Drug overdose deaths in the United States spiked during the COVID-19 pandemic; recent estimates from the Centers for Disease Control and Prevention indicate that more than 105,000 lives were lost in 2021. This level of preventable mortality stands in stark contrast to international peer countries and is contributing to an unprecedented decline in U.S. life expectancy.
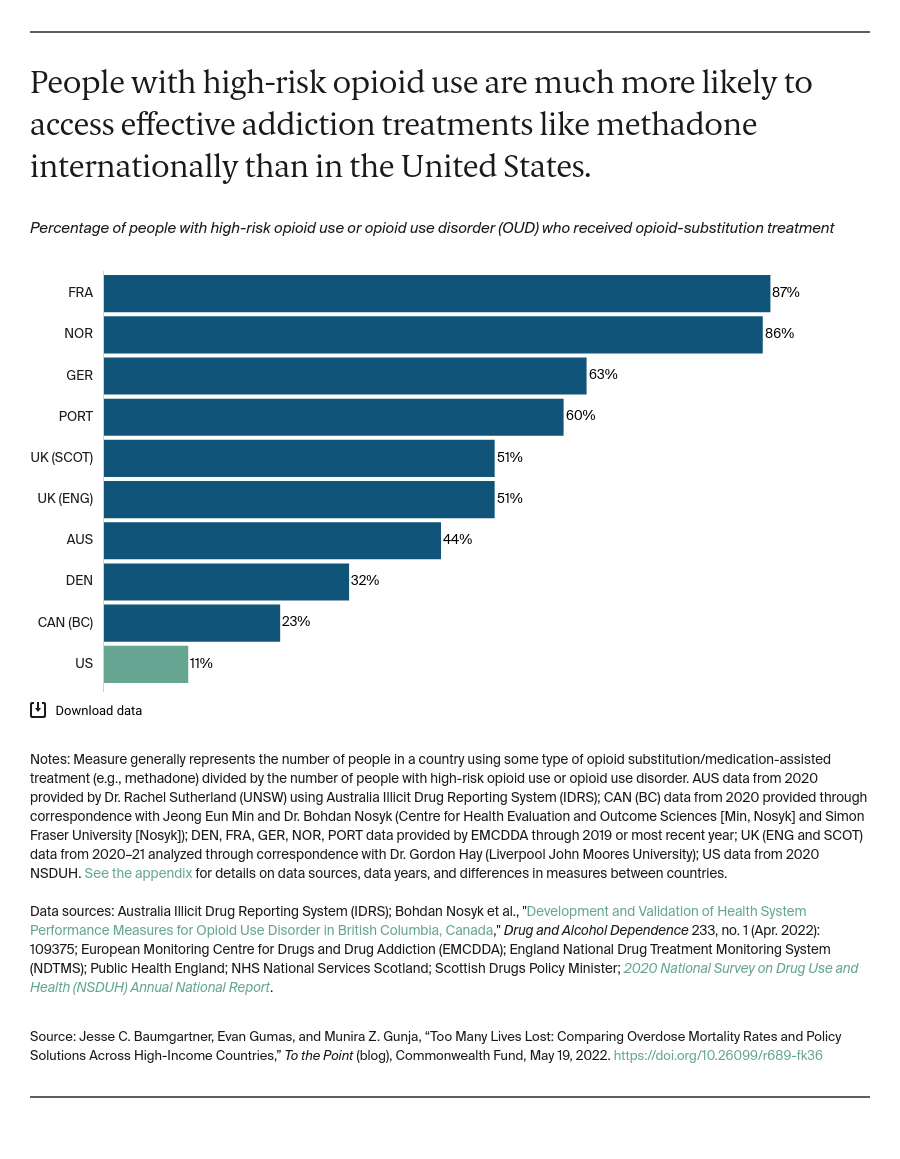
In this post we compare the U.S. to other high-income countries in drug overdose deaths and then highlight differences in behavioral health care, drug policies, and social services, and look at recent U.S. initiatives.
Understanding and leveraging international models can help the U.S. reduce overdose deaths and enact more compassionate, evidence-based policy around drug use.
