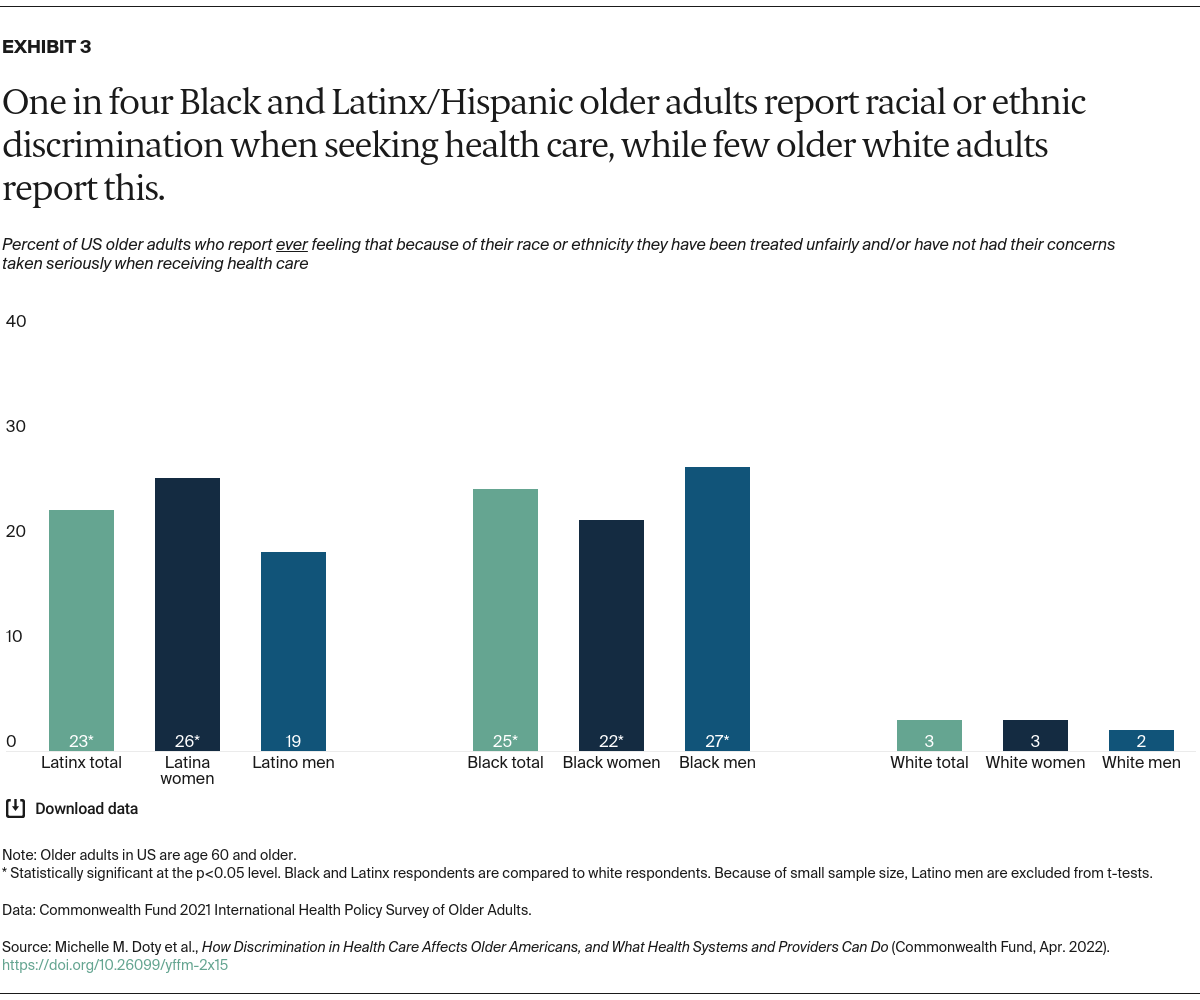
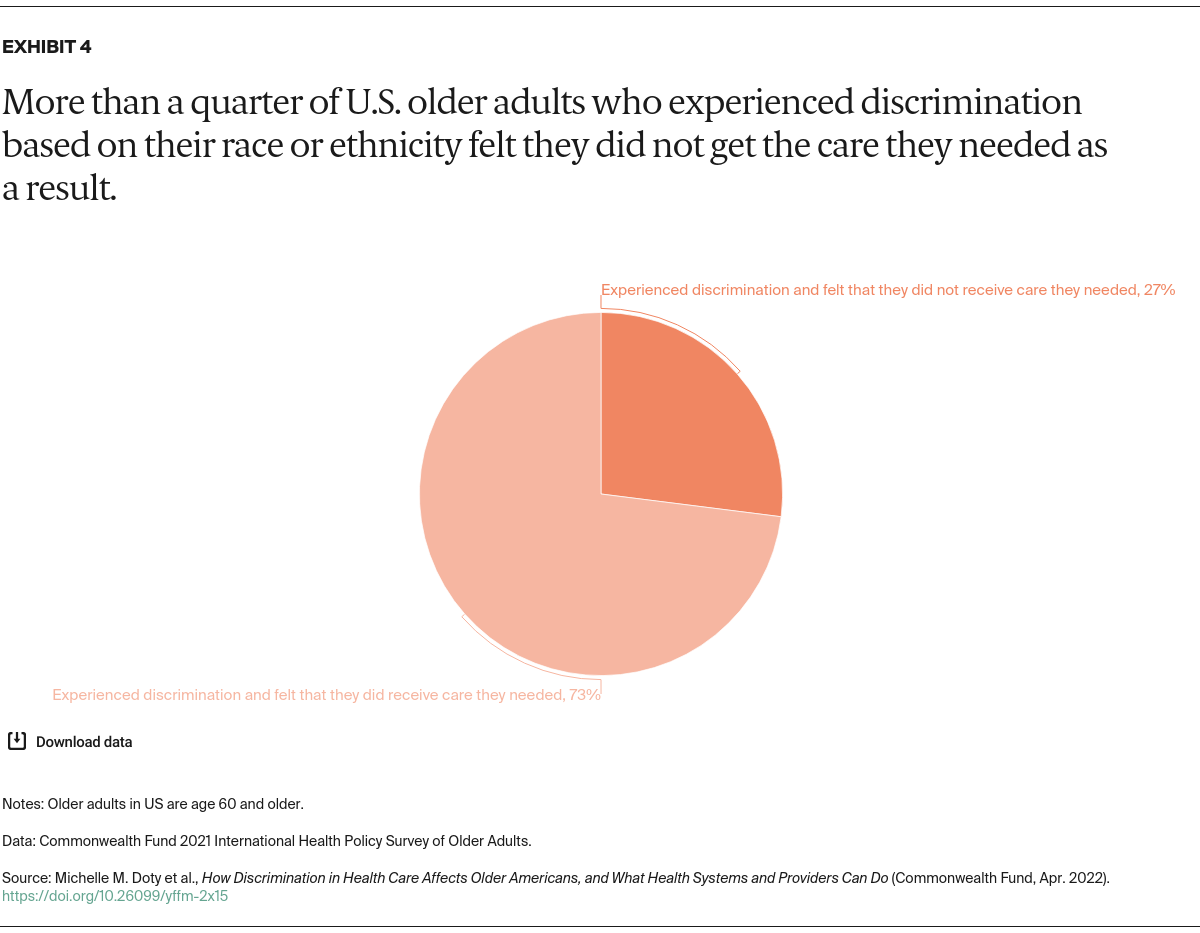
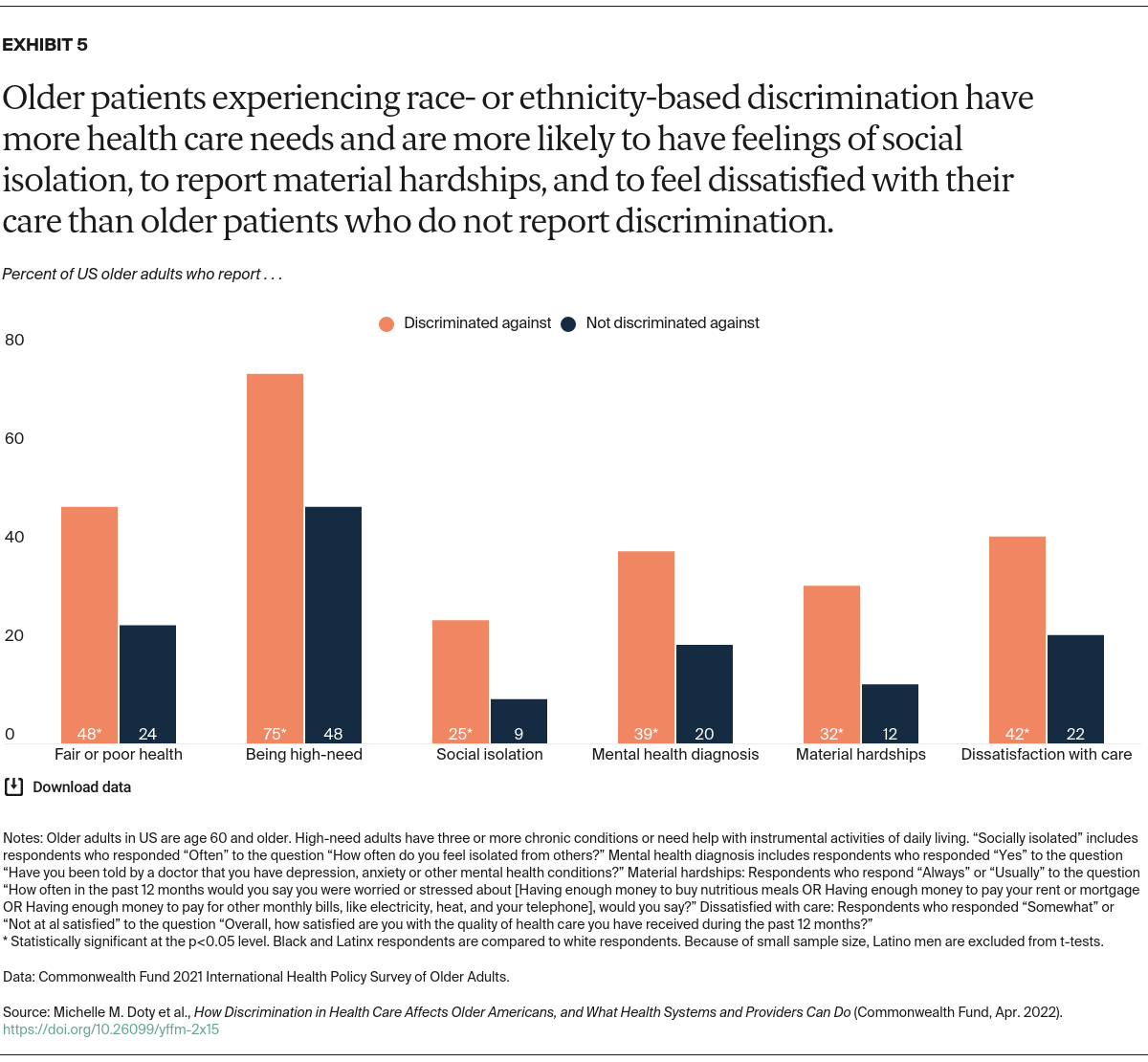
The majority (61%) of U.S. older adults who said that they experienced discrimination based on their race or ethnicity were Black or Latinx (data not shown). Nearly half of those who experienced such discrimination reported being in fair or poor health, twice the rate of those who did not experience discrimination. In fact, three-quarters of adults who have felt discriminated against have three or more chronic conditions or need help with daily activities (data not shown). Older adults who have faced discrimination based on their race or ethnicity are also significantly more likely to feel socially isolated, have a mental health diagnosis, and experience a material hardship (always or usually feeling stressed about having enough money to pay for food, housing, or monthly bills).
Older adults who have felt discriminated against when receiving care are significantly more likely to be dissatisfied with the quality of their care than those not reporting discrimination.9 More than four in 10 respondents who reported discrimination said they are somewhat or not at all satisfied, about double the rate for those who did not report discrimination.
Consistent with previous research, older Black and Latinx/Hispanic adults are more likely than older white adults to report being in fair or poor health and to experience material hardships (data not shown).
Policy Recommendations
Battling discrimination throughout the health care system is imperative to advancing health equity. Given that older adults use far more health care services than do younger people, and that the U.S. population is rapidly aging, addressing discrimination in health care settings is especially important for older adults of color. Ending discrimination and racism in health care begins with recognizing it and then actively working to dismantle it. Following are recommendations for spurring and supporting such efforts.
