New digital health technologies — including remote sensors, communication platforms, and assistive devices — are shedding light on how frail elders are faring outside of hospitals and medical offices. Such tools allow health care providers to create a more realistic and immediate picture of the health and well-being of older adults, identify rising risks and adverse events, and discern patterns that can be used to design solutions for particular groups.
Starting next year, a team led by Jeffrey Kaye, M.D., a professor of neurology and biomedical engineering at Oregon Health and Science University, will begin tracking the activities of 360 older adults using a network of sensors they’ve agreed to place in their homes. With research partners in other parts of the country, his team will be monitoring the vital signs, medication use, mobility, activities, sleep patterns, and phone and computer use of a cross-section of Americans, including African Americans in Chicago, Latinos in Miami, public housing residents in Portland, Ore., and veterans in rural communities. One of his goals in tracking older adults who are still relatively healthy is to identify the early signs of physical and cognitive decline — generating insights that may guide medical care and enable patients to retain their independence.
Kaye began developing the platform, known as Life Lab, more than 10 years ago and with a team of researchers, statisticians, and software developers has been analyzing data from over 700 volunteers. Early findings have been surprising. For one, patients' own reports — which doctors rely on to help determine diagnoses and treatment plans — aren’t entirely reliable.1 Asked to explain what they did in the last two hours, a quarter were wrong and another third were only partially right. "They knew we had the data on what they were doing, and they weren’t cognitively impaired," Kaye says. "They just couldn’t remember accurately what they’d done." Another finding was that patterns in movement and behavior seemed to track cognitive impairment. For example, variable walking speed, less time spent away from home, and less time spent on computers “individually and together create a very strong signal that the person is in the early stages of cognitive decline," he says.
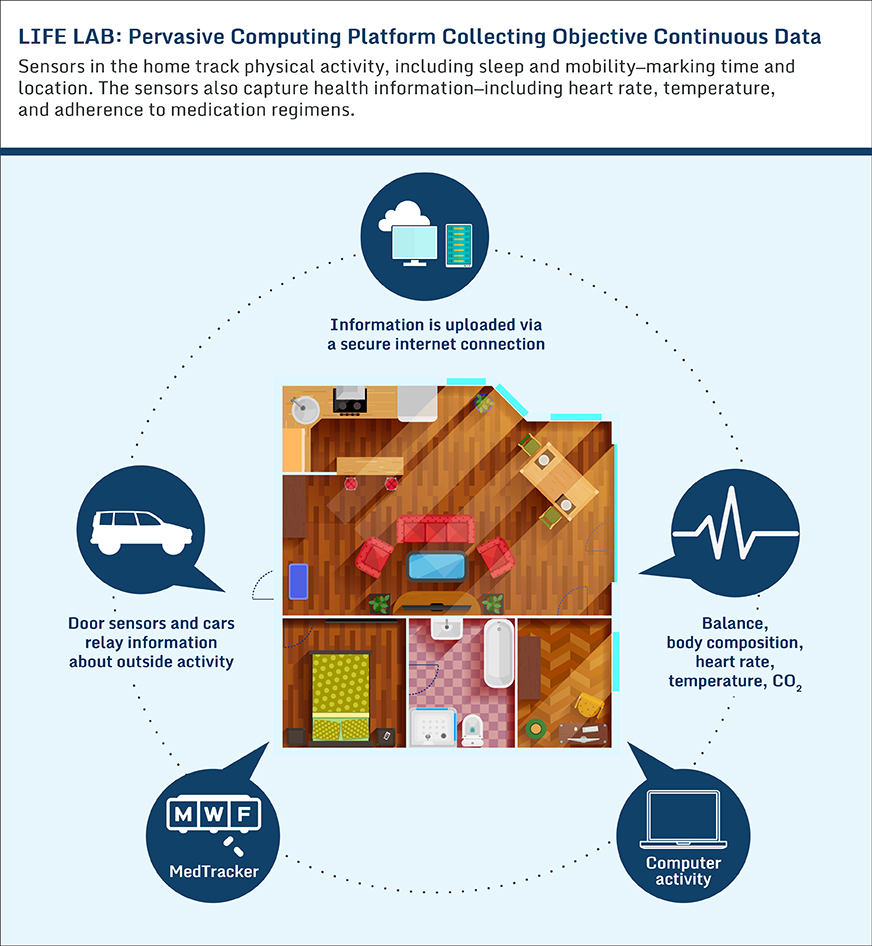
This issue of Transforming Care looks at the potential for a wide variety of emerging technologies to not just fill in knowledge gaps but help older Americans avoid falls, manage chronic disease, and reduce social isolation, among other goals. Many attempt to get beyond controlled medical environments and gather more points of data, filling in gaps that have created blind spots, particularly for high-need patients. "In medicine we've been very focused on what's happening in the hospital and physician’s offices—creating action plans based on that—but what happens there is not necessarily reflective of what happens to the patient at home and in daily life," says Adam Darkins, M.D., who helped develop and scale telehealth at the Veterans Health Administration before joining the medical device and technology company Medtronic. Indeed, Life Lab found that people tend to walk more slowly and cautiously at home than they do when demonstrating their gait in a doctor’s office.
