An update to this blog post was published in November 2023, available here.

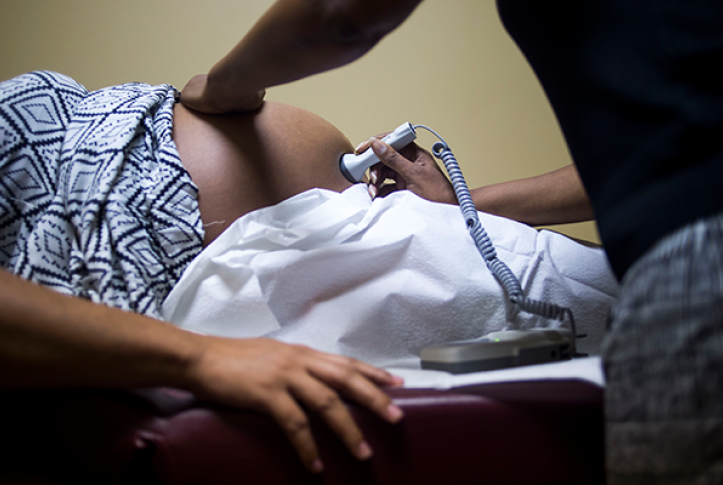
Photo: Zack Wittman/New York Times/Redux
Photo: Zack Wittman/New York Times/Redux

Senior Program Officer, Center for Health Care Strategies

Vice President and Director of Delivery System Reform, Center for Health Care Strategies, Inc.

Senior Vice President, Advancing Health Equity, The Commonwealth Fund

Senior Program Officer, Center for Health Care Strategies

Vice President and Director of Delivery System Reform, Center for Health Care Strategies, Inc.

Senior Vice President, Advancing Health Equity, The Commonwealth Fund
State Medicaid agencies can help improve maternal health outcomes by implementing policies that improve coverage, quality, and equity
A new data resource from the Commonwealth Fund identifies 25 state policies that can improve maternal health outcomes
An update to this blog post was published in November 2023, available here.
Medicaid is the health insurer for 45 percent of births in the United States and 66 percent of all births to Black mothers. Given the disparate rates of maternal mortality and morbidity between Black and indigenous people and white people in the U.S., there is an opportunity for state Medicaid agencies to take the lead in implementing policies that promote better birth outcomes and reduce these drastic racial disparities in maternal health outcomes.
State Medicaid agencies and public health departments can craft policy options that, for example, extend postpartum coverage; enhance benefits to cover home-visiting programs, group prenatal visits, and doulas; or develop value-based payments that reward improved health outcomes and equity. Understanding the state policy landscape can help policymakers, researchers, patient advocates, and health care providers target their efforts.
To aid in these efforts, the Center for Health Care Strategies (CHCS), in partnership with the Institute for Medicaid Innovation and with support from the Commonwealth Fund, created a dataset and interactive maps of state maternal health policies that support high-value care. They identified 25 policies that are organized into three categories: 1) coverage and benefits; 2) care delivery transformation; and 3) data and oversight.
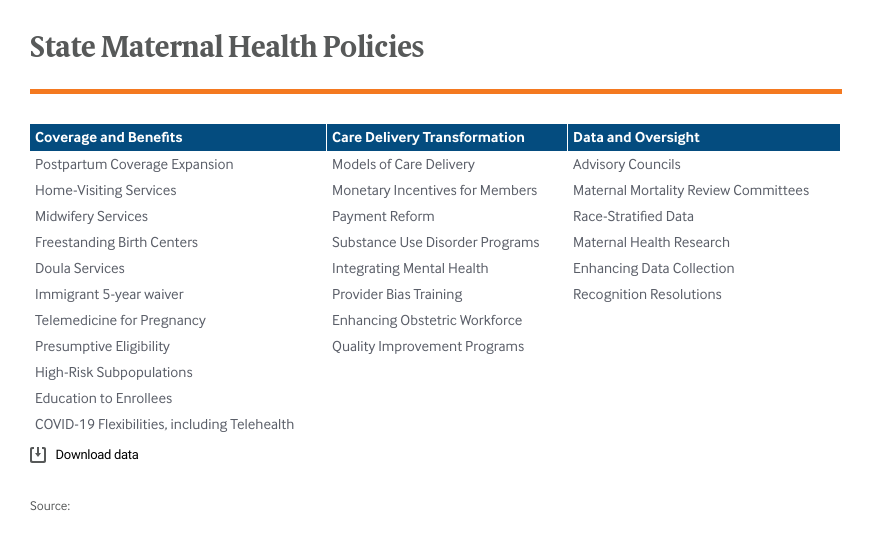
Based on their research, CHCS analyzed maternal health policies to identify national and state trends. Highlights include:
To learn more about how states compare in maternal health policy adoption, explore State Policies to Improve Maternal Health Outcomes.
Publication Details
Date
Citation
Priti Khanal, Tricia McGinnis, and Laurie Zephyrin, "Tracking State Policies to Improve Maternal Health Outcomes," To the Point (blog), Commonwealth Fund, Nov. 19, 2020. https://doi.org/10.26099/bj36-a204
Area of Focus