This case study is the second in a series profiling how primary care clinics — federally qualified health centers, independent clinics, and clinics that are part of large health systems — are meeting the needs of patients with low incomes. The series profiles clinics that exhibit some or all of the following attributes:
- medical home capabilities as a foundation
- multidisciplinary teams with community health workers
- integration of primary health care with public health, social services, and behavioral health
- using data to manage and improve patient care and clinic performance
- geographic empanelment, including appropriate risk stratification and targeting
- proactive patient and family engagement to address physical, social, and cultural barriers to care, and
- leveraging of digital tools to improve health.
CareSouth Carolina stands out for its efforts to field staff and services in people’s homes, schools, and churches to address their medical and social needs.
Background
Communities in the Pee Dee region along the coastal plains of South Carolina were already suffering, and then came the storms. In the last few years, powerful hurricanes have destroyed crops, washed out roads and bridges, and generally made lives more complicated in a region already marked by high poverty rates and poor health.
By knocking out major thoroughfares, the hurricanes also have made it harder for CareSouth Carolina, a federally qualified health center (FQHC), to treat patients across this sprawling region. The FQHC operates 14 primary care clinics across five counties, reaching some 45,000 people, or about 12 percent of residents. The largest clinic is in Hartsville, a small town with a main street lined with boutiques and cafes. The others are in outlying regions where patients and their families have lived for decades; some are so rooted they won’t travel to see a doctor even 10 miles away.
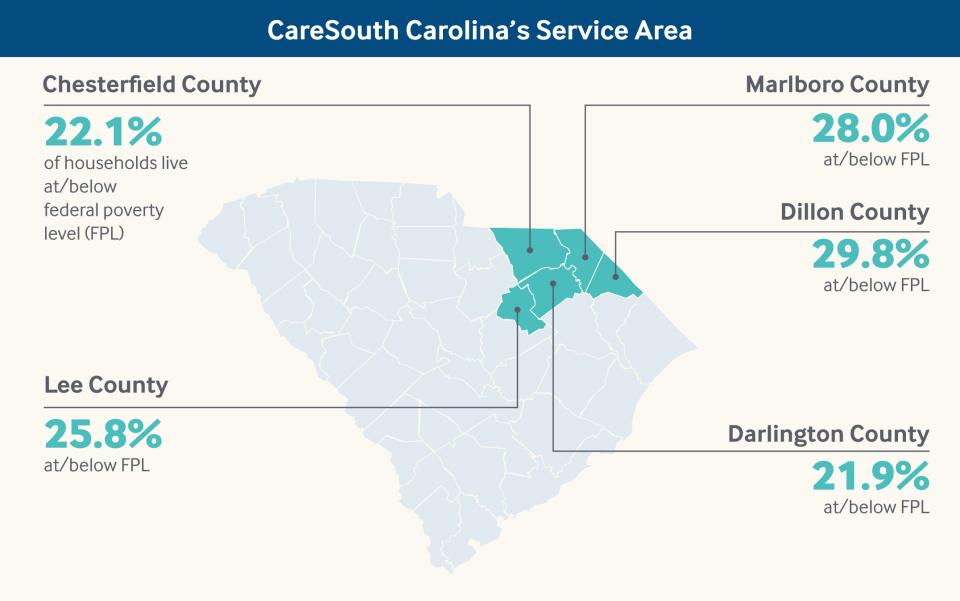
Data: U.S. Census Bureau, Small Area Income and Poverty Estimates (SAIPE) for Chesterfield, Darlington, Dillon, Lee, and Marlboro Counties, South Carolina, 1997–2017.
There is poverty here that is generational, that is just a way of life. No one even thinks that they’re in poverty.
“They’re little communities that people don’t get out of either because of habit, lack of transportation, or other barriers,” says Joe Bittle, CareSouth’s chief of community health.
Many patients live in severe poverty that extends across generations and struggle to afford basic necessities. CareSouth’s community health workers (CHWs) routinely visit homes where multiple families are living. Its dentists have treated children who don’t have toothbrushes. And clinicians once discovered that a child who’d repeatedly been to the emergency department for asthma exacerbations had been sleeping on the floor for lack of a crib.
This case study describes CareSouth’s efforts to overcome the geographic and economic barriers patients face in accessing primary care. These strategies include:
- Assigning community health workers to help people find safe housing, nutritious foods, and other social supports.
- Fielding medical assistants to help people manage prevalent chronic conditions, including hypertension, diabetes, and other cardiovascular conditions that put people at risk of stroke and other complications.
