Synopsis
A study of hospitals in U.S. metropolitan areas found those affiliated with accountable care organizations (ACOs) were able to more quickly reduce the rate at which patients discharged to skilled nursing facilities needed to be readmitted within 30 days. Careful attention should be paid to the discharge planning methods and information exchange practices used by ACO-affiliated hospitals, which could contribute to the difference in reduced readmission rates.
The Issue
"The reductions suggest that ACO-affiliated hospitals are either discharging to the nursing facilities more effectively compared to other hospitals or targeting at-risk patients better, or enhancing information sharing and communication between hospitals and skilled nursing facilities."
About 20 percent of admissions to skilled nursing facilities come from hospitals, and many of the patients cared for in these facilities are elderly. For these individuals, care often is fragmented and poorly coordinated. Part of the mission of ACOs is to improve the coordination of patient care and reduce the need for costly rehospitalization. A new Commonwealth Fund–supported study in Health Affairs examined whether ACO-affiliated hospitals in metropolitan areas are more effective in reducing readmissions from skilled nursing facilities than other hospitals are. Fewer readmissions would generate significant health system savings while improving quality of life for the elderly. The study focused exclusively on noncommercial ACOs participating in Medicare’s Shared Savings Program and Pioneer ACO demonstration, both authorized by the Affordable Care Act.
Key Findings
- Looking at readmissions data across nearly 8,000 diagnoses, the researchers found that, from 2010 to 2013, all hospitals reduced readmissions of those patients discharged to skilled nursing facilities. This suggests that all hospitals had focused on decreasing readmissions, likely motivated by a new Medicare regulation that penalized hospitals with relatively high readmission rates. However, ACO-affiliated hospitals reduced readmissions more quickly than other hospitals.
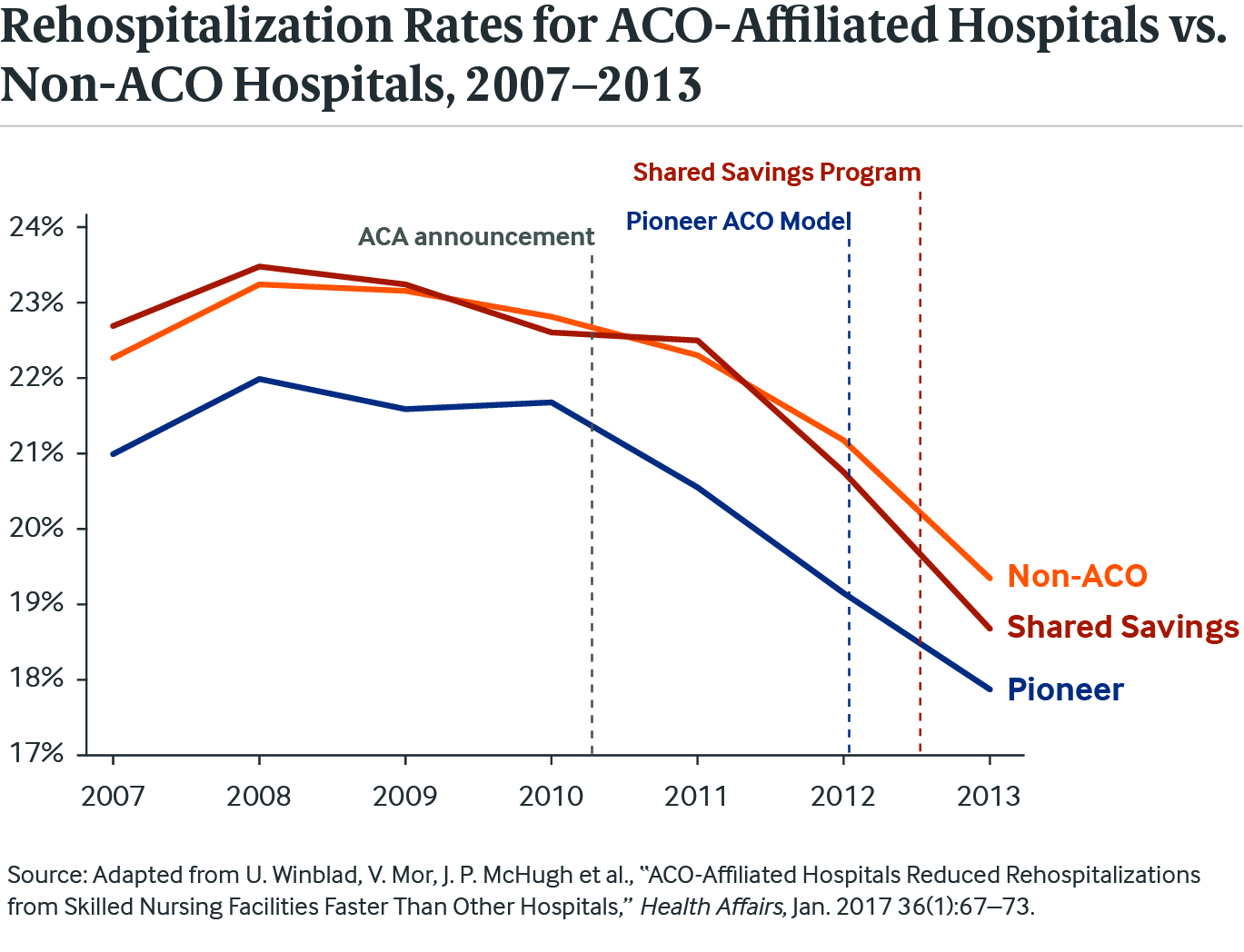
- From 2007 to 2013, Pioneer ACO hospitals reduced their 30-day readmissions by 3.1 percentage points, Medicare Shared Savings hospitals reduced readmissions by 4.0 points, and non-ACO hospitals decreased readmissions by 2.9 points.
- When adjusting the data for clinical and demographic characteristics, the researchers found that from 2007 to 2013 there was a relative reduction in all-cause readmissions of 17.7 percent for Shared Savings hospitals, 14.9 percent for Pioneer ACO hospitals, and 13.1 percent for non-ACO hospitals.
- Pioneer ACO hospitals had lower 30-day readmission rates than both non-ACO and Shared Savings hospitals.
- Most of the difference in readmission rates occurs within the first three days of hospital discharge.
The Big Picture
That ACO-affiliated hospitals were able to reduce readmissions more than other hospitals suggests they had changed their discharge practices or improved their communication with skilled nursing facilities. The authors contend that more information is needed about the specific mechanisms that are most effective. In addition, they recommend ACOs establish more formal governance structures that allow skilled nursing facilities a greater voice in ACO decision-making. This could lead to better health outcomes for patients.
About the Study
The researchers compared readmission rates for Medicare beneficiaries served by ACO-affiliated metropolitan hospitals with those served by non-ACO hospitals in the same geographic area. The analyses were based primarily on Medicare Part A claims and Medicare enrollment files for the years 2007 to 2013. Researchers used Medicare data to identify beneficiaries’ prior nursing home residence.
The Bottom Line
Rehospitalizations generally decreased between 2007 and 2013 for all Medicare patients transferred to nursing homes, but ACO-affiliated hospitals reduced their readmissions more quickly than other hospitals.