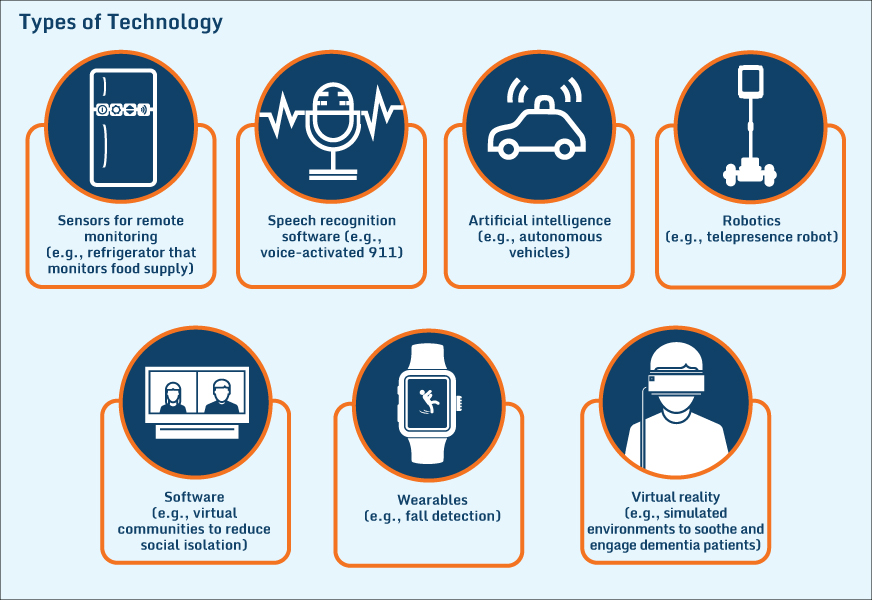
Technology Targets Leading Risks Among Older Adults
Preventing Falls and Other Adverse Events
The Miami, Fla.–based startup Care Heroes is one of a handful of companies seeking to leverage the insights of caregivers—either paid or unpaid—to help identify hazards in the home and frail elders who may be at risk.2 “We can now pull caregivers in as a core part of the care team—to recognize them and try to help them achieve what we all want to achieve, which is keeping frail elders out of the hospital or nursing home,” says Chiara Bell, Care Heroes founder and CEO. “We want to give them a voice.”
The tool creates a communication link between caregivers and health plan care managers. Caregivers use a phone-based app to report what they see and do, earning points for completing tasks and identifying hazards, such as a need for grab bars in a bathroom. They can then use the points to claim small prizes (e.g., $5 Target gift cards). Care managers receive caregiver reports immediately and can use them to address risks. The company will be aggregating the data to identify best practices for keeping members safe and help its clients distinguish and incentivize high-performing home care vendors.