- Expanding access to behavioral health services, including treatment of opioid use disorder.
- Partnering with community groups to bring resources like health coaching to the region.
- Joining with other FQHCs to pursue value-based payment and using incentives earned from Medicaid managed care companies to finance additional services.
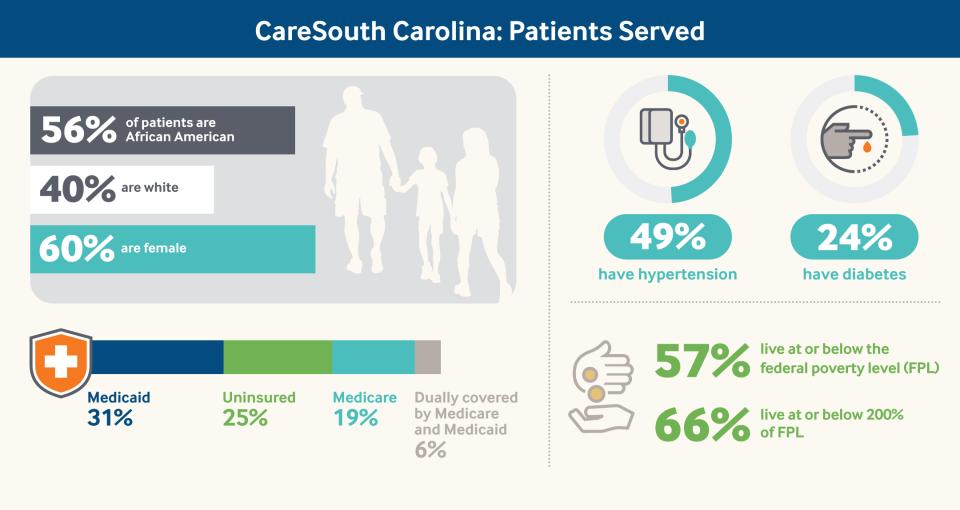
Data: “2018 CareSouth Carolina, Inc., Health Center Program Awardee Data,” UDS Data Comparisons (Health Resources and Services Administration, 2018).
Bringing Support Services into the Community
CareSouth was founded in 1980 to help meet the need for primary care in the region. Since 2013, all of its clinics have been certified by the Joint Commission as patient-centered medical homes — a testament to leaders’ efforts to field teams of physicians, nurse practitioners, nurses, medical assistants, and social workers across a vast service area, in some cases by using floaters who travel from clinic to clinic. In Lee County, CareSouth is the only health care provider.
To further extend its reach, CareSouth dispatches mobile units and sends clinicians into schools and churches. And for the past five years, it has relied on teams of community health workers and medical assistants to uncover patients’ needs and offer practical support. “Patients come in to medical visits dressed in their Sunday best,” says Brenda Petruccelli, one of CareSouth’s family support staff. “But when we go to their home, we can see they have no heat or air conditioning, or they might not have adequate food.”
CareSouth’s approach to engaging patients and helping them manage their conditions was shaped by its participation from 2012 to 2017 in the Robert Wood Johnson Foundation’s Learning from Effective Ambulatory Practices initiative. This program brought together leaders from 30 practices to explore ways to leverage their workforces to improve care quality, efficiency, and job satisfaction.
After speaking with other practice leaders from around the country, CareSouth’s CEO Ann Lewis realized her care management staff — who at the time were mainly nurses — could reach more people if they customized services to patients’ particular needs. “We realized we didn’t need to [provide the same] things to all people,” she says.
Bringing Services into the Community
Through the Miles of Smiles program, CareSouth’s dentists and hygienists travel to 35 schools in a mobile dental clinic that offers cleanings, sealants, and X-rays, reaching more than 2,000 children a year. (In the photo below, CareSouth Carolina CEO Ann Lewis stands in front of the mobile dental clinic.) The need is acute: teachers report that tooth pain is a leading cause of student absences, and dentists have had to extract children’s teeth and implant dentures because of severe problems. CareSouth also operates a dental clinic and sends another mobile dental van to treat adults at other sites.
The health center struggles to get adolescents to come to the clinics for well-child visits (just 30% of teens had one last year). To reach more teens, clinicians offer well-child services at 35 middle and high schools. And for the past four years, social workers have offered counseling to kids and teens in eight public schools. They work with about 300 students at a time, many with attention-deficit/ hyperactivity disorder or other behavioral issues and some who are coping with domestic violence or other problems at home.
The referenced media source is missing and needs to be re-embedded.
