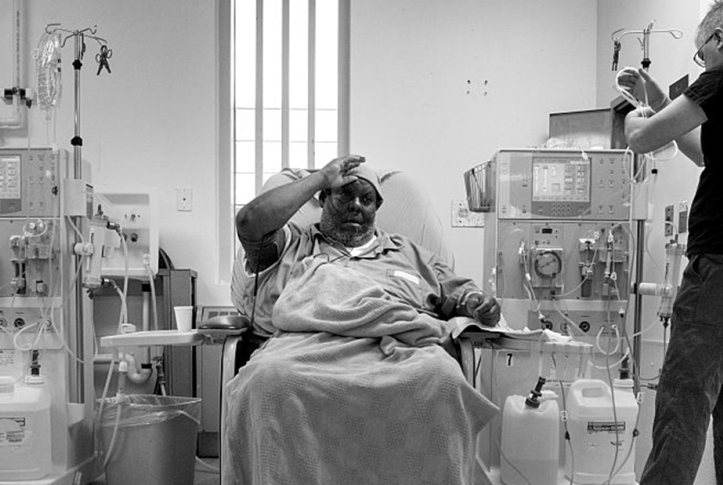
Image caption: Jesse Owens, 52, of New Orleans, Louisiana, is helped by John Thompson, a patient care technician, during a dialysis treatment at Devens Federal Prison in Devens, Massachusetts. Owens receives treatment for his chronic condition three times a week. Photo: Nikki Kahn/The Washington Post via Getty Images
Abstract
- Issue: Individuals who are incarcerated or otherwise involved with the criminal justice system (justice-involved people) face significant health challenges, including high rates of COVID-19.
- Goal: To describe the health needs of justice-involved populations, explain how Medicaid meets those needs, and identify policy changes that could strengthen Medicaid’s role as a tool to improve health outcomes in this population.
- Key Findings: State and local governments are developing new Medicaid approaches to meet the health needs of justice-involved people, particularly as they are leaving incarceration. However, siloes between correctional and community health care providers disrupt care coordination and create gaps in treatment and health services that can be life-threatening. Medicaid policy contributes to these siloes because Medicaid cannot cover services provided to incarcerated people. New policies are being considered to allow Medicaid coverage of some services provided during incarceration to improve coordination, access, and health outcomes.
- Conclusions: The concurrent COVID-19, substance abuse, and mental health crises, as well as growing awareness of racial inequities, are prompting state and federal interest in examining the role of public programs, such as Medicaid, in meeting the needs of the justice-involved population.
Introduction
Several factors are driving efforts to strengthen health care for people who spend time in jails and prisons or are otherwise involved with the criminal justice system. These include the impact of COVID-19 behind bars, the need to address the country’s mental health and substance use crises, and interest in helping people successfully rejoin their families and communities after they are released from prison or jail.
In general, justice-involved individuals have extremely complex health care needs. They experience chronic and infectious diseases, including COVID-19, as well as serious mental illness and substance use disorders at higher rates relative to the general population. Improving health services for justice-involved people can improve the health of populations and communities, keep state and local health care spending down, and advance public safety goals like successful reentry and reduced recidivism. Many individuals currently in the criminal justice system are eligible for Medicaid, especially in states that have taken up the Affordable Care Act’s expansion of eligibility for low-income adults. Medicaid plays a central role in supporting these individuals. Because people who are incarcerated are disproportionately poor and of color, strengthening health care approaches for the justice-involved can advance the goals of health and racial equity.
This issue brief describes the health care needs of people involved in the justice system, how Medicaid’s role in providing coverage for this population has evolved to address those needs, and new policy changes that states and the federal government are advancing.