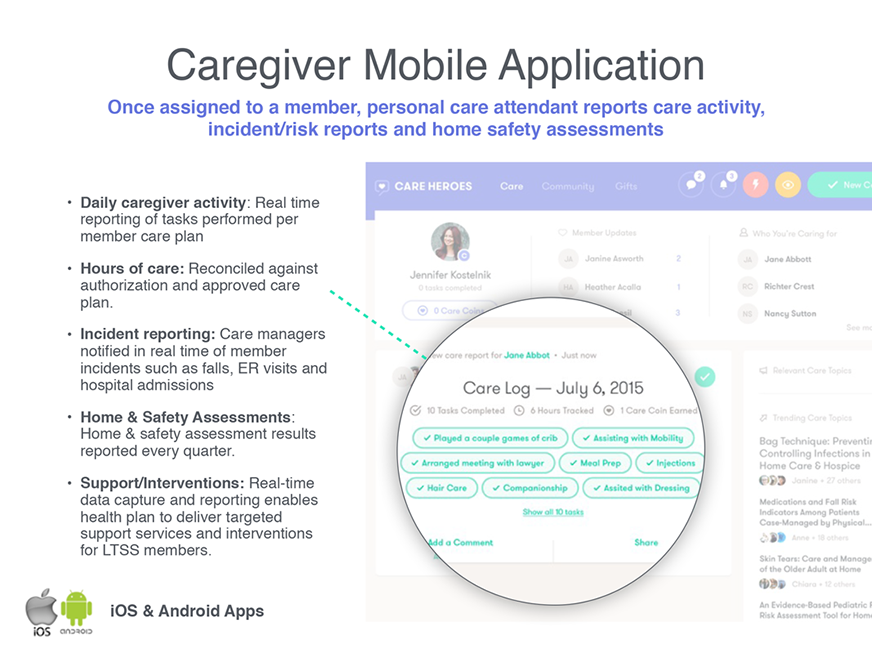
Source: Care Heroes
A key goal of monitoring approaches like Care Heroes and Life Lab is to identify when seniors begin to have problems with balance and other issues that put them at risk of falling, which is a leading cause of injury and injury-related deaths among older adults. Treating nonfatal falls alone cost Medicare nearly as much as treating all cancers last year.3 Some cities are treating falls as a public health problem: Baltimore City Department of Health, for instance, is analyzing data from the city’s health information exchange to identify the frequency and patterns of falls with a goal of offering support to those most at risk.
Other tools focus on the hospital environment.4 The technology and services company Philips is seeking to prevent falls by reducing the confusion and delirium that can be brought on by anesthesia or other aspects of hospitalization. It has developed four prototype rooms, now being piloted in a hospital in Germany, where most medical equipment is hidden from view. Clouds and other calming visualizations are projected onto a luminous ceiling, on which elders can use an iPad to play interactive games that help orient them to their environment. “We’re trying to turn the adult hospital world into the environment of the NICU, where we’re very sensitive to the needs of developing infants,” says Joseph Frassica, M.D., chief medical officer and chief innovation officer for Philips Healthcare.
Staff at Beth Israel Deaconess Medical Center are also working to alleviate the stress and confusion brought on by intensive hospital care. They’ve developed a tablet-based patient portal, MyICU, that offers educational and communication tools to patients’ families, including a journal to record daily events—visitors, tests, and progress made—to share with their loved ones later. “Patients can have post-traumatic stress disorder after an ICU stay,” says Barbara Sarnoff Lee, senior director of social work and patient/family engagement. “It has to do with their critical condition but also the drugs they’ve taken: they’re missing pieces of memory.” Journals can “help people put the pieces together,” she says, and have been shown to improve their adjustment after discharge.5
Promoting Evidence-Based Medicine, Treatment Adherence, and Chronic Disease Management
Other technologies seek to shape medical practice, promote treatment adherence and help older adults and their caregivers manage chronic conditions. More than a third of Medicare beneficiaries age 65 or older live with a chronic condition, and 15 percent live with six or more.6
A new startup, HealthReveal, collates and analyzes data from medical claims, electronic health records, pharmacy records, and lab results to find specific instances where a patient’s care is at variance with evidence-based literature—which research suggests occurs fairly often.7 It’s an approach that takes into account the difficulty of keeping abreast of medical literature and evolving clinical guidelines, and in particular of treating older adults who may have multiple comorbidities. The system is being implemented by self- insured employers and health systems to support physicians caring for patients with diabetes, cardiovascular disease, or kidney disease: three conditions that are “like the axis of evil” in that any one of them can prompt or exacerbate the other, says Lonny Reisman, M.D., the company’s founder.