In 2015, the health center launched a three-tiered model of what it calls family support services. Patients’ needs are identified by their clinicians, medical record review, and a screening tool that assesses whether they have sufficient food, stable housing, and income and whether they’ve experienced trauma, violence, discrimination, or harassment. Those who appear to need help are then assigned an advocate, community health worker, or medical assistant, depending on their needs. In 2018, CareSouth’s 39 family support services staff members worked with 15,000 patients, logging some 75,000 visits, phone calls, or other interactions. They record their activities in patients’ electronic health records and offer updates to their clinicians during daily huddles.
Level 1 family support services staff serve as advocates, helping patients enroll in health insurance or other benefit programs and encouraging them to get vaccinations, cancer screenings, and other preventive care. In Hartsville, Ann Chapman recently helped a woman who had been diagnosed with multiple sclerosis and needed an MRI scan just after she lost her job and health insurance. Chapman was able to secure financial and other support for the patient through the Multiple Sclerosis Society.

CareSouth operates 14 clinics, with its largest in Hartsville. It relies heavily on nurse practitioners, who are easier to recruit than physicians and under South Carolina law can manage their own panels of patients.
Level 2 family support services staff are CHWs who offer health education and coaching to patients with moderate needs, such as those newly diagnosed with a chronic condition or those struggling to adhere to a treatment plan. They must complete a yearlong training course (which CareSouth helped develop) at a local community college that includes fieldwork and lessons on patient engagement tools such as motivational interviewing.
With some 12,000 hypertension patients and more than 6,000 diabetes patients, there’s enormous need. “It used to be, we could have a day where you could bring in all the patients who had diabetes, and you could do education,” says Randall Carlyle, chief quality officer. “It’s gotten to where now, every day is diabetes day.” CHWs also identify patients’ social needs and connect them with food banks, housing programs, and other sources of support. They share information about patients’ circumstances with clinicians, who can then make treatment recommendations as actionable as possible. “A lot of our patients are too proud to tell their clinicians about their problems,” says Carlyle. “But they may confide in a CHW. And getting a better handle on what’s going on with the patient outside of the visit has been key for our providers.”
Level 3 family support services staff are medical assistants who assist people with greater medical needs, most of whom have diabetes and/or hypertension, and many wind up in the emergency department or hospital from complications of their chronic conditions. The medical assistants offer them hands-on support in managing medications as well as coaching to help them make changes, like finding affordable ways to exercise or adjusting their favorite recipes to make them healthier.
Petruccelli, a medical assistant, helped a man with uncontrolled diabetes and hypertension who had become isolated in his home, eating meals on his own instead of with his family. “I discovered he liked gardening and so we talked about how gardening gets him outside, and how what he’s growing will help him provide for his family. He felt very down about not being able to do that,” she says. After a few months, the man agreed to have a retinal eye exam to screen for diabetic retinopathy and reduced his A1c from a 14.7 to an 11.7 — better, but still elevated. “I was constantly in contact with him and eventually, he started having an occasional meal with his wife,” she says. “Once, he said to me, ‘You act like you care and want me to be healthy.’”
Life and Death in the Stroke Belt
CareSouth serves five counties that are part of what’s known as the “buckle” of the stroke belt: 153 counties in North Carolina, South Carolina, and Georgia where death rates from stroke have been twice as high as the rest of the U.S. for several decades.1 Researchers have identified several factors that may contribute to the problem, including worse access to health care services, lower quality of care, greater health risks (particularly hypertension and diabetes), greater behavioral risks (smoking and fatty, salty diets), environmental risks (certain minerals in the water and soil), and the effects of poverty and racism.
Along with the nation, South Carolina has made strides in recent years in reducing stroke deaths, mainly because of advances in treatment during the first crucial hours after an occurrence. Still, stroke rates in the state are the sixth-highest in the nation, and black residents are 43 percent more likely to die from stroke than white South Carolinians.2
Recognizing the signs of stroke and getting to the hospital quickly are key to reducing stroke mortality and morbidity; treatment is most effective within two hours of the start of symptoms.3 But many people in the Pee Dee region lack reliable transportation, and the nearest hospital is often miles away.4 Lack of information about strokes also may be part of the problem.5
Integrating Behavioral Health Services
CareSouth integrated its behavioral and physical health care services 25 years ago. At the time, patients often had to wait six weeks or longer for appointments at community mental health clinics, and many gave up before being seen. CareSouth began hiring its own counselors, mainly licensed clinical social workers, to offer behavioral health assessments and treatment. Today, each of the 14 clinics has a counselor. Primary care clinicians screen patients at all visits for signs of depression, substance abuse, and other behavioral health problems, and counselors reserve 15 minutes of each hour so they can offer immediate consultations if problems are detected.
