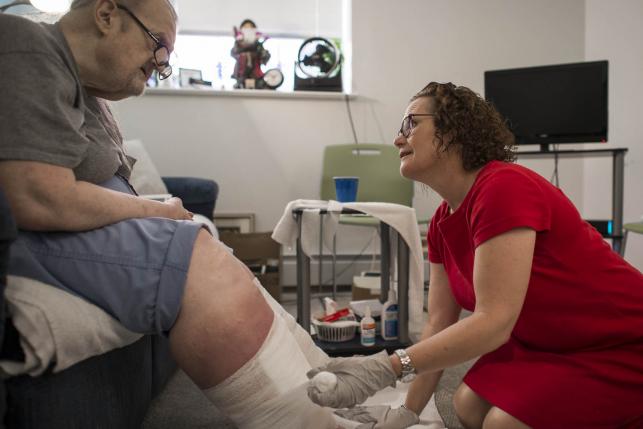
Vermont’s Bold Experiment in Community-Driven Health Care Reform
In 2014, Vermont encouraged the state’s largest payers — Medicare, Medicaid, and Blue Cross and Blue Shield of Vermont — to move more quickly from fee-for-service to risk-based contracting. The concept appealed to OneCare Vermont, a large accountable care organization (ACO) that had engaged more than half the state’s physicians and nearly all its hospitals in its network but had struggled to earn savings in its previous contracts with insurers. This case study examines OneCare’s community-driven approach to care coordination, which it piloted in 2017 among a subset (around 29,000) of the state’s Medicaid beneficiaries.