HealthReveal plans to combine its decision support software with remote monitoring tools, so it can help track elders’ weight, blood pressure, and other biometric signals to alert physicians when they may need to intervene. It may also market its product to consumers, who are often unaware of widely varying quality of care.
Other companies have focused on remote monitoring tools that can track elders’ behavior—going beyond “smart” pillboxes and other wireless devices that have had an impact on disease management to an “internet of things” approach that embeds sensors in consumer products, such as refrigerators.8 One example is Samsung’s smart refrigerator, which can track how much food is inside and how often it’s opened—indicators of how well elders are taking care of themselves. Such innovations are more common in Japan and South Korea because they have large elderly populations and insufficient social supports, says David Bates, M.D., chief innovation officer and senior vice president at Brigham and Women’s Hospital. “It’s more of a burning platform in Asia.”
Dementia and Cognitive Declines: Supporting Patients and Caregivers
New technologies may provide the greatest benefit to older adults with Alzheimer’s disease or other forms of dementia—conditions that place considerable strain on their caregivers. An estimated 14 percent of Americans age 71 or older have Alzheimer’s disease or other forms of dementia, and 15 million Americans are providing them with unpaid care.9
Diane Mahoney, a geriatric nurse practitioner and researcher at Massachusetts General’s Institute of Health Professions, heard from caregivers of Alzheimer’s patients that they often struggled when helping their loved ones get dressed, particularly in the middle stage of the disease when elders wanted to dress themselves but were losing their ability to follow sequences. Working with occupational therapists and programmers, Mahoney developed a “smart dresser” system using an iPad, embedded sensors in dresser drawers, and wearable sensors that prompt elders through the steps of dressing and respond to their cues. “We can sense in real time where the person is at and what they are doing,” says Mahoney. “If they get stuck, the system gives a cue through the iPad to take out your shirt. It will show a picture and a voice will say, ‘That is the right shirt. Now put it on your right arm.’” The tool is able to assess each user and tailor response to their particular dressing patterns and cognitive issues. “This is really the breakthrough,” she says. “Usually programs are standardized, and the user must learn and adapt to the technology. We intentionally reversed this process to accommodate persons with dementia.”
The smart dresser is part of a growing number of assistive technologies that seek to support Alzheimer’s patients through daily activities, such as washing and exercising, or use interactive programs to stimulate their memories and encourage them to stay connected to others.10
Ameliorating Social Isolation
Finally, several researchers are testing whether technology can ameliorate another major risk for elders: social isolation, which some studies suggest can be as hazardous to health as smoking, obesity, or lack of exercise.11 The University of Miami Leonard M. Miller School of Medicine’s Sara Czaja, an expert on aging and human factors design, has worked with a team at the Center for Research and Education on Aging and Technology Enhancement to develop a computer software and training system for older adults. It provides a bundle of easily accessible features, including email, web browsing, and a curated set of community resources (e.g., Meals on Wheels, cultural events) as well as social networking opportunities. A pilot test among older adults who lived alone, had limited social interaction, and had minimal computing experience found that it reduced loneliness and increased their quality of life.12 “We had 98-year-olds sending email,” Czaja said.
