Abstract
States have flexibility in implementing the Affordable Care Act’s health insurance marketplaces and may choose to become more (or less) involved in marketplace operations over time. Interest in new implementation approaches has increased as states seek to ensure the long-term financial stability of their exchanges and exercise local control over marketplace oversight. This brief explores the experiences of four states—Idaho, Nevada, New Mexico, and Oregon—that established their own exchanges but have operated them with support from the federal HealthCare.gov eligibility and enrollment platform. Drawing on discussions with policymakers, insurers, and brokers, we examine how these supported state-run marketplaces perform their key functions. We find that this model may offer states the ability to maximize their influence over their insurance markets, while limiting the financial risk of running an exchange.
BACKGROUND
The Affordable Care Act (ACA) provides for the creation of health insurance exchanges, known as marketplaces, where consumers can shop for a health plan and apply for federal subsidies to help pay for coverage. The health law specifies the core features of each marketplace—for example, they must be financially self-sustainable—and gives states the option to create their own exchange (a state-based marketplace) or leave that responsibility to the federal government (a federally facilitated marketplace).1 Sixteen states and the District of Columbia have established their own marketplaces, while a federally run version operates in the remaining 34 states.
Federal regulations and guidance issued since the ACA’s passage have fleshed out the law’s marketplace framework. These rules spell out a range of functions, from eligibility and enrollment, to consumer and stakeholder engagement, to health plan management.2 Over time, they also have given form to new marketplace models that promote shared responsibility between states and the federal government for exchange operations.3 Through this adaptive approach, federal officials have sought to allow states flexibility to tailor their involvement with the marketplaces to suit local needs.4
As options for implementation have evolved, state approaches to marketplace establishment and operations are changing, too. For example, state officials may seek to regain autonomy over regulatory and policymaking decisions or to give consumer outreach and assistance efforts a more local feel. Alternatively, states looking to rebound from earlier technology system failures, or to place their exchange on more solid financial footing, may wish to leverage certain federal operations.
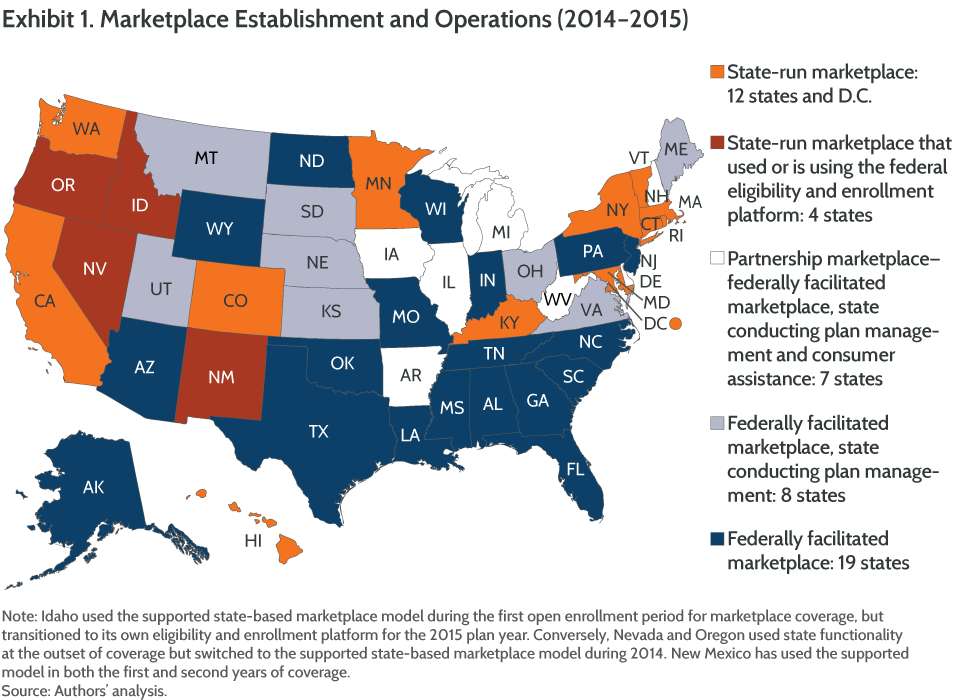
Whether their exchange is state-based or federally facilitated, many policymakers are seeking ways to realize the advantages of a state-run model while minimizing, so far as possible, the financial and operational burdens of building or maintaining one. Interest has therefore focused on the experiences of states that established their own exchanges but have worked with the federal government to operate them.5 These “federally supported state-based marketplaces” are similar to other state-run exchanges except that they use the federal HealthCare.gov platform for eligibility and enrollment instead of state technology. To date, four states—Idaho, Nevada, New Mexico, and Oregon—have chosen this course for one or more years of marketplace coverage, with a fifth, Hawaii, slated to adopt the model for 2016 (Exhibit 1).6
This brief describes the operations of these supported exchanges. Drawing on discussions with policymakers, insurers, and brokers in the four states that have used the model so far, we examine how these marketplaces perform critical functions and describe the advantages and limitations for consumers and other stakeholders.