Overview of the Justice-Involved Population
The United States has the highest incarceration rate of any nation. Jails and prisons function differently within the criminal justice system, although they are often talked about together. On any given day in 2020, about 2.3 million individuals are held in prisons and jails in the U.S.1 Just over 600,000 people enter prison annually. In December 2018, almost 1.5 million individuals were in state or federal prisons.2 Despite how large these numbers are, they pale in comparison to the jail population. There are 10.6 million admissions to jail each year.3 In 2018, the weekly jail inmate turnover rate was 55 percent, and the average jail stay was 25 days.4 The U.S. Department of Justice (DOJ) estimates that the annual cost of corrections to U.S. taxpayers is just over $80 billion, although many experts believe that to be an underestimate.5
Incarceration and the Criminal Justice System: A Quick Overview
In most states, jails and their health care services are the responsibility of counties under the oversight of an independently elected sheriff. There are 3,000 U.S. counties, and most of the individuals held in their jails are detained pretrial, or serving a sentence of less than a year. Prisons, on the other hand, hold individuals sentenced for more than a year and are run by states or the federal government. Prisons generally fall under the jurisdiction and financial responsibility of a state-appointed director of corrections or the federal Bureau of Prisons. The reach of the criminal justice system extends beyond jails and prisons; millions more people are under probation, parole, pretrial supervision, and specialty court supervision, as well as under other local alternatives to incarceration.
Jails and prisons are responsible for providing health care services to people when they are incarcerated. Many facilities contract with vendors to provide services under the oversight of state correctional administrators and local officials, who generally determine the level of services made available. Health care spending, services, and staffing vary from institution to institution and depend on what is available in the community.6
The incarcerated population is disproportionately poor and made up of people of color. According to the Prison Policy Initiative, incarcerated prisoners had a median annual income of $19,185 prior to their incarceration, 41 percent less than what comparable nonincarcerated people earned (Exhibit 1).7
In addition, people of color are more likely to be incarcerated than whites. In 2018 approximately 431 per 100,000 U.S. residents were in prison (state or federal) (Exhibit 2). But the imprisonment rate for Black residents (1,134 per 100,000) was much higher than the rate for white residents (218 per 100,000). The imprisonment rate for Hispanic residents was also high (549 per 100,000).8 Similar racial disparities exist in jails (Exhibit 2).9 Disparities also exist across gender and other racial and ethnic groups.
COVID-19’S Impact
COVID-19 is taking a heavy toll on people who live or work in the nation’s prisons and jails and on the communities that are overrepresented in the justice system. As of October 2020, there were a reported 146,472 cases of COVID-19 among incarcerated people and 30,178 cases among correctional staff, although inconsistent state and local reporting means the actual case rate is not known.10 In late April, over 70 percent of tested inmates in federal prisons had COVID-19.11 The high rates of comorbidities among people who are incarcerated place them at risk of dangerous COVID complications. In some state prisons, three out of every four inmates have tested positive.12 This spring, the rate of infection for prisoners was 5.5 times higher than that of the general public, and the COVID-19 death rate was three times higher.13 Because people of color, and particularly Black people, are much more likely to be incarcerated than white people, high COVID-19 rates in correctional settings contribute to racial disparities in COVID’s impact.
Correctional facilities face serious challenges in mitigating virus transmission. Close, shared spaces make it difficult to control the spread of COVID-19 behind bars.14 Resources for treatment available within correctional facilities vary, and many are not equipped to treat acute COVID complications or coordinate with community providers as people enter the correctional setting or are released. Because correctional staff return home to their communities each day, and many jail stays are brief, these facilities are a leading source of community transmission in the U.S.15 Researchers estimated that one in six cases of COVID-19 in Illinois could be traced back to the Cook County jail.16
People Involved in the Justice System Have Complex Health Issues
COVID-19 is having a severe impact on many people who are incarcerated. Incarcerated individuals — including people in prisons and jails — are much more likely to suffer from chronic health conditions and infectious diseases (such as hypertension, tuberculosis, diabetes, and hepatitis), which elevate their risk of serious COVID complications, than nonincarcerated individuals (Exhibit 3).17
Justice-involved people also experience high rates of substance use disorders and have more severe mental health needs. In 2009, an estimated 58 percent of state prisoners and 63 percent of sentenced jail inmates met the criteria for drug dependence or abuse, in comparison to just 5 percent of the total general population over age 18 (Exhibit 4).18 In general, prison and jail inmates are three-to-five times more likely to meet the threshold for serious psychological distress than adults in the nonincarcerated U.S. population.19
When people leave prison or jail, they are also more likely to use hospital services and experience adverse health events, including death. In the first two weeks post reentry, the mortality rate for individuals leaving prison is 12 times higher than that of the general public.20
Medicaid’s Role for Justice-Involved Individuals
Because many people who are incarcerated are poor, most of them are eligible for Medicaid. States that have expanded Medicaid to low-income adults play a particularly strong role in providing coverage to justice-involved people. Over the past several years, states and providers have strengthened Medicaid coverage and services for people who are involved in the justice system.