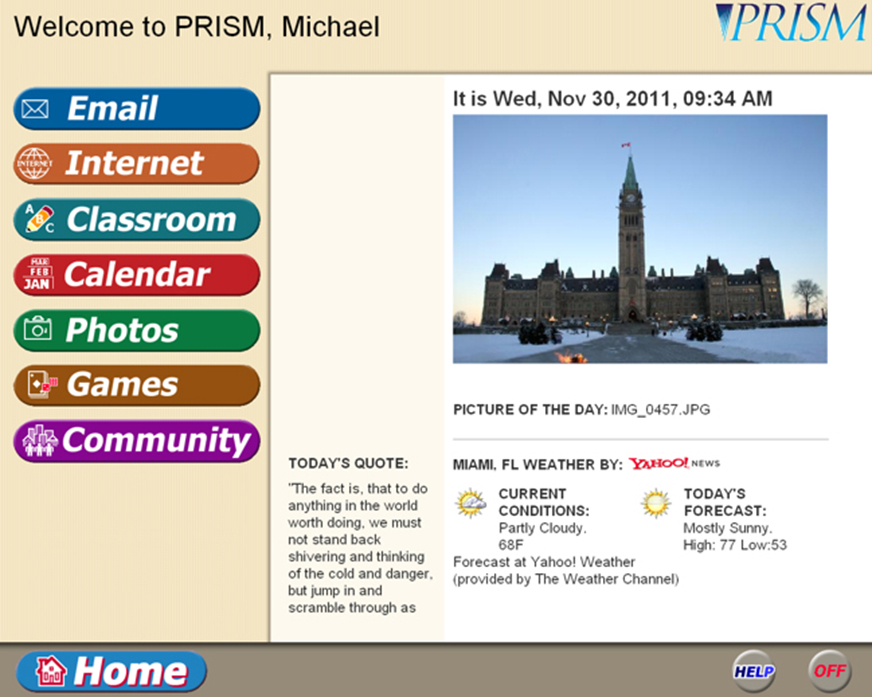
Source: Center for Research and Education on Aging and Technology Enhancement
Challenges
Need for User-Centered Design
To encourage adoption of new technologies by older adults (as well as their caregivers and clinicians), developers must do a better job in creating user-friendly products (see sidebar on user-centered design). A recent Commonwealth Fund–supported study found that users struggled with even the basic functions of high-ranked apps designed to manage chronic conditions.13 “They were frustrated with the design features and how to navigate the apps,” says Bates, who took part in the study. “At the same time, they were really interested in technology; they just felt what we were showing them—which was really best in class—didn’t meet their needs.”
To start, developers must ensure their user interfaces are accessible to those who may have vision or agility problems by creating large buttons, fonts, and clear navigation. Some developers are bypassing systems that require reading and typing in favor of voice-activated software that functions on traditional platforms, such as televisions.
There’s also lack of understanding of the real pain points because the industry is populated by young people, experts say. Too many technologies are driven by their creator’s personal experience, not market research. “I ask how many customers have you met with, and they say my grandma,” says Lisa Suennen, managing partner of the health care consulting firm Venture Valkyrie. To help developers understand the needs of those who could benefit most from digital health tools, the Commonwealth Fund and the Gordon and Betty Moore Foundation commissioned development of a prototype digital health advisor; its designers began by speaking with frail elders and their caregivers, among others.
To build understanding of seniors’ needs, the AARP has sought to engage the tech industry through several channels, including an annual demo day at which thousands of its members vote on pitches from tech developers. For four of the past five years, the consumers’ choice winner differed from that chosen by a panel of the venture capitalists. (Care Heroes was a consumers’ choice winner in 2014.) “We believe the innovation is going to come from start-ups,” says Jody Holtzman, senior vice president of market innovation at AARP.
Academic medical centers and other health systems have also set up innovation centers so that clinicians can work hand in hand with designers and developers in identifying needs and developing tools to meet them.14 Particularly for solutions that seek to promote behavior change to improve health, technologies must “be coupled with doctors’ knowledge about patients and what motivates them,” says Frassica. “If you build technology that supports intimate knowledge of patients, then you will win; without it, you will lose every time.”
User-Centered Design
Gretchen Addi, associate partner at IDEO, the design consultancy credited with reimagining the shopping cart, partners with health care providers and pharmaceutical companies as well as patients and their caregivers to develop products and services that better meet the needs older Americans. She encourages companies interested in reaching them to look beyond functionality to find solutions that bring joy and delight.

Gretchen Addi and Barbara Beskind, an IDEO fellow who draws on her background in occupational therapy to help design products for older adults. Photo credit: Nicolas Zurcher.
The starting point for us is always the human experience. We ask what do people need? What is missing for them? And where are they disconnected? We also look at extremes to find inspiration. In the aging space, this means talking to people who are incredibly isolated and people who have figured out how to be incredibly engaged. Often what we find is that they’ve co-opted a system or a service to make it work for them, and that’s where we see opportunities.