KEY CHARACTERISTICS OF SUPPORTED STATE-BASED MARKETPLACES
Legal Authority and Governance
The four states that have used the supported state-based model came to it from different directions. Idaho and New Mexico established their exchanges relatively late—in early 2013, two years after most states acted—and relied on federal eligibility and enrollment technology to facilitate an on-time launch of the first open enrollment period (Exhibit 2).7 Idaho subsequently created its own systems for the second year of coverage, while New Mexico continues to use the federal HealthCare.gov platform. By contrast, Nevada and Oregon converted to the federal technology after state-contracted systems failed to perform during year 1.
Exhibit 2. Supported State-Based Marketplaces: Legal Authority and Governance
| Legal authority establishing the marketplace |
Marketplace structure and governance mechanism |
|
| Framework | States must have legal authority to establish a marketplace. States may obtain requisite authority through legislation or, in some cases, executive action. |
ACA requires marketplace to be governmental agency or nonprofit entity established by state. States have discretion over where to house their marketplace (e.g., outside a traditional state agency or within one, like a state Medicaid office or insurance department) and how to govern it. |
| State | ||
| Idaho | Legislation (House Bill 248, enacted 2013) |
Quasi-governmental entity governed by independent 19-member board.* |
| Nevada | Legislation (Senate Bill 440, enacted 2011) |
Independent public entity housed within own newly created governmental agency. Governed by independent 10-member board. |
| New Mexico | Legislation (Senate Bill 221, enacted 2013) |
Quasi-governmental entity governed by independent 13-member board.* |
| Oregon | Legislation (Senate Bill 99, enacted 2011; modified by Senate Bill 1, enacted 2015) |
Originally established as quasi-governmental entity governed by independent nine-member board.* In 2015, state abolished original marketplace entity and transferred its duties, functions, and powers to an existing state agency, the Department of Consumer and Business Services. |
| Remaining state-based marketplaces |
Legislation in 10 states and DC (CA, CO, CT, DC, HI, MA, MD, MN, RI,† VT, WA) Executive action in two states (KY, NY) |
Quasi-governmental entity in seven states and DC (CA, CO, CT, DC, MA, MD, MN, WA) Existing state agency in four states (KY, NY, RI, VT) Private nonprofit in one state (HI) |
Note: Idaho used the supported state-based marketplace model during the first open enrollment period for marketplace coverage, but transitioned to its own eligibility and enrollment platform for the 2015 plan year. Conversely, Nevada and Oregon used state functionality at the outset of coverage but switched to a supported state-based marketplace model during 2014. New Mexico has used the supported model in both the first and second years of coverage.
* Marketplaces described as “quasi-governmental” are public entities exempt from many, but not all, of the administrative and other legal requirements applicable to traditional state agencies. The actual legal designation that attaches to these entities varies by state: Idaho (“independent body corporate and politic”); New Mexico (nonprofit public corporation); and Oregon (public corporation).
† Rhode Island’s governor used an executive order to establish a state-based marketplace in 2011. Legislation enacted in June 2015 provided statutory authority for the exchange.
Sources: The Affordable Care Act, §§ 1311(d) & 1321(b); authors’ analysis.