However, Medicaid’s role for people who are incarcerated is limited. By law, Medicaid cannot cover services provided to people while they are in jail or prison, with the exception of inpatient hospital stays provided outside of carceral settings. This prohibition, known as the inmate exclusion policy, was established in 1965, when Congress first authorized Medicaid, to prevent cost-shifting from state and local governments to the federal government. As a result, states and local governments are solely responsible for financing health care delivered to incarcerated people who qualified for Medicaid before they were in prison or jail. The services provided to people who are incarcerated reflect the variability of state and local resources and practices; consistent standards do not apply and there is substantial variation in the amounts spent, the type and quantity of services provided, and the quality of services.
The inmate exclusion policy thus creates discontinuities in care for Medicaid beneficiaries as they move from Medicaid coverage preincarceration to the correctional system, which is largely locally driven, and back to the Medicaid system upon release. Insufficient coordination between corrections providers and community providers frequently interrupt the services, medications, and treatments that individuals were receiving prior to detention. It also creates disruptions at release that make it difficult for people to obtain services that can support successful reentry and reduce recidivism.
States and local jurisdictions have begun developing approaches to better meet the health needs of Medicaid beneficiaries who are incarcerated. Historically, many states responded to the inmate exclusion policy by terminating individuals’ Medicaid eligibility when they became incarcerated, which means that people leave incarceration without Medicaid eligibility and must reapply. Increasingly, however, states are recognizing the value of maintaining continuous Medicaid coverage for this population. Instead of terminating coverage, many states are suspending Medicaid benefits for incarcerated people. As of 2019, 43 states had implemented suspension policies for some prisons, while 42 had done so for some jails.21 Leveraging data exchange between information systems can help ensure suspensions are coordinated between state Medicaid agencies and prisons and jails.
States also are developing approaches to strengthen services and coordination for people during and after incarceration. Strategies include:
- conducting in-reach by encouraging community providers and health plans to begin communication and coordination before release
- deploying peer support specialists who have lived experience with incarceration and/or behavioral health issues
- training primary care providers to be culturally competent and understand the unique and complex health needs of justice-involved individuals
- addressing housing instability and other social determinants of health.22
Data Exchange in Arizona
Arizona operates a data-exchange pilot program. Through this program, participating jails correspond daily with the state Medicaid agency to provide information on everyone who was either booked or released that day. Arizona’s system uses data transfer to automate the suspension of Medicaid eligibility for incarcerated individuals and reinstate coverage when they are released. Arizona also uses this information to provide notices to managed care organizations and community providers about who is enrolled.
As of 2017, this program operated in most of the state’s counties and covered more than 90 percent of the state’s jail population.23
These approaches are much more common in Medicaid expansion states, where the share of the low-income population that Medicaid covers is substantially larger and is supported with a favorable 90 percent federal matching rate, making systems and programmatic investments for this population more viable.24
Another strategy being used by some states is the establishment of “health homes,” created by the Affordable Care Act as an option for Medicaid beneficiaries with chronic conditions. Beneficiaries are eligible for health homes if they have two or more chronic conditions (including mental health disorders, substance use disorders, asthma, diabetes, heart disease, and obesity), have one chronic condition and are at risk for a second, or have one serious and persistent mental health condition. The model is designed to coordinate and integrate all primary care, hospital care, mental health services, substance use disorder services, and ongoing social services and supports.