Providing this level of access requires a large behavioral health team. CareSouth has built its pipeline by training social work interns from the University of South Carolina, many of whom return to work at CareSouth after graduation, and by giving staff time off to pursue master’s degrees in clinical social work.
CareSouth Carolina’s Health Literacy and Educational Assessment
Source: CareSouth Carolina.
Some people may be fatalistic about their disease. Maybe their mother or father was diabetic and died at 50. I sit down with them and say, ‘This is what is going to happen: you are going to lose your fingers, your toes unless you make a change.’ For some people this is a wake-up call. But you can’t talk to somebody that way unless you get to know them.
CareSouth’s approach to behavioral health services was shaped by its involvement, from 2001 to 2006, in one of the Health Disparities Collaboratives led by the Health Resources and Services Administration. The collaborative brought together 94 community health centers in an effort to reduce disparities in depression treatment and outcomes based on research that had shown that patients with low incomes were more likely than those with higher incomes to have depression but less likely to be treated.6 Participants in the collaboratives used the Patient Health Questionnaire (PHQ ) to screen all patients, at least annually, for depression; engage people in treatment; and track outcomes. CareSouth was one of seven centers that reduced patients’ depression symptoms and sustained the improvements over time.7
Still, it took more focused work to reduce racial disparities in depression control. In 2003, CareSouth’s black patients who screened positive for depression were 15 percent less likely to receive treatment than white patients; among those receiving treatment, medications were not being titrated up as needed. “I think we fell into the trap of thinking some patients have low incomes or unreliable transportation, so let’s not stress them by making them come in,” says Elizabeth Kershner, M.S.W., director of behavioral health. “And so, there was a big push to make clinicians aware of the disparity. We expect everyone to be able to get better, and it’s our responsibility to meet them where they are and give them the support they need.”
Kershner and her colleagues began auditing records to ensure everyone who screens positive on the PHQ receives a full psychosocial assessment, a treatment plan, and goals for care, and then deploying outreach staff to encourage them to come in for treatment. She also began tracking depression treatment and outcomes and sharing the data with clinicians in monthly reports. During the past year, CareSouth has closed the gap between black and white patients in terms of depression control.
Substance Abuse Treatment
In 2016, CareSouth began offering medication-assisted treatment (MAT) for opioid use disorder after being approached by the state’s drug and alcohol agency for help in coping with the opioid epidemic. At the time, no clinicians in the region offered MAT; today, 13 CareSouth clinicians have gone through the waiver process required to prescribe buprenorphine. Together, they treat about 800 patients a year.
Stephen Smith, M.D., medical director, was the first to step forward, and his success built the will for others to do so. “He tells a story about a whole family that showed up in his church in gratitude for having gotten their family back together through medication-assisted therapy,” says CEO Lewis. “He tells people, ‘Ain’t nobody gonna show up in my church to thank me for helping them lower their cholesterol.’”
In treating opioid use disorder, CareSouth has partnered with local drug and alcohol treatment providers who offer counseling to patients while they receive MAT. The health center recently launched a MAT van to make the rounds at three drug and alcohol treatment agencies so that people can undergo drug screenings, receive their medication, and take part in counseling in one place. “We’re hoping that we’ll reduce some barriers to access,” says Kershner.
Our culture here has been one of working together to solve problems. There’s enough for everybody to say grace over.
Forging Community Partnerships
CareSouth collaborates with county officials, nonprofits, and social service agencies to assess residents’ needs. In one such effort, the partners surveyed 1,300 residents about their health experiences and views. Forty-three percent said they were dissuaded from seeking medical care by the high costs of prescription drugs, and 32 percent pointed to other out-of-pocket health care costs.8
To encourage more people to seek care, family support services staff canvas neighborhoods to let people know CareSouth’s services are available to all, regardless of their ability to pay. (Like other FQHCs, CareSouth charges sliding-scale fees based on patients’ income; the average visit has a $10 copayment.) The health center recently created a fund to cover patients’ copayments for drugs to manage diabetes, hypertension, asthma, and mental health conditions. Any patient with family income at or below 200 percent of the federal poverty level ($25,750 for a family of four in 2019) is eligible for this assistance.
