The 2005 Commonwealth International Survey on Sicker Adults was released Nov. 3 at the Fund's 2005 International Symposium on Health Care Policy in Washington, D.C. Click on the image at left to see a slide show of slides from the event. Or click here for a multimedia presentation that features slides, audio, video and a transcript of speakers' comments during the survey release and question-and-answer period that followed. Note that this presentation will open in a separate window and that the video might take a few seconds to load. Dial-up and DSL users may choose to watch this version of the presentation, which does not include the video.
In the Literature
A new international survey supported by The Commonwealth Fund finds that one-third of U.S. patients with health problems reported experiencing medical mistakes, medication errors, or inaccurate or delayed lab results—the highest rate of any of the six nations surveyed. While sicker patients in all countries reported safety risks, poor care coordination, and inadequate chronic care treatment, with no country deemed best or worst overall, the United States stood out for high error rates, inefficient coordination of care, and high out-of-pocket costs resulting in forgone care.
Results and analysis from the survey—the eighth in a series of Fund-supported cross-national surveys—are discussed in Taking the Pulse of Health Care Systems: Experiences of Patients with Health Problems in Six Countries (Health Affairs Web Exclusive, November 3, 2005).
For the first time, the survey includes Germany, in addition to Australia, Canada, New Zealand, the United Kingdom, and the United States. The 2005 study examines issues of safety, health care coordination, chronic disease care, and access to care. Adults who had recently been hospitalized, had surgery, or had health problems were interviewed by telephone between March and June 2005.
Medical, Medication, and Lab Errors
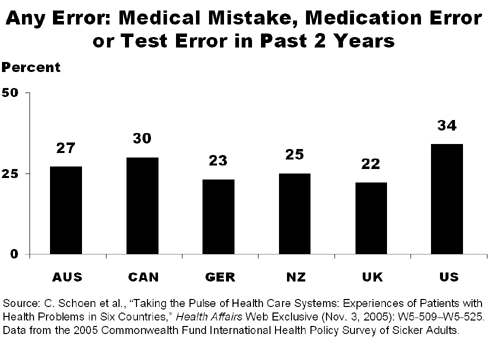
One-third (34%) of U.S. respondents reported at least one of four types of errors: they believed they experienced a medical mistake in treatment or care, were given the wrong medication or dose, were given incorrect test results, or experienced delays in receiving abnormal test results. Three of 10 (30%) Canadian respondents reported at least one of these errors, as did one-fifth or more of patients in Australia (27%), New Zealand (25%), Germany (23%), and the U.K. (22%). While patient safety efforts have focused chiefly on hospital settings, most patients (60% or more) said these errors occurred outside the hospital—a signal that safety initiatives should also focus on ambulatory care, said Cathy Schoen, the study's lead author and a senior vice president at The Commonwealth Fund.
Patients receiving complex care may be at even higher risk of medical errors: the incidence of patient-reported errors rose sharply with the number of physicians seen. Despite studies showing patients value discussion about mistakes or errors, most patients (61% to 83%) in each country said the health care providers involved did not tell them about the mistakes.
Communication and Care Coordination
Communication issues also adversely affect patients' experiences during hospital stays. At least one-fifth of patients (19% to 26%) in the six countries reported communication gaps between themselves and hospital staff, and one-sixth said they would have liked greater involvement in decisions made about their care.
Good transitional care—helping patients transfer from hospital to home—also relies on clear communication and coordination. In all six countries, however, at least one-third of patients said they did not receive instructions about symptoms to watch for, did not know whom to contact with questions, or were left without follow-up care arrangements. German patients had the highest rate of coordination deficiencies when discharged from the hospital, with 60 percent reporting failures to coordinate care. According to the authors, poor transitional care can result in complications and increase the likelihood of hospital readmission, raising concerns about costs as well as quality.
While the U.S. performed better than most countries on the hospital transition measure, it had the highest rate of patients reporting coordination problems during doctor visits. One-third (33%) of U.S. respondents said that either test results or records were not available at the time of appointments or that doctors duplicated tests. These delays and duplications are a clear sign of inefficient care, the authors said, and waste both physicians' and patients' time and resources. Rates of care coordination problems in the other survey countries were significantly lower, ranging from one-fifth to one-quarter of patients reporting such problems.
Access Issues, Financial Burdens, and Forgone Care
As was found in past surveys, the U.S. is an outlier in terms of financial burdens placed on patients. One–half of adults with health problems in the U.S. said they did not see a doctor when sick, did not get recommended treatment, or did not fill a prescription because of cost. Despite these high rates of forgone care, one-third of U.S. patients spent more than $1,000 out-of-pocket in the past year. In contrast, just 13 percent of U.K. adults reported not getting needed care because of costs, and two-thirds had no out-of-pocket costs.
There were wide and significant variations in access and waiting times on multiple dimensions across the six countries. Respondents in Canada and the U.S. were significantly less likely than those in other countries to report same-day access and more likely to wait six days or longer for an appointment. At the same time, majorities of patients in New Zealand (58%) and Germany (56%), and nearly half in Australia (49%) and the U.K. (45%), were able to get same-day appointments. Waiting times for elective surgery or specialists were shortest in Germany and the U.S., with the majority of patients in both countries reporting rapid access.
Overall Performance
The authors say that no country emerges as a clear winner or loser. All survey countries experience high rates of safety risks, failure to coordinate care during transitions, inadequate communication, and a lack of support for chronically ill patients. These areas of shared concern, they conclude, will likely require policy innovations that transcend current payment and delivery systems.
Facts and Figures:
- More than one of four patients in each country (28% to 32%) said risks were not completely explained during their hospital stay.
- In all countries, sizable majorities of patients said physicians had not always reviewed all their medications during the past year, and one-third or more reported infrequent reviews.
- Across countries, one-sixth to one-fourth of patients said physicians only sometimes, rarely, or never make goals of care and treatment clear or give them clear instructions.
- Relative to the U.S. and Canada, the four countries reporting comparatively rapid access to physicians—Australia, Germany, New Zealand, and the U.K.—also had significantly lower rates of emergency room use.