by reducing complexity for patients and providers, and reducing transaction and administrative costs as a share of premiums.
- Works to improve health care quality and efficiency through administrative reforms, provider profiling and network design, utilization management, pay-for-performance payment models, and structures that encourage adherence to clinical guidelines.
- Minimizes dislocation; people can maintain current coverage if desired.
- Simple to administer.
- Has the potential to lower overall health care cost growth.
Financing
- Financial commitment to achieve these principles.
- Financing should be adequate and fair, based on ability to pay, and is a shared responsibility of federal and state governments, employers, individual households, and other stakeholders.
Current Proposals for Health Insurance Reform
Current proposals to reform the health insurance system include: strategies that emphasize tax incentives for obtaining insurance through the individual market; proposals that build on existing privatepublic group insurance with a shared responsibility for financing coverage; and proposals to cover everyone through public forms of insurance, like Medicare.
Tax Incentives for Individual Market Insurance. Proposals by President George W. Bush, former New York City mayor Rudy Giuliani, Senator John McCain (RAriz.), and former Massachusetts governor Mitt Romney would create tax incentives for people to gain coverage through the individual insurance market.
Mixed Private-Public Group Insurance with Shared Responsibility for Financing. The state of Massachusetts, Governor Arnold Schwarzenegger of California, and five Democratic presidential candidates (Senators Hillary Clinton (DN.Y.), Christopher Dodd (DConn.), and Barack Obama (DIll.), former North Carolina Senator John Edwards (DN.C.) and New Mexico Governor Bill Richardson) have either proposed plans or passed lawsin the case of Massachusettsfor universal coverage that maintain and build on the current mixed private and public insurance system. Most include requirements for individuals to purchase coverage and for employers to offer or help pay for coverage, expansions in Medicaid and State Children's Health Insurance Program (SCHIP), and new group insurance options with financial support for premiums and out-of-pocket expenses for lower- and middle-income households.
Public Insurance. Representative Pete Stark (DCalif.), Senator Edward Kennedy (DMass.), Representative John Dingell, (DMich.), Representative John Conyers (DMich.), and Representative (and presidential candidate) Dennis Kucinich (DOhio) have proposed universal coverage plans in which Medicare or a new government plan plays a central role.
Which Strategies Have the Greatest Promise to Move the System to High Performance?
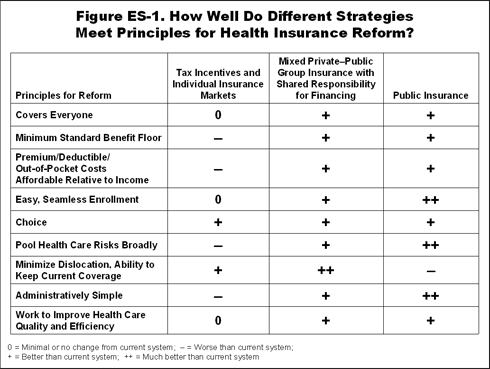
Assessing the health insurance reform proposals against the key principles described earlier helps to illustrate each proposal's strengths and weaknesses (Figure ES-1).The proposals, which reflect different philosophical strategies and values, use a range of mechanisms to address health system issues of inadequate access to care, variable quality, and high cost. Design features of the three different approaches have significant implications for each of these issues, including the number of people covered, the cost to stakeholders and the overall health system, equity in access and financing, and improvements in efficiency and quality. Raising the right questions and weighing the evidence will help shape consensus.
Tax Incentives for Individual Market Insurance
Reform proposals that rely on tax incentives and voluntary purchase of coverage in the individual insurance market are, on their own, unlikely to achieve universal coverage (Figure ES-1). Buying coverage in the individual market will continue to be challenging if tax incentives are not coupled with an individual mandate, minimum benefit standards, regulations against risk selection, and premium and out-of-pocket spending limits as a share of income. Providing incentives for coverage in the individual market without an individual mandate or regulations against risk selection would not pool risks. Insurers would still write individual policies rather than policies for a broad group of people. With administrative costs in the individual market running from 25 percent to 40 percent of premium dollars compared with 10 percent in employer group markets and 2 percent in Medicare, covering more people through this market would only fuel growth in annual administration costs.
Supporters of these proposals argue that consumers spending their own money on health insurance and health care would be more cost-conscious, seek out lower cost providers, and avoid marginal or unnecessary care. These proposals would allow substantial choice of covered benefits and financial protection within the limits of people's budgets. However, they could limit options and increase costs for those with health risks, depending on existing consumer protections, which vary by state. People with preexisting conditions might face very high premiums, might be unable to get their health needs covered, or might not be offered a policy at all. If designed to avoid undermining employer-based coverage, the proposals would cause minimal dislocation with the ability to maintain current health insurance coverage.
These proposals would do little to alter incentives to improve health care quality and efficiency. From a financing perspective, the lack of risk pooling and higher administrative costs would inflate the size of tax credits necessary for making premiums affordable for lower-income people.
Mixed PrivatePublic Group Insurance with a Shared Responsibility for Financing
Most proposals that build on the current system would ensure universal coverage by requiring that all individuals purchase coverage and that employers either provide coverage to employees or contribute to premiums. Such mandates would be critical to ensure everyone is covered (Figure ES-1). Most proposals would also create new group insurance options, sometimes referred to as "exchanges" or "connectors" for people without access to employer coverage and for small businesses. These new health insurance exchanges would allow consumers a choice of private and public plans. Offering a public plan option like Medicare in these new health insurance exchanges would give individuals and businesses the ability to choose between private and public health plans. Most proposals specify a minimum standard benefit package for plans offered by employers and through the health insurance exchange.