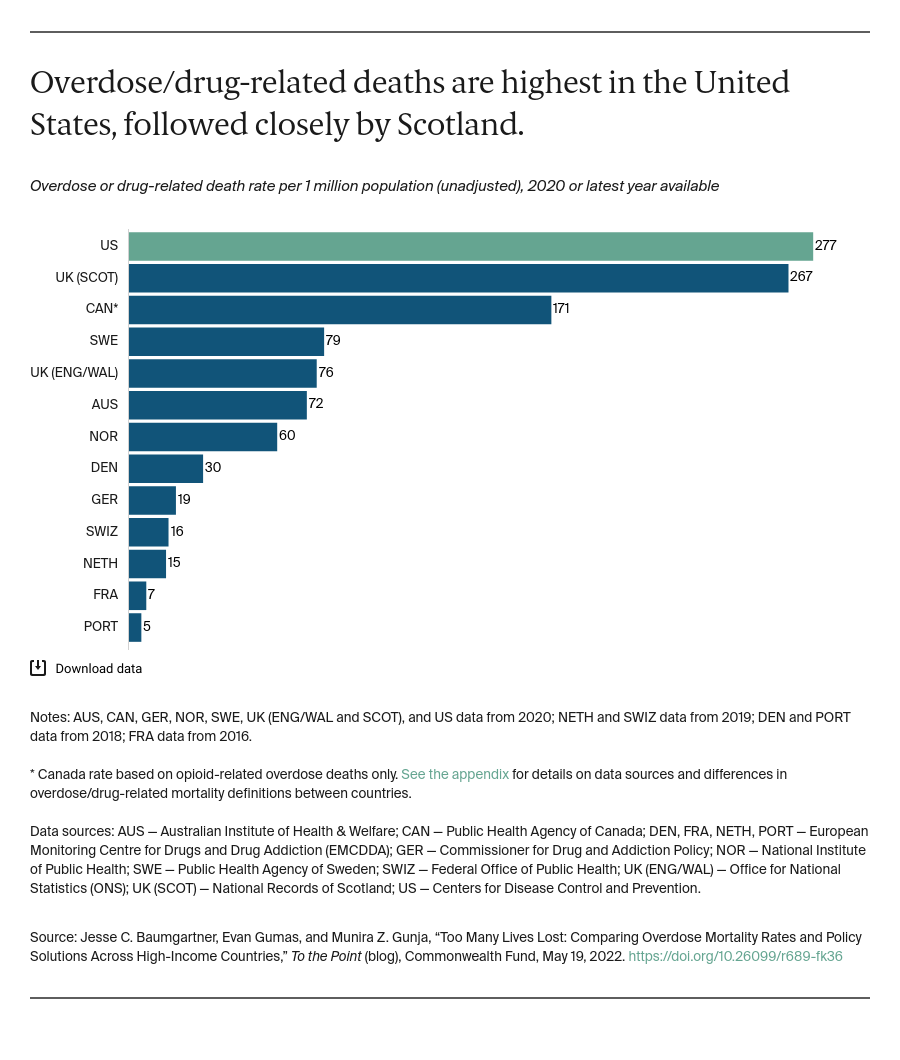
Overdose/Drug-Related Deaths Are Highest in the United States, Followed Closely by Scotland
Data released during the past year showed a dramatic increase in U.S. drug overdose deaths after COVID-19 emerged, with nearly 92,000 lives lost in 2020. Provisional data indicate that more than 105,000 lives were lost in 2021. Researchers have pointed to factors such as social isolation, addiction treatment interruption, and stronger synthetic opioids like fentanyl.
These staggering numbers are well above most international peer countries. Analysis of the latest publicly available data from each country finds that in 2020, the U.S. had the highest unadjusted rate of drug overdose deaths — 277 lives lost per million residents. Based on provisional data, the rate was likely near 320 lives per million residents in 2021. Scotland, which has long reported higher overdose mortality than the rest of the United Kingdom, is next at 267 deaths per million residents, followed by Canada with an opioid-related death rate of 171 deaths per million residents. In contrast, all other countries in the exhibit are below 100 deaths per million residents.
Many other countries also reported upticks in overdose deaths during 2020. While Canada stood out with a 77 percent increase in opioid-related deaths, rates for Germany and Norway started from a much lower level and increased by a lower percentage than the United States did. (See the appendix for 2019–2020 changes and differences in mortality data between countries.)