Health Homes in New York and Rhode Island
Both New York and Rhode Island have implemented variations of the health home model, an optional state plan benefit designed specifically to serve Medicaid beneficiaries with chronic health conditions on their reentry into the community.
As of 2017, New York had developed seven criminal justice health home pilots, while Rhode Island had three health homes, each focused on a different group of individuals based on their chronic disease profiles. One of these three — the opioid treatment program — was specifically designed to assist the reentry population.25
The authorization of Medicaid health homes has encouraged collaboration across the criminal justice and community health boundary in some states, a development that should improve the care provided to the justice-involved population and result in better health outcomes.
Recent Proposals to Change Medicaid’s Inmate Exclusion Policy
Policy proposals are emerging to allow Medicaid to cover services for people who are incarcerated.
Federal Policy Changes
In May, the U.S. House of Representatives included the Medicaid Reentry Act in the COVID relief package it passed (the HEROES Act, which awaits action by the Senate).26 The Medicaid Reentry Act would allow Medicaid to cover services for beneficiaries who are incarcerated during the 30 days preceding their release from prison or jail.27 This would close part of the gap in care that beneficiaries experience when they are incarcerated and could improve the health of those involved in the justice system.
The reform also would facilitate access to pre- and postrelease services for individuals with COVID-19 and other complex health conditions, including substance use disorders and mental health conditions. And it could address the concerns of local government and public safety officials who argue that the inmate exclusion policy leads to worse health outcomes, creates service gaps at reentry that drive recidivism, and poses a financial and administrative burden for local governments.28 Other recent legislative proposals would repeal the inmate exclusion policy altogether.29
The Medicaid Reentry Act follows the passage of another piece of legislation focused on similar policy goals, the SUPPORT (Substance Use Disorder Prevention that Promotes Opioid Treatment for Patients and Communities) Act. The law requires the Centers for Medicare and Medicaid Services (CMS) to issue policy guidance to states to help them improve health care transitions for incarcerated people at reentry, including providing services in the 30-day period prior to release, through a Medicaid Section 1115 demonstration waiver. This guidance has not yet been issued.30
State Policy Changes
At the same time, some states are proposing to provide Medicaid services to people when they are incarcerated. States are seeking federal authority to waive the inmate exclusion policy.31 Specifically:
- As part of broader COVID-19 response 1115 waiver proposals, California and Illinois have asked for authority for Medicaid coverage for COVID-19 testing and treatment for Medicaid beneficiaries who are incarcerated.32
- Utah recently submitted an 1115 waiver proposal to CMS seeking authority to cover services for people who are preparing to leave incarceration and return to their communities. Utah proposes to provide comprehensive services to people with complex health needs in the 30 days prior to release from prison or jail.33 CMS has not yet acted on this proposal.
- Last year, the District of Columbia proposed to provide transition planning services for people leaving incarceration, among other settings.34 In 2017, Illinois proposed to provide behavioral health services to Medicaid beneficiaries leaving Cook County jail. The federal government did not approve these proposals to cover services for people leaving incarceration.
In permitting Medicaid coverage of these services, all these proposals, whether undertaken statutorily or administratively, would recalibrate the historical coverage and financing responsibilities assigned to local, state, and federal governments for health care for people who are incarcerated. These proposals also create the potential for greater coordination of care and services by reducing the policy barrier that separates the correctional health system from the community health system. Implementing these proposals would require overcoming service delivery differences between correctional and community health, including differing systems of accreditation, quality, and health care decision-making. It also would necessitate developing relationships between correctional and community providers, as well as an enhanced focus on ensuring that people involved in the justice system have access to community services.