A lot of products and services that are out there for older adults send the message that aesthetics don’t matter, but if you want to engage people, they have to be desirable. That’s especially true in health care because people do not want to be reminded that they are sick or getting older. I’m as guilty of that as the next person. I’m 65, and if someone says this is a great product for older adults, I’m going to step away from it.

IDEO works to make assistive devices like walkers more desirable.
To find good ideas, we spend a lot of time talking to people and shadowing them to understand at a very core level what they are challenged by and how we can make their experience better by bringing design and joy to it. We don’t talk about designing for aging—we talk about designing for life stage and for needs that specific individuals have. Often it comes down to managing transitions. Take treatment adherence. As we see it, people who are struggling with a disease are moving through stages and need help with navigating them. It’s not simply having a better device for managing your medication. They need help adapting to new routines and help understanding that some of the emotional challenges they are experiencing are normal.
Technology can help by creating supports—either through communities of patients or with products and services that help reinforce new rituals and behaviors. These can benefit everyone because you don’t have to be old and frail to have this challenge. Think about using a bathroom mirror for instance. We’re in front of one multiple times a day so it’s already part of our routine. We have the technology to send messages through mirrors and relay those messages on things that are fun to carry with you. It doesn’t have to be a medical support device—it can be something that has a bit of personality to it. A cane is a good example. Most people don’t want to use them, but if they are decorated and personalized, they become a conversation piece and allow people to connect with others. Instead of being stigmatizing, it unites them with others.
There are physical transitions as well, which we don’t manage well in health care. When thinking about moving someone from his or her home to the health care environment and back, we encourage people to think in terms of a journey—not just for patients but for providers and caregivers as well. You must look at the specific needs and outcomes at each stage of the way and get into the mindset of those people and see where the disconnects are.
We can’t do this work without partnering closely with the people having the direct experience. One of our employees, Barbara Beskind, is a great example. She’s in her 90s and suffers from macular degeneration, so she’s trying to navigate the world while losing her sight. That spurred a lot of wonderful ideas, including eyeglasses that rely on facial or voice recognition to identify the person coming toward her. Based on her experience living in a retirement community, she’s also suggested using air bag technology in clothing to protect people from falls. By asking Barbara and others what their days are like, we gain insight about what’s needed and where the big opportunities lie.
Uncertain Funding Streams
Another major impediment to adoption of new technologies is figuring out who will pay for them. It’s not surprising that investors favor products that can be marketed directly to consumers because they’re wary of passing the evidentiary and regulatory hurdles required to secure reimbursement from Medicare or other insurers (see expert roundtable for discussion of the challenges). Foundations like the Alzheimer’s Association have stepped in to provide grants to fund research and development of products in places where they see market gaps, such as assistive technologies like Mahoney’s smart dresser. And cities like San Francisco have begun to address access barriers by providing low-income older adults with training, equipment, and subsidies to access the Internet, an essential component of many digital health technologies. “Internet access should be considered a health utility,” says Kathleen Kelly, executive director of the Family/Caregiver Alliance.
Health systems that are taking on financial risk for patient outcomes are also showing some interest, starting with tools that have been shown to work in managing expensive conditions like heart failure. And some of the larger health systems are using their investment funds to sponsor their innovation centers, accelerators, or other tech partnerships.
Need to Make Data Actionable
Many new technologies create new sources of data from wearable sensors and remote monitoring tools among other devices, and the key question is how to make it digestible and actionable to care providers. Platforms like IBM’s Watson and HealthReveal are starting to come to market to combine data from different sources and apply machine learning to make it manageable and useable.
And evidence is emerging that—when provided at the most opportune time and place—new sources of information gathered via technology can change care delivery. In a recent study, primary care clinicians who received a report summarizing whether their patients took their blood pressure medication, detected via an electronic pillbox that transmitted the time and date when it was opened, were more likely to intensify treatment among patients with uncontrolled hypertension.15
Realizing Value
Finally, it will be important to focus on technologies that stand to provide real value—and not to be distracted by the latest and greatest. “There’s a lot of spin and buzz about technology that’s exciting,” Kaye says. “And certainly, I’m as susceptible as anyone to the siren call of cool gadgets. But a lot of what is out there is still aspirational.”