To establish a marketplace, the ACA requires that a state “elect” to do so; policymakers must want to pursue a state-based path.8 Despite their differences, all four states adopted the supported model for the same reason: because state leaders believed it gave them the best opportunity, in a rapidly changing regulatory environment, to retain local control over their markets.9
Eligibility and Enrollment
The chief feature distinguishing supported state-based marketplaces from other state-run exchanges is how they handle eligibility and enrollment. Rather than using state technology for these functions, the supported model relies on the federal HealthCare.gov platform to determine consumers’ eligibility for marketplace coverage and subsidies, and to facilitate and process enrollment. These federal functions are then paired with the supported marketplaces’ own branded websites (New Mexicans may navigate to beWellnm.com, for example) and call centers. The state resources provide information about marketplace coverage and assistance opportunities, then deliver consumers to HealthCare.gov or the federal call center to obtain an eligibility determination and shop for plans.
Policymakers and stakeholders reported positive experiences with this arrangement. Despite the initial failures of HealthCare.gov early in the first open enrollment period and the complications posed by the (then unprecedented) transition between state and federal platforms in Idaho, Nevada, and Oregon, respondents were largely satisfied with the federal system’s functionality.10 Simply put, after the early rollout problems were over, the federal site worked—which was not fully the case in the two states that suffered setbacks with their own technology.
This generally favorable view finds support in marketplace enrollment data. Idaho’s enrollment via the federal platform in 2014 far surpassed observers’ projections.11 Meanwhile, the three current supported marketplaces experienced an influx of sign-ups in year 2 that exceeded the average for states using HealthCare.gov (Exhibit 3).
Exhibit 3. Marketplace Enrollment in 2014 and 2015, by Enrollment Platform

| State | 2014 marketplace enrollment* |
2015 marketplace enrollment* |
Percentage change in enrollment (2014–2015) |
| Idaho | 76,061 | 97,079 | 27.6% |
| Nevada | 45,390 | 73,596 | 62.1% |
| New Mexico | 32,062 | 52,358 | 63.3% |
| Oregon | 68,308 | 112,024 | 64.0% |
| All other states using HealthCare.gov |
61.1% | ||
| All other states using own marketplace platforms |
11.9% |
Notes: Idaho used the supported state-based marketplace model during the first open enrollment period for marketplace coverage but transitioned to its own eligibility and enrollment platform for the 2015 plan year. Conversely, Nevada and Oregon used state functionality at the outset of coverage but switched to a supported state-based model during 2014. New Mexico has used the supported model in both the first and second years of coverage.
* Data represents the total number of individuals who have selected a marketplace plan by the close of each year’s open enrollment period.
Sources: Enrollment data comes from the Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation (ASPE), as compiled by the Urban Institute; authors’ analysis.
The federal platform has limitations. First, states lack authority over its design and layout and cannot control when the website is available for consumers to access. Federal policy and operational decisions directly related to the technology—use of consumer decision-support tools, for example, or flexibility regarding special enrollment periods—become the state’s own by default. While most respondents in the supported marketplace states do not currently feel constrained by federal choices, some expressed hope that the technology could be customizable over the longer term.
Second, use of the federal platform limits the ability of states to integrate eligibility processes for marketplace financial assistance with those for Medicaid. Though the experience for these marketplaces and their consumers is no different from that in other states using HealthCare.gov, supported state-based exchanges lack the option of a seamless “single door” eligibility and enrollment system for insurance affordability programs akin to those built successfully elsewhere, like Kentucky.12
Consumer Outreach and Assistance
Similar to other state-based marketplaces, Idaho, Nevada, New Mexico, and Oregon provided consumers with informational services related to the ACA and its coverage options as well as personalized enrollment assistance. In addition to operating their own branded websites and call centers, these marketplaces trained and certified community-based enrollment counselors, facilitated connections between consumers and brokers, and conducted marketing and outreach campaigns.13
Policymakers in the supported marketplace states repeatedly emphasized the critical importance of tailoring outreach and assistance to their states’ diverse populations and needs.14 Senior staff from New Mexico suggested that localized outreach, particularly in underserved areas, has helped generate significantly higher enrollment both in their state and nationwide.
