Overview
The fourth Commonwealth Fund Scorecard on State Health System Performance tells a story that is both familiar and new. Echoing the past three State Scorecards, the 2015 edition finds extensive variation among states in people’s ability to access care when they need it, the quality of care they receive, and their likelihood of living a long and healthy life. However, this Scorecard—the first to measure the effects of the Affordable Care Act’s 2014 coverage expansions—also finds broad-based improvements. On most of the 42 indicators, more states improved than worsened.
"On most of the 42 indicators, more states improved than worsened."
By tracking performance measures across states, this Scorecard can help policymakers, health system leaders, and the public identify opportunities and set goals for improvement. The 50 states and the District of Columbia are measured and ranked on 42 indicators grouped into five domains: access and affordability, prevention and treatment, avoidable hospital use and cost, healthy lives, and equity. Individual indicators measure things like rates of children or adults who are uninsured, hospital patients who get information about how to handle their recovery at home, hospital admissions for children with asthma, and breast and colorectal cancer deaths, among many others.
The top-ranked states are Minnesota, Vermont, Hawaii, Massachusetts, Connecticut, New Hampshire, and Rhode Island. These states were also leaders in the 2014 Scorecard.
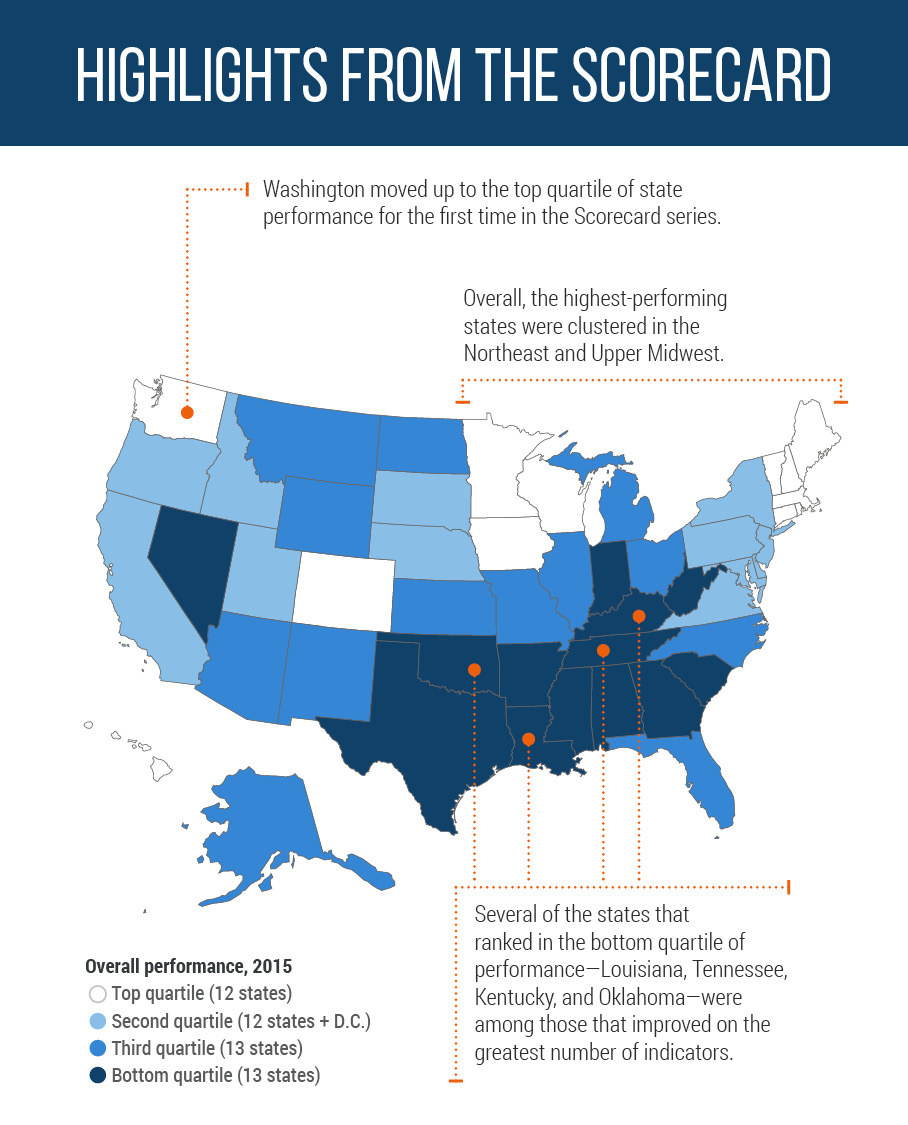
There are wide variations in performance, with up to an eight-fold difference between top- and bottom-ranked states.
- National attention may be encouraging better quality of care in hospitals and home health care settings and to more appropriate medication use in nursing homes and doctor’s offices. However, declining rates of preventive care in several states signal the need for greater attention to prevention.
- Reductions in hospital readmissions accelerated in 2012, when the federal government began financially penalizing hospitals with high rates of readmissions.
- Rates of potentially preventable admissions to the hospital continued to fall in several states. In recent years, health care spending growth moderated for Medicare beneficiaries across states, while premiums for employer-sponsored health plans continued to rise.
- State Scorecard Finds Progress in Reducing Hospital Readmissions
Select a dimension name to open a PDF with highlights from each report area.





ABOUT THE SCORECARDThis 2015 edition of the Scorecard on State Health System Performance is the fourth in an ongoing series. Previous State Scorecards were published in 2007, 2009, and 2014. The 2014 Scorecard assessed changes from 2007 to 2012, which included the Great Recession but stopped short of major coverage expansions under the Affordable Care Act.The 2015 edition measures changes in performance during 2013 and 2014 to assess the effects of the ACA’s 2014 health insurance expansions, as well as early effects of health care delivery and payment reforms like accountable care organizations and financial incentives to reduce hospital readmissions. The effects of the ACA are not yet fully reflected in the 2015 Scorecard results. It may take many years to see the resulting changes.Annual updates in this series will document the trajectory of states’ performance as changes shaped by public policy and the private market continue to unfold.Download the full report for all highlights, as well as a complete description of Scorecard methods and indicators. See Appendices for state-specific rates for each indicator. Also see a companion brief, The Changing Landscape of Health Care Coverage and Access: Comparing States’ Progress in the ACA’s First Year. |