Mahoney agrees. “People always want the next best thing, but there’s great opportunity to make common things work more reliably and cheaper. We still have a ways to improve while looking for the next best thing.”
Descriptions of products and services in Transforming Care are based on publicly available information and self-reported data provided by the institution(s) featured. Their inclusion should not be construed as an endorsement by The Commonwealth Fund.
Notes
1 K. V. Wild, N. Mattek, D. Austin et al., “‘Are You Sure?’” Lapses in Self-Reported Activities Among Healthy Older Adults Reporting Online,” Journal of Applied Gerontology, June 2016 35(6):627–41.
2 Other companies seeking to leverage the insights of caregivers include Care at Hand and Atlas of Caregiving.
3 M. Maciag, “How Governments Are Tackling a Deadly Threat to Seniors,” Governing, Nov. 21, 2016.
4 M. Ferris, “Protecting Hospitalized Elders from Falling,” Topics in Advanced Practice Nursing eJournal, 2008 8(4).
5 See C. Jones, M. Capuzzo, H. Flaatten et al., “ICU Diaries May Reduce Symptoms of Posttraumatic Stress Disorder,” Intensive Care Medicine, 2006 32 (Suppl 1):S144 and http://icu-diary.org/diary/Literature.html.
6 See https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Chronic-Conditions/MCC_Main.html.
7 See for example D. M. Levine, J. A .Linder, and B. E. Landon, “The Quality of Outpatient Care Delivered to Adults in the United States, 2002 to 2013,” JAMA Internal Medicine, Dec. 2016 176(12):1778–90 and J. C. Hsu, T. M. Maddox, K. Kennedy et al., “Aspirin Instead of Oral Anticoagulant Prescription in Atrial Fibrillation Patients at Risk for Stroke,” Journal of the American College of Cardiology, June 2016 67:2913–23.
8 For example, one study found that use of electronic pillboxes, coupled with the opportunity to be entered into a lottery for daily cash prizes, improved medication adherence and disease management. See K. G. Volpp, G. Loewenstein, and A. Troxel et al., “A Test of Financial Incentives to Improve Warfarin Adherence,” BMC Health Services Research, 2008 8:272–72. At Partners HealthCare, tracking heart failure patients through remote monitoring tools, along with efforts to promote behavior change, are credited with reducing hospitalizations related to the disease by 50 percent over several years. See A. Broderick, Partners HealthCare: Connecting Heart Failure Patients to Providers Through Remote Monitoring (New York: The Commonwealth Fund, Jan. 2013).
9 See https://www.alz.org/documents_custom/2016-facts-and-figures.pdf.
10 For examples, see E. Dishman and M. C. Carillo, “Perspective on Everyday Technologies for Alzheimer’s Care: Research Findings, Directions, and Challenges,” Alzheimer’s and Dementia, 2007 3:227–34 and http://www.alz.org/national/documents/etac_proceedings.pdf.
11 J. Holt-Lunstad, T. B. Smith, and J. B. Layton, “Social Relationships and Mortality Risk: A Meta-Analytic Review,” PLoS Medicine, 2010 7(7):e1000316.
12 Forthcoming, The Gerontologist.
13 U. Sarkar, G. I. Gourley, C. R. Lyles et al., “Usability of Commercially Available Mobile Applications for Diverse Patients,” Journal of General Internal Medicine, published online July 14, 2016.
14 M. Hostetter, S. Klein, D. McCarthy, S. L. Hayes, Findings from a Survey of Health Care Delivery Innovation Centers, (New York: The Commonwealth Fund, April 2015).
15 I. M. Kronish, N. Moise, T. McGinn et al., “An Electronic Adherence Measurement Intervention to Reduce Clinical Inertia in Treatment of Uncontrolled Hypertension: The MATCH Cluster Randomized Clinical Trial,” Journal of General Internal Medicine, Nov. 2016 31(11):1294–1300, http://link.springer.com/article/10.1007/s11606-016-3757-4.