These positives notwithstanding, respondents identified two areas where improvements in state–federal collaboration might benefit consumers. First, because they use the federal platform, supported marketplaces do not own, and lack prompt access to, the granular application and enrollment data that other state-run marketplaces obtain as a matter of course. This lack of information means that, for all their efforts to design focused outreach strategies, these exchanges are comparatively limited in their ability to understand and analyze their markets. While they may have access to some data on delay or from other sources—insurance departments in several states sought data directly from their carriers, for example—the issue remains of concern to state policymakers, and efforts with federal officials to resolve it are ongoing.
Second, a byproduct of federal responsibility for eligibility and enrollment is that consumers who have specific questions or difficulties regarding the sign-up process must contact the federal call center for support. While stakeholders’ experiences with the federal call center varied, many were critical of the level of service it has provided.15
Health Plan Management
The ACA requires marketplaces to regulate and certify the health plans they make available for sale.16 This “plan management” encompasses numerous activities (Exhibit 4). However, state agencies were already performing many of these tasks prior to health reform, and of those elements that are new, much applies to the regulation of insurers selling outside the exchanges, as well.17 Given that these activities are a natural extension of states’ historical role in regulating insurance—and that many state policymakers seek to avoid ceding oversight authority to the federal government wherever possible—most states, regardless of exchange model, are choosing to perform as many of these functions as possible. Fifteen states with federal marketplaces have responsibility for these tasks (though they do not have the final call on plan certification, which belongs to federal officials in non-state-based exchanges). The supported marketplaces, like other state-run exchanges, are exercising full plan management authority, largely through delegation to state departments of insurance.
Exhibit 4. Marketplace Health Plan Management: Selected Activities
| Plan management activity | Description |
| Confirm state licensure and solvency |
Marketplace must confirm that each participating insurer is licensed and in good standing in state in which coverage is offered. |
| Certify marketplace plans | Each marketplace plan must meet minimum set of certification criteria related to marketing practices, provider networks, care quality, and transparency. Marketplace must implement processes for determining whether plans satisfy these criteria and for awarding certification. |
| Review justifications of rate increases |
Marketplace must require plans seeking certification to justify any premium rate increase prior to increase being implemented; this justification, along with any state insurance department recommendations regarding rate increases, must be considered as part of approval process for plans’ participation on the exchange. |
| Review compliance with rating and benefits requirements |
Marketplace must ensure that participating plans comply with ACA’s premium rating restrictions and requirements pertaining to covered benefits and cost-sharing. |
| Provide ongoing compliance monitoring |
Marketplace must implement a process for recertifying (or decertifying) plans and conduct ongoing oversight to ensure insurer compliance. |
| Manage a selective contracting process (if desired) |
Marketplace must ensure that each plan’s participation is in interest of consumers and small businesses. At discretion of state policymakers, exchanges may choose to further this objective by engaging in selective contracting. |
Note: Under the ACA and its implementing regulations, ultimate responsibility for plan management functions rests with the exchange. However, exchanges may delegate authority for one or more of these activities to an eligible entity, most commonly in the case of plan management, to the state’s department of insurance.
Sources: The Affordable Care Act, §§ 1301(a), 1311(d)(4)(A), and 1311(e); 45 C.F.R. § 155.1000 et seq.; S. Corlette, J. Volk, and K. Lucia, Plan Management: Issues for State, Partnership and Federally Facilitated Health Insurance Exchanges (Princeton, N.J.: Robert Wood Johnson Foundation, May 2012).
Financial Sustainability
Initial development of the 17 state-based marketplaces was financed largely through federal start-up grants authorized by the ACA.18 These funding opportunities were, however, time-limited: the health law prohibited new grants after January 1, 2015, requiring marketplaces to be self-sustaining after that date.19
The ACA gives states that set up their own exchanges broad discretion over mechanisms to achieve sustainability. States may fund their marketplaces through ordinary budget appropriations, for example, or even through sale of ancillary products or website advertising. At present, however, most are financed predominately through an assessment on health plans.20 Three of the study states raise revenue from fees levied on plans sold through their exchanges; New Mexico, by contrast, assesses all major medical plans, including Medicaid managed care plans, sold on and off its exchange (Exhibit 5).