CareSouth is also a founding member of the Northeastern Rural Health Network, which in 2017 won a grant from the Duke Endowment to improve health in Dillon, Marlboro, and Chesterfield counties. Given broad latitude to figure out how to do so, members of the network adopted the Faithful Families curriculum, a national program in which health educators partner with church leaders to encourage parishioners to eat healthy and be active.
Collaborating with Other Community Health Centers
In 2008, CareSouth and 13 other South Carolina FQHCs (out of 22 in the state) formed the independent practice association Community Integrated Management in response to South Carolina’s decision to shift Medicaid beneficiaries from fee-for-service to managed care. Health centers were being inundated by overtures from managed care plans seeking to enter the market and needed help negotiating value-based contracts, according to Peter Leventis, CEO of CIMS.
Today, Leventis negotiates contracts with four Medicaid managed care plans that pay health centers per member per month (PMPM) fees, including an additional $1.50 to $3.00 PMPM to fund care management services, plus incentive payments if providers improve performance on measures of health care quality and cost.9 Each year, CIMS distributes the incentive payments to health centers based on their volume of patients and performance. It holds back funds when a health center falls short and uses the money to offer clinical training programs or other support.
This collaboration has enabled the health centers to leverage shared resources. Early on, CIMS members invested in a performance dashboard that has helped leaders make sense of the medical claims data they receive from health plans. They’ve also used the dashboard to generate lists of assigned beneficiaries they’ve never seen, so patients can be targeted for outreach. “Between 22 percent and 40 percent of those assigned to our health centers have never graced our doors,” says Leventis. Not only are many people missing out on preventive and primary care, but the FQHCs are held accountable for beneficiaries’ health care spending and outcomes, whether or not they treat them.
For the past four years, CareSouth has fielded three community health workers to three local hospitals, where they encourage people visiting the emergency departments to come in for primary care. This and other efforts seem to have been effective: While in 2018 about one-quarter of Medicaid beneficiaries assigned to CareSouth had never visited its clinics, by the first half of 2019 only 20 percent of beneficiaries have not visited.
Since 2018, CIMS members have held regular calls to compare performance reports and share strategies for closing gaps in care. CareSouth leaders visited two health centers that had created dedicated teams to focus on particular populations. Under the leadership of Jeniqua Duncan, D.O., M.B.A., associate medical director, CareSouth then created three teams: one focused on Medicare beneficiaries, another focused on Medicaid beneficiaries, and a third focused on overseeing specialist referrals and following up with all patients after hospitalizations or emergency department visits.
Performance Measures Reported to Managed Care Plans by CIMS Members
- Well-infant visits 0–15 months: six or more visits
- Well-child visits ages 3–6 years: one visit
- Adolescent well care ages 12–21 years: one visit
- Child and adolescent weight assessment and counseling
- Childhood immunization: appropriate before 2nd birthday
- Pap tests ages 21–64: every three years unless HPV
- Adult body mass index (BMI) screening and follow-up
- Tobacco use screening: received cessation counseling or on cessation medication
- Colorectal cancer screening
- Breast cancer screening: one every two years
- Asthma pharmacological therapy ages 5–64
- Controlled hypertension: adults ages 18–59 whose blood pressure was <140/90 mm Hg; adults ages 60–85 with a diagnosis of diabetes whose blood pressure was <140/90 mm Hg; adults ages 60–85 without a diagnosis of diabetes whose blood pressure was <150/90 mm Hg
- Diabetes HbA1c >9% or no measurement during year
- Diabetes retinal eye exam, dilated
- Diabetes annual microalbumin screening
- Prenatal patients beginning prenatal care in first trimester
Data: Community Integrated Management Systems (CIMS).
“Our care management staff had been doing so many things, it was sometimes difficult for them to prioritize,” says Duncan. “The new organization helps them become experts at engaging certain groups.”
For its 2017 performance (the latest data available) in managing Medicaid beneficiaries, CareSouth earned about $650,000 in incentive payments from the managed care plans. The additional funds have enabled the health center to pay for CHWs and other aspects of its family support services.
Assessing Impact
CareSouth uses a comprehensive scorecard to track performance by individual clinicians, each of its clinics, and the health center as a whole on a range of measures.
During the past year, the health center has improved its performance on some measures of preventive health screenings and services, such as tobacco use screening and counseling, weight screening and counseling for children and adults, and depression screening. Leaders attribute this recent progress to the creation of regular performance reports that have enabled them to track care gaps and to dedicated teams that focus on particular patients and goals.