Conclusion
Medicaid plays a key role in providing coverage for low-income people who are involved in the criminal justice system. The program is propelling health care advances that have the potential to address disproportionately high rates of COVID-19, substance use disorders, and mental health issues among this population, as well as to facilitate successful reentry. State and local governments are increasingly strengthening enrollment processes and care delivery for justice-involved people, particularly at reentry.
A number of issues are bringing Medicaid’s inmate exclusion policy into sharper focus, including the need for expanded, continuous access to substance use disorder and mental health treatment, the COVID-19 crisis in prisons and jails, and a desire to address serious racial inequities in health and criminal justice. As a result, there is growing state and congressional interest in broadening Medicaid’s role for people who experience incarceration.
Glossary
Inmate exclusion policy
Section 1905(a) of the Social Security Act prohibits federal Medicaid funds, known as federal financial participation, from being used to pay for services for inmates of public institutions, even if they are otherwise eligible for Medicaid. This is known as the Medicaid inmate exclusion policy. The Code of Federal Regulations defines an “inmate of a public institution” as an individual who is living in a public institution, except if he or she is in an institution for “a temporary period pending other arrangements appropriate to his needs.” Public institutions are defined as those that are “the responsibility of a governmental unit or over which a governmental unit exercises administrative control,” including jails and prisons (42 CFR Section 435.1010). Despite the inmate exclusion, Medicaid can reimburse a provider for services delivered to an inmate sent to a noncorrectional medical facility if the inmate is an inpatient in that facility for greater than 24 hours. The Affordable Care Act did not make any changes to these long-standing federal Medicaid policies.
Jail vs. Prison
Jails are typically county or city institutions that house individuals awaiting local trial (detainees) and individuals convicted of misdemeanors (inmates) who are serving short sentences, generally less than one year. Prisons, on the other hand, are state or federal facilities that usually incarcerate convicted felons (frequently referred to as inmates or prisoners) serving sentences longer than one year. At any time, a jail inmate may be released on bail or charges could be dropped. By contrast, prison inmates are usually stable on admission and have relatively fixed release dates that depend on their sentences.
Justice-involved
Refers to any individual — or the population of individuals — that come into direct contact with the U.S. criminal justice system. This includes those in jails and prisons, but also those under probation, parole, pretrial supervision, specialty court supervision, and other alternatives to incarceration. The term encourages a more holistic, and realistic, recognition of our criminal justice system.
Pretrial
Refers to the processes and events that occur at the front end of the criminal justice system — from initial contact with a law enforcement officer through final adjudication of charges — as well as to the period during which those processes and events occur. In general, defendants are either held in jail or released into the community during the pretrial period.
Pretrial supervision
Strategy often used to ensure that an individual who has been accused of committing a crime will appear for a court hearing without having to post a bond, thus avoiding pretrial incarceration. This supervision can take many forms, including, but not limited to, check-ins with a designated case manager, court date reminders, and drug and alcohol testing.
Probation vs. Parole
Two forms of community supervision by the criminal justice system. An offender may be sentenced to probation in lieu of serving jail or prison time. Probation sentences usually involve strict guidelines to which offenders must adhere; violating conditions of probation can result in incarceration. Parole is a conditional release from prison. Parolees are individuals who have already served time in prison and are granted an early release, dependent on certain conditions that must be met for the offender to avoid reincarceration.
Recidivism
Generally speaking, the phenomenon in which an individual who was once detained or incarcerated ends up back in a correctional facility. There are various ways that this can happen. For instance, a previously incarcerated individual could commit another crime or violate the terms of his or her probation or parole. Thus, there are many ways to define recidivism.
Reentry
The transition period between custody in jail or prison and the community. Although individuals making this transition are sometimes given assistance through discharge planning, the resources available are typically very limited.
Serious psychological distress
Serious psychological distress is determined through questions based on the Kessler 6 (K6), a six-question tool developed to screen for serious mental illness among adults age 18 and older in the general U.S. population. People taking the K6 are asked how often in the past 30 days they have felt:
- nervous
- hopeless
- restless or fidgety
- so depressed that nothing could cheer them up
- like everything was an effort
- worthless.