Promote transparency and accountability by identifying instances of discrimination and publicly reporting discrimination data. One way is to provide patients with the opportunity to report experiences of racism or other types of discrimination when completing standard patient satisfaction surveys. Health care organizations could expand existing patient experience surveys to ask about discrimination, bring these reports to the attention of system leaders, and identify opportunities for improvement. To promote accountability, health care organizations also could be required to publicly report responses.
Older adults of color, particularly those with health concerns, have many interactions with health personnel. Allowing them opportunities to reflect on how they were treated and to report their experiences with discrimination are important steps.
Develop medical school curricula to educate students about how the U.S. health care system has harmed patients of color and other historically marginalized communities. Studies have shown that medical students’ perceptions of race and implicit biases, together with false ideas of race-based biological differences, can affect their treatment recommendations for patients of color.10 The same is true for older patients: when medical students are exposed only to the sickest older patients in their training, they may adopt stereotypical thinking that affects treatment.11 To encourage their students to address bias, medical schools could teach the history of racism in the health system, institute implicit-bias training, and ensure that race is understood as a risk marker, not necessarily a risk factor, for health outcomes.12
Examine how current policies enable discrimination and then remove or reform those policies. Understanding how federal, state, and health care organizations’ policies and care delivery approaches enable discrimination and racism is an important step in diagnosing and treating racism in the health system at large.13 The National Academies of Sciences, Engineering, and Medicine is currently reviewing federal policies that promote health disparities, but private institutions could also systematically review their policies and practices to determine if and how they harm persons of color.14
Address the lack of diversity in the U.S. health care workforce. A diverse health care workforce can help promote the cultural competency of providers and improve access to health care, since providers of color are more likely to work in underserved communities, including those with large elderly populations.15 Providers whose racial or ethnic background reflects that of their patients can also engender greater trust. To foster diversity, medical schools could show how they are seeking to improve diversity among faculty and students, evaluate the diversity and experiences of those on recruitment committees, and target community colleges, historically Black colleges and universities, and Hispanic-serving institutions in their recruitment.16
Provide culturally and contextually appropriate care that addresses patients’ communication needs and preferences. All patients should have the opportunity to receive care the reflects their cultural values and language needs. To provide such care, organizations can offer translation services and create medical forms in multiple languages and provide cultural competency training to staff.17 Organizations also could work with the communities they serve to ensure care delivery reflects the needs and preferences of the community.
By taking these steps, health care organizations can do their part to address discrimination against older and younger adults alike to improve health equity and outcomes.