Exhibit 5. Supported State-Based Marketplaces: Financial Sustainability Mechanisms
| Insurer assessment levels: percent of premium or per member per month (PMPM) fee |
||||
| State | Primary long-term revenue source |
2014 | 2015 | 2016 |
| Federally facilitated marketplace |
Assessment on plans offered through marketplace |
3.5% | 3.5% | 3.5% |
| Idaho | Assessment on plans offered through marketplace |
1.5% | 1.5% | 1.99% |
| Nevada | Assessment on plans offered through marketplace |
$4.95 PMPM | $13.00 PMPM | 3.0% |
| New Mexico | Broad-based assessment on plans offered on and off marketplace* |
N/A | Assessment pegged to insurer market share and marketplace operating expenses |
Assessment pegged to insurer market share and marketplace operating expenses |
| Oregon | Assessment on plans offered through marketplace† |
$9.38 PMPM | $9.66 PMPM | To be determined |
Note: Idaho used the supported state-based marketplace model during the first open enrollment period for marketplace coverage but transitioned to its own eligibility and enrollment platform for the 2015 plan year. Conversely, Nevada and Oregon used state functionality at the outset of coverage but switched to a supported state-based model during 2014. New Mexico has used the supported model in both the first and second years of coverage.
* New Mexico’s assessment on carriers varies based on their market share (calculated by the total of their major medical and Medicaid managed care premiums written on and off the exchange) and is pegged to the annual operating expenses of the marketplace.
† Oregon imposes a broad-based assessment on insurers selling both on and off the exchange. However, the exchange authority has retained only the assessment derived from the plans sold through the marketplace.
Source: Authors’ analysis.
Though supported marketplaces must grapple with many of the same budget issues that confront other state-run exchanges—their revenue streams are tied to and affected by fluctuations in enrollment and premium rates, for example—they enjoy an important advantage over their brethren: they do not, at present, have to pay for their eligibility and enrollment platform. In 2014 and 2015, supported marketplaces have been able to use the federal technology without cost, thereby eliminating the pressure of financing one of the most expensive and complicated pieces of the exchange puzzle. This relief will continue for states using the supported model in 2016, as well, making it especially attractive to policymakers in the near term.
In subsequent years, the calculus is expected to change somewhat. Federal officials have signaled they intend to develop a leasing arrangement for the HealthCare.gov platform, starting in 2017.21 Although the exact framework of this arrangement and the cost for the platform’s use will be determined through rulemaking, the charge is expected to be materially lower than the current fee for the federally facilitated marketplace.
DISCUSSION
The supported state-based marketplace model is one implementation path that may be attractive to states from across the exchange spectrum.22 For states that already run a marketplace, the supported model may reduce the operational and, ultimately, financial risk of doing so. Development and maintenance of an eligibility and enrollment platform have been the most expensive and among the most troubled aspects of exchange implementation. By leveraging existing federal technology, marketplaces can operate more leanly and direct their limited resources to other service priorities. For states now using the federally facilitated exchange, the option to keep the familiar interface—and avoid the costs of building or buying a new one—may mitigate the most significant financial obstacle to the creation of a state-based exchange.
Beyond these benefits, the supported model has allowed the states that have used it to retain, through governance authority and plan management functionality, autonomy over critical policy decisions and market oversight. They also have continued to capitalize on local knowledge and connections to reach underserved populations, facilitate enrollment assistance services for consumers, and engage with stakeholders. For policymakers looking to overcome budgeting or scale issues with their state-based marketplaces while maintaining full state oversight—or for states without their own exchange that are looking to reduce the federal footprint—there may be something to like in the examples of these four states.
Ultimately, the appeal of the supported marketplace model may hinge on two factors that stand in some tension: cost and control. Federal regulators are currently developing rules to specify the lease process for the federal technology platform and its cost. It falls to these officials to settle on a stable fee that fairly reflects the support provided by the federal services but that also maintains HealthCare.gov as a cost-effective choice for states looking to transition. Meanwhile, states interested in the model are likely to increase calls for marketplace technology that is more responsive to specific state needs. Relative to other state-based exchanges using their own platforms, supported marketplaces thus far have enjoyed less flexibility to customize the consumer enrollment experience, have been limited in their ability to integrate with Medicaid systems, and continue to work with federal officials to get timely access to data. While some of these barriers may be overcome as experience with the model grows and the lease process is formalized, others, especially around customization, may drive up the price of the platform. It will be up to federal and state policymakers to work together to balance these considerations so the exchanges can meet both their policy goals and their bottom lines.
Notes
1 Pub. L. 111-148, 124 Stat. 782 (2010) §§ 1311, 1321 (codified at 42 U.S.C. §§ 18031, 18041).
2 45 C.F.R. 155.100 et seq.; Center for Consumer Information and Insurance Oversight, Blueprint for Approval of Affordable Health Insurance Marketplaces.
3 See, e.g., S. Dash, C. Monahan and K. Lucia, “Health Policy Brief: Health Insurance Exchanges and State Decisions,” Health Affairs, July 18, 2013.
4 K. Lucia, S. Dash, and C. Monahan, “Evolving Dynamics of Health Insurance Exchange Implementation,” The Commonwealth Fund Blog, June 19, 2013.
5 See, for example, S. Armour, “States Eye Health Exchange Options,” Wall Street Journal, June 26, 2015; M. Sanger-Katz, “Obamacare Ruling May Have Just Killed State-Based Exchanges,” New York Times, June 25, 2015; C. Koller, “Supported State-Based Marketplaces: The Point of Convergence?” Health Affairs Blog, June 11, 2015; and R. Pradhan, “A State Fix If Court Hits Obamacare?” Politico, June 17, 2015.
6 Hawaii Health Connector, “Board of Directors Meeting, June 5, 2015.”
7 One state established an exchange via legislation in 2010 (California), eight did so in 2011 (Colorado, Connecticut, Hawaii, Maryland, Nevada, Oregon, Vermont, and Washington), two did so in 2012 (Massachusetts and Washington, D.C.), and three did so in 2013 (Idaho, Minnesota, and New Mexico). Rhode Island enacted statutory authority for its exchange in 2015, four years after the state’s governor first established the marketplace, through an executive order. Both Idaho and New Mexico submitted exchange blueprint applications and letters declaring their intention to establish an exchange in December 2012.
8 Pub. L. 111-148, 124 Stat. 782 (2010) § 1321(b) (codified at 42 U.S.C. § 18041(b)). For a discussion of state options for obtaining legal authority, see N. Bagley and D. Jones, No Good Options: Picking Up the Pieces After King. v. Burwell (New Haven, Conn.: Yale Law Journal Forum, April 2015).
9 An Idaho official offered the characteristic view, that Idahoans could manage a marketplace better (and cheaper) than the federal government. Likewise, stakeholders voiced preference for in-state governance. For example, an insurer representative from a state that transitioned to the supported model after its technology failed expressed satisfaction that there remained a local exchange staff and governing board that understood the market and were accessible.
10 According to respondents, one important complication in the transition between technology platforms was that the process did not support automatic reenrollment of consumers in their existing plans—functionality that was generally available in the marketplaces that did not transition. There is reason to expect that requiring consumers to return to the marketplace to shop for coverage may be advantageous, at least for some: given changes from one year to the next in the price of health plans and in consumers’ life circumstances, those who return yearly to shop may be able to find more affordable coverage. See, for example, S. Ahn, J. Hoadley, and S. Corlette, Six State Experiences with Marketplace Renewals: A Look Back and a Glimpse Forward (Washington, D.C.: Robert Wood Johnson, July 2015). At the same time, as respondents suggested, the absence of the option for auto-enrollment made coverage retention for 2015 a significant challenge.
11 Idaho’s enrollment for the first open enrollment period (76,061) was about 34 percent higher than projected by the Urban Institute (57,000) and more than double the expectations of analysts at Avalere (35,000). L. Blumberg, J. Holahan, G. M. Kenney et al., Measuring Marketplace Enrollment Relative to Enrollment Projections: Update (Washington, D.C.: Urban Institute, May 2014); C. Pearson, “Avalere Analysis: Exchange Enrollment Outpaces Expectations in 22 States,” Avalere, May 6, 2014.
