Health care purchasers, accrediting organizations, and consumer advocates are among the stakeholders currently using quality improvement (QI) methods to improve patient care. But there is still one key group for whom the pursuit of QI has not become routine: physicians.
To date, QI has not permeated the culture of professional medicine, say the authors of "Measure, Learn, and Improve: Physicians' Involvement in Quality Improvement" (Health Affairs, May/June 2005). Drawing upon data from the Commonwealth Fund National Survey of Physicians and Quality of Care, Anne-Marie J. Audet, M.D., and her colleagues found that only one-third of doctors have been involved in any redesign efforts aimed at improving performance. Just a third, moreover, have access to any data about the quality of their own clinical performance, while seven of 10 physicians do not feel the public should have access to quality-of-care data. The survey also revealed surprisingly low use of electronic medical records (EMRs): only about a quarter (27%) of doctors reported using an EMR routinely or occasionally.
Audet, an assistant vice president at The Commonwealth Fund, led the research team, which also included Fund senior analyst Michelle M. Doty, Ph.D., program associate Jamil Shamasdin, and executive vice president for programs Stephen C. Schoenbaum, M.D.
No Data, No QI
A large part of the lag in QI among physicians seems to be that they lack essential data about their own practices. In the survey, less than half of doctors reported they could easily identify patients by age group (49%) or diagnosis (44%). And most said it would be difficult or impossible to generate data about patients with abnormal lab results (83%) or to identify patients taking high-risk medications that might require follow-up care (84%).
In addition to asking about patient data, the survey queried doctors about access to quality-of-care data, appropriate use of health care services, and clinical outcomes. Only 33 percent of physicians surveyed said they receive any data about the quality of care they provide (patient surveys were the data source doctors most commonly cited). Doctors also have problems getting performance information when they refer patients for specialized care: nearly two-thirds (64%) say they rarely or never have access to such information, while one-third say they have trouble getting referral information in a timely manner.
Reluctance to Share
In addition to not using data themselves, physicians are generally reluctant to share performance-level data with others, the survey found. While nearly three-quarters of physicians agreed that clinical performance data should be shared with the medical leadership of their health systems, they were not as likely to share information with patients or the general public. Fifty-five percent of doctors felt such data should be shared with patients, and less than a third (29%) felt the general public should have access to quality-of-care data.
Practice Size Matters
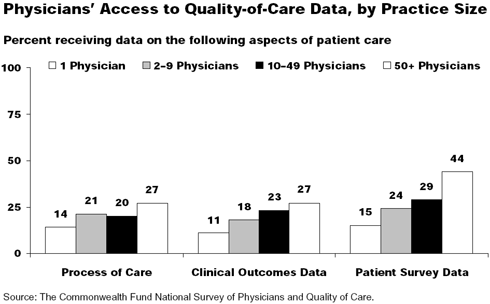
Practice size figured prominently throughout the survey. Physicians in large practices (i.e., 50 or more doctors) were more likely to generate practice-level data and to receive quality-of-care data. They were also more likely to engage in redesign efforts. Why are these providers more up to speed? Collecting and analyzing data, and then using the information to implement change requires resources, say the researchers. Physicians in large group practices, as well as salaried physicians, "might have more financial flexibility and access to capital and thus be in a better position to implement both the measurement and the improvement parts of the QI cycle." The authors add that organizational culture and management may also play a role.
Speeding Adoption of QI
According to the Commonwealth Fund survey, only 34 percent of physicians are involved in efforts to redesign systems to improve care. While adoption of QI methods seems to be highest among physicians in larger group practices, policies and proposals must consider the fact that most U.S. physicians provide care in solo or small-group practice (i.e., two to nine physicians) settings. One potential strategy is to create payment policies that reward quality, or even involvement in QI work. For most of the surveyed physicians, productivity was the major factor determining compensation; clinical quality was cited as a major factor by fewer than 10 percent.
Furthermore, most existing quality measures are aimed at the hospital or health plan level. Organizations and agencies such as the National Committee for Quality Assurance, Centers for Medicare and Medicaid Services, and the Ambulatory Care Quality Alliance (whose members include the American Academy of Family Physicians, American College of Physicians, America's Health Insurance Plans, and Agency for Healthcare Research and Quality) are currently working to develop measures that will target physicians' offices. Educational initiatives, like improved medical school curricula and expanded residency training, as well as recertification programs, may also be necessary to speed up QI adoption, the researchers say.
Facts and Figures
- About one-fifth of physicians in solo practice receive quality-of-care data, compared with nearly half of those in groups of 50 or more.
- Commercial insurance companies and health plans were the most common sources of quality-of-care data: 25 percent of physicians reported receiving data from such groups.
- Primary care physicians were engaged in redesign efforts more often than specialists were (42% vs. 31%).
- A higher proportion of physicians who had been recertified in their specialty reported being involved in practice redesign efforts compared with those who had not been recertified (37% vs. 31%).