In addition, the health center has been able to substantially increase the number of patients screened for colorectal cancer (from 21% in 2016 to 48% in 2018). It also has increased the number of patients screened for cervical cancer (from 31% in 2016 to 40% in 2018), though the health center remains in the bottom quartile of performance among health centers nationally on this metric. CareSouth still struggles in other areas, particularly in managing chronic conditions. About half of patients with hypertension (55%) had their condition under control in 2018 (the fourth quartile of performance), while 70 percent of patients with diabetes had the condition under control (the second quartile).10
To promote improvement, CareSouth offers financial incentives to clinical teams who’ve made progress in closing gaps in recommended care or chronic disease control. All team members share in the quarterly bonuses. “It’s not just clinicians who play a role,” says Carlyle, the chief quality officer. “It could be a front office person who is calling patients to get them to come in for a Pap smear. Staff who work in medical records and billing analysts share in the bonuses because their work helped you do it.”
Lessons
CareSouth Carolina’s experience offers lessons for other primary care providers working to engage low-income patients and support them in efforts to build healthier lives.
Services Must Move Beyond the Clinic
CareSouth has for decades worked to improve the quality of health services it provides. But to gain further traction and reach patients who don’t come in for care, leaders have moved services into the community. Along with operational challenges, there are financial challenges to doing so. Revenues from CareSouth’s pharmacy as well as its managed care contracts help pay for extra services, particularly the family support services staff. Grants from CareSouth’s charitable arm, as well as from health plans and foundations, fund the mobile dental and medical units. But bringing services to all who could benefit may be difficult without other sources of funding.
CareSouth has begun experimenting with telehealth as one way to scale its services. It plans to have telehealth equipment in schools, so clinicians can support school nurses in treating sick kids. And it hopes to train family support services staff so they can visit patients in their homes and facilitate virtual visits with providers.
Engaging People in Their Health Is Paramount
Even with outreach into schools, churches, and homes, CareSouth’s leaders are acutely aware they are not reaching all who might benefit from the health center’s services. Its greatest challenge is “to make health foremost in everyone’s mind,” says CEO Lewis. Overcoming some black residents’ distrust of health care institutions — rooted in the South’s history of segregation and infamous instances of racism in health care — are part of this challenge, Lewis says: “There are long, long memories associated with that.”
To pursue its goal of serving 10,000 more people by 2021, CareSouth has customized its engagement approaches. For example, certain staff members are focused on encouraging people to receive preventive services, while others are focused on helping people manage chronic conditions. To make further progress, the health center may need to further segment patients according to their life circumstances and needs and try more customized strategies for engaging those not coming in for care.
Still, the region’s pervasive poverty — and South Carolina’s decision not to expand Medicaid to more residents — means there is enormous need in the community. “Our five counties are stuck at the bottom on health rankings,” says CEO Lewis. “Something has got to change.”
Collaborations Can Strengthen Communities
CareSouth’s work has been amplified through its long-standing partnerships with other health care organizations as well as county agencies, nonprofits, churches, and others. Its partnership with other FQHCs, in particular, has leveraged more resources for patients and created a platform for policy discussions with health plans and the state. For example, CIMS has lobbied the state to make well-child visits a condition of school attendance (or at least sports participation) to engage more young people in care. “Where you’re really going to affect the health of the community is at that adolescent and that child visit,” says Bittle, chief of community health.
Partnerships will be key to future successes, says Foster, the chief operations officer. “Communities are left undone until groups come together. Nobody can do it alone.”
Acknowledgments
CareSouth Carolina: Joe Bittle, Rose Brown, Randall Carlyle, Ann Chapman, Jeniqua Duncan, Peggy Foster, Gary Herrington, Deloras Jackson, Elizabeth Kershner, Ann Lewis, Marianne Liebenberg, Nichelle Nichols, Brenda Petruccelli, and Stephen Smith. Northeastern Rural Health Network: Christian Barnes Young. Community Integrated Management Systems: Peter Leventis. Chesterfield County Coordinating Council: Margaret Plettinger Mitchell. Commonwealth Fund: Melinda Abrams, John Craig (retired), Douglas McCarthy, and Jeanne Moore.
Commonwealth Fund case studies examine health care organizations that have achieved high performance in a particular area, have undertaken promising innovations, or exemplify attributes that can foster high performance. It is hoped that other institutions will be able to draw lessons from these cases to inform their own efforts to become high performers. Please note that descriptions of products and services are based on publicly available information or data provided by the featured case study institution(s) and should not be construed as endorsement by the Commonwealth Fund.