Affordability of coverage would be assured through expansion of Medicaid and SCHIP for lower-income families and provision of premium assistance for lower- and middle-income people buying coverage in the new health insurance exchange. However, it is important that potential out-of-pocket costs also be taken into consideration when defining affordability under a mandate.
By building on multiple forms of existing group coverage and adding a new group insurance option, these proposals, on their own, would not make enrollment easier or more seamless. They would also retain much of the complexity of the current system. Automatically enrolling people through the tax system under an individual mandate would help ensure that people become and remain enrolled. The income tax system can also provide an administrative mechanism for income-related premium assistance and ceilings on out-of-pocket costs as a percentage of income.
These approaches would pool risk by building on the large risk pools of the employer market and public programs and create new health insurance exchanges with regulations against risk selection. The actual design of the new health insurance exchanges will be important, however, with respect to the restrictions against risk selection, the type of plans available for consumers, the extent of income-related subsidies and whether both out-of-pocket costs and premiums are taken into consideration when determining the amount a family pays.
By building on the current system, these proposals would cause minimal dislocation. People could keep their employer coverage as long as it met minimum benefit and affordability standards. By replacing small group or individual market coverage with coverage through health insurance exchanges or public programs, administrative savings could be achieved. If Medicare, Medicaid/SCHIP, and employer coverage were redesigned to reward health care providers for higher quality or more efficient care, even further savings are possible. Success will depend on effective national leadership, collaboration between the public and private sectors, and the creation of the information and infrastructure including information technology.
Financing would be a mix of federal and state general revenue taxation, employer and individual premium contributions, and modest cost-sharing. Subsidies for low-income families would offset all or part of their premium and out-of-pocket costs; broad risk pooling would help keep the size of subsidies low. The financial distribution of costs is likely to be closely proportional to earnings, and more progressively shared than financing under most approaches that provide tax incentives for coverage through the individual market. Some proposals would fund the federal portion of costs by repealing or not renewing tax cuts for higher-income households, thereby increasing the progressive nature of the overall financing.
Public Insurance
Public insurance programs offer the greatest potential for automatic and continuous enrollment and the ability to cover everyone (Figure ES-1). Enrollment could be facilitated through local Medicare or Social Security offices. Those failing to enroll could be signed up when they seek health care services or coverage could be verified as part of income tax filing. With everyone eventually enrolled at birth in an expanded Medicare, people would automatically be enrolled and stay enrolled across their lifespans. Most proposals would establish a minimum standard benefit package modeled on the typical plan offered to members of Congress or to employees of large firms. For those proposals requiring enrollees to pay cost-sharing or a portion of premiums, a ceiling on out-of-pocket costs and premiums as a percentage of income would be established to ensure affordability. Some proposals modeled, for example, on the Canadian health systemwould not include patient cost-sharing for basic services and would be financed by federal and state taxes.
Given Medicare's low administrative costs and broad risk pooling, substantial savings could accrue in an expanded Medicare approach through a reduction in administrative costs. Other sources of savings would likely arise from paying providers Medicare rates that are lower, on average, than private rates.
The proposals modeled on the current Medicare program would provide choice of plans, including the private plan options currently available to Medicare beneficiaries and the program's self-insured plan.
The public insurance approaches to health insurance reform would create dislocation, with people moving from their current coverage to coverage through Medicare or another public plan. However, people would still likely keep their same set of providers. Proposals that would allow employers to continue offering coverage would be less disruptive initially, although it is anticipated that most employers would ultimately prefer to pay a part of the Medicare premium rather than private coverage premiums, which would probably be higher.
These proposals would allow the nation to develop and utilize common quality metrics, gather data on the health care outcomes of the full population, and evaluate and improve the performance of providers based on a large pool of patients not fragmented by insurance type. They also would allow for the creation of uniform provider payment systems that reward high-quality care, standardization in health information technology, and the creation of universal processes to improve safety systematically across healthcare institutions.
Financing is likely to come largely from federal income and payroll taxes or new taxes, such as a value-added tax or consumption tax. This would be less administratively complex than providing premium subsidies based on income. The distribution of financing is most likely to be more progressively related to income than either individual insurance market or mixed privatepublic group insurance proposals.
Conclusion
Ultimately, we must move the health care system to high performance using goals and properly aligned incentives that orient all participants in the same direction: toward improved access, quality, equity, and efficiency. The most important feature of any health insurance reform proposal is whether it can succeed in providing health insurance and access to care to all. In addition, proposals should be examined for their ability to produce better access, higher quality, and greater efficiency. Whenever possible, we must seek synergy between coverage expansion and reform that will move the U.S. to a high performance health system.
Achieving universal coverage will require engaging everyone in a debate on values, our commitment to a healthy and productive life for all, and the merits of different strategies for achieving improved coverage and better performance from our health system. This guide is offered to both underscore the importance of such reforms and to help shape the debate and emerging consensus on future directions for the U.S.
Serious reform will require broad consensus and a significant financial investment by federal and state governments, employers, households, and other stakeholders. A shared responsibility among all stakeholders will be needed to achieve the goals of reform in a way that is effective and fair.