12 For a discussion of Kentucky’s experience, see T. Riley and A. Gauthier, “State Exchanges Breaking New Ground,” National Academy for State Health Policy, State Health Policy Blog, April 14, 2015.
13 The supported state-based marketplaces sometimes collaborated with other state agencies to perform these tasks. For example, the New Mexico and Nevada marketplaces worked with their respective departments of insurance to certify qualifying enrollment assisters and to monitor their compliance with state standards.
14 Materials from one state’s exchange governing board put this point succinctly: “We know New Mexico.” New Mexico Health Insurance Exchange Board, “New Mexico Health Insurance Exchange Board Meeting Presentation, March 31, 2015.”
15 Notably, stakeholders reported ups and downs with state-run call centers, as well, suggesting the job of providing telephone support for a complicated transaction like the purchase of insurance may be difficult, no matter who is in charge.
16 Pub. L. 111-148, 124 Stat. 782 (2010) § 1311(d)(4)(A) (codified at codified at 42 U.S.C. §§ 18031(d)(4)(A)).
17 S. Corlette, J. Volk, and K. Lucia, Plan Management: Issues for State, Partnership and Federally Facilitated Health Insurance Exchanges (Washington, D.C.: Georgetown University Health Policy Institute and the National Academy of Social Insurance, May 2012).
18 From 2010 to 2014, the state-based marketplace states received approximately $4.3 billion in exchange establishment grants. Federal funding for the four study states was as follows: Idaho ($105 million); Nevada ($91 million); New Mexico ($123 million); Oregon ($303 million). Kaiser Family Foundation, “Total Health Insurance Exchange Grants,” Jan. 5, 2015.
19 Pub. L. 111–148, 124 Stat. 782 (2010) §§1311(a)(4), 1311(d)(5) (codified at 42 U.S.C. §§ 18031(a)(4), 18031(d)(5)). States still have time, after January 1, 2015, to wind down open projects and may seek limited extensions for certain types of funded work. Center for Medicare and Medicaid Services, “FAQ on the Use of 1311 Funds and No Cost Extensions,” March 14, 2014.
20 S. Miskell, J. Giovannelli, K. Lucia et al., “State-Based Marketplaces Look for Financing Stability in Shifting Landscape,” The Commonwealth Fund Blog, May 14, 2015.
21 Silver State Health Insurance Exchange, “Exchange Sustainability Considerations,” June 11, 2015; and New Mexico Health Insurance Exchange Board, “New Mexico Health Insurance Exchange Board Meeting Presentation, March 31, 2015.”
22 A supported marketplace is not the only option for states looking to transition. Private entities, including those with experience building portions of the technology infrastructure used by several state-run marketplaces, have asserted they can provide a fully functional exchange system “out of the box” and in a short time frame. Though these claims have not been tested and the degree to which a private solution as it exists now would satisfy federal requirements is unclear, the presence of private innovation in exchange development seems to bode well for states that would prefer an alternative to HeathCare.gov over the long-term.
Multistate “regional” exchanges are, in theory, still another choice, one expressly blessed by the health law. Pub. L. 111–148, 124 Stat. 782 (2010) §1311(f)(1) (codified at 42 U.S.C. § 18031(f)(1)). Given the amount and complexity of cross-state coordination necessary to build and maintain such an entity, however, the option has won relatively little attention from state policymakers.
In a similar but more modest vein, states may share services or systems with another state while maintaining each marketplace as a separate entity. For example, after its own technology proved unreliable, Maryland’s state-based marketplace adopted the Connecticut exchange’s technology platform beginning in 2015. Similarly, Arkansas, a current partnership state that is planning to transition to a state-based marketplace—for small group coverage, in 2016, and for individual insurance, in 2017—is seeking to use another state’s enrollment platform. See R. Pradhan, “As States Consider Joining HealthCare.gov, Arkansas Plans Its Exit,” Politico, July 6